Chapter 99 VAGINOPLASTY—CONSTRUCTION OF NEOVAGINA
Reconstruction of the female perineum is indicated for congenital absence of the vagina, lymphedema, vaginal defects, previous ablative surgery for various perineal malignancies, relief of pain after radiation therapy, and repair of labial hypertrophy. Vaginal reconstruction has become a standard procedure performed by plastic surgeons, gynecologists, and urologists. The most common indication for vaginal reconstruction is congenital absence of the vagina.
Counseller1 reported that congenital absence of the vagina occurs in approximately 1 of every 4000 births and that these abnormalities usually coexist with uterus and urinary tract abnormalities. Usually, the ovaries are not affected, and the secondary sex characteristics develop normally. Embryologically, because the cervix and vagina initially form a solid unit, the lack of cavitation and cell death needed to form a vagina is the reason for vaginal agenesis.1 However, the hormonal factors that stimulate cavitation are unknown.
VAGINAL RECONSTRUCTION
History
In 1573, a student of Vesalius, Realdus Colombus, first reported vaginal agenesis, and it was not until 1872 that Heppner described vaginal reconstruction using the labia.2 However, the landmark report for vaginal reconstruction is credited to Abbe in 1898.3 In one patient, Abbe described dissecting a canal and lining it with split-thickness skin grafts.
These skin grafts were placed over a rubber stent packed with gauze. After 10 days, the stent was removed, and the skin grafts were completely vascularized. The patient was asked to wear a vaginal conformer postoperatively, and evidently, intercourse was possible. However, Abbe’s report was lost for almost 40 years, until McIndoe4 popularized the Abbe technique by lining the new vaginal canal with partial-thickness skin grafts. McIndoe reported an impressive array of 63 repairs,5 and in 1948, Counseller reported 70.1 Other methods of vaginal reconstruction have been attempted, but most have had undesirable effects, especially when segments of the gastrointestinal tract have been used for lining the new vaginal canal. In 1953, Conway and Stark6 described use of the rectum; earlier, Sneguireff,7 Popow,8 and Schubert9 had described the same thing. In 1904, Baldwin10 even described using a loop of ileum. However, obvious difficulties with bowel transposition such as necrosis, infection, and abscess formation occurred. If the procedure was successful, the secretions arising from the bowel lining were mostly inappropriate and unwanted. The added morbidity of an intra-abdominal procedure, various bowel anastomoses, the possibility of vascular compromise, and undesired mucosal secretions account for the lack of popularity of these procedures.
The Frank procedure, a nonoperative technique, has been successful in some instances of incomplete vaginal atresia. In 1927, Frank and Geist11 demonstrated the use of intermittent pressure at the perineal dimple between the anus and the urethra in the normal location of the vagina. This pressure is applied until the patient feels mild discomfort by a series of graduated obturators in the form of increasing sizes of test tubes. The pressure is relieved and then reapplied. The skin is inwardly stretched in the same way that a skin expander works with an outward force. This process continues for weeks until the largest dilator can be introduced within the neovagina and worn comfortably. This procedure requires a very compliant and persistent patient and an anatomy that is consistent with incomplete vaginal agenesis. The skin lining the new vagina is cutaneous squamous epithelium, and it must be lubricated externally to allow intercourse.
Surgical Techniques
Abbe-McIndoe Procedure
Over the years, the Abbe-McIndoe procedure evolved to become the easiest and most successful method of vaginal reconstruction, avoiding the risks and disadvantages of laparotomy (Figs. 99-1 and 99-2). The procedure must be performed under general or spinal anesthesia. A Y-shaped incision is made along the median raphe between the urethra and the anus. A catheter is placed in the urethra, and dissection is carried cephaloposteriorly. This dissection can be done relatively bluntly, and safety is ensured by keeping a gloved finger in the rectum for tactile ease of dissection. The Y incision allows three cutaneous flaps to be enfolded into the vaginal canal so that circumferential scar contraction can be avoided. The depth of dissection should be somewhat exaggerated and is in the range of 10 to 14 cm in the adult. The surgeon must overcorrect somewhat because of the expected subsequent contraction (Fig. 99-3).
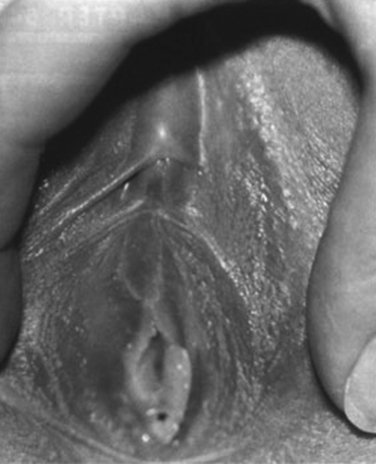
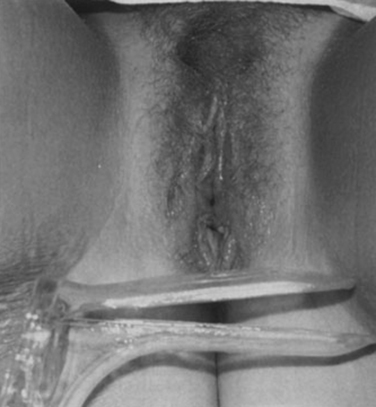
Figure 99-1 Congenital vaginal aplasia with an enlarged urethral meatus below the clitoris.
(From Lesavoy MA, Carter EJ: Vaginal reconstruction. In Raz S [ed]: Female Urology, 2nd ed. Philadelphia, WB Saunders, 1996, pp 605-616.)
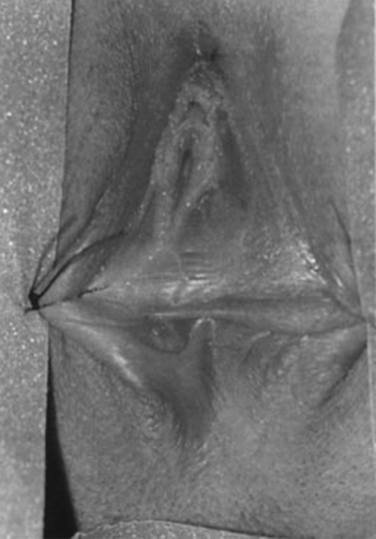
Figure 99-2 Sutures holding the labia majora.
(From Lesavoy MA, Carter EJ: Vaginal reconstruction. In Raz S [ed]: Female Urology, 2nd ed. Philadelphia, WB Saunders, 1996, pp 605-616.)

Figure 99-3 Catheter in the urethra and dissection of the neovaginal canal.
(From Lesavoy MA, Carter EJ: Vaginal reconstruction. In Raz S [ed]: Female Urology, 2nd ed. Philadelphia, WB Saunders, 1996, pp 605-616.)
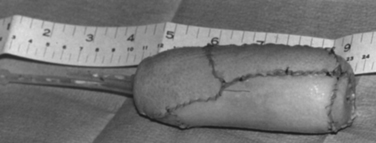
Several techniques have been developed to apply the skin graft to the vaginal canal. Historically, candle wax, carved balsa wood, gauze packing, syringe casing, dental wax, and hard plastic conformers have been used. The Heyer-Schulte Company has produced a soft, pliable, and expandable vaginal conformer that works very well. This stent has a central semirigid foam core and a surrounding silicone envelope that can be expanded with air or saline (Fig. 99-4). There is a central drain site through the core of the stent. After the graft has been harvested, the vaginal stent should be inflated with air and lubricated with mineral oil.

Figure 99-4 Heyer-Schulte inflatable vaginal stent.
(From Lesavoy MA, Carter EJ: Vaginal reconstruction. In Raz S [ed]: Female Urology, 2nd ed. Philadelphia, WB Saunders, 1996, pp 605-616.)
The skin graft sheets are sutured to each other and placed over the stent with the raw dermal sides out (Fig. 99-5). The epidermal side of the skin is adjacent to the stent. Subsequently, hemostasis is checked in the neovaginal canal, and the stent and overlying skin grafts are eased into the canal (Fig. 99-6). It may be necessary to deflate the vaginal stent while slowly rotating and pushing the stent and skin graft into the vaginal canal, but after the stent is seated to the depth of the dissection, it should again be inflated to spread out the skin graft, ensure direct apposition to the raw walls, and provide an excellent bolster for the ensuing neovascularization of the skin graft.
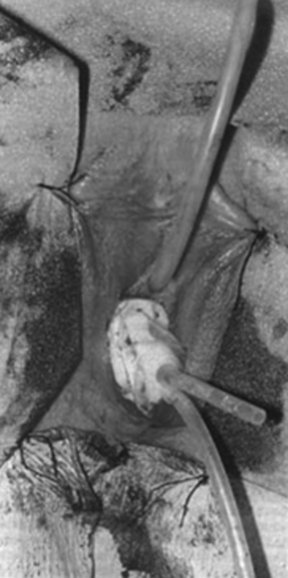
Figure 99-6 Vaginal stent with the skin graft invaginated into the neovaginal canal.
(From Lesavoy MA, Carter EJ: Vaginal reconstruction. In Raz S [ed]: Female Urology, 2nd ed. Philadelphia, WB Saunders, 1996, pp 605-616.)
Postoperatively, the patient remains in bed for a minimum of 5 days and is medically constipated (a lower bowel preparation is required preoperatively). On the fifth or sixth postoperative day, the patient is sedated in bed, and the labial sutures are removed. The skin graft can then be checked by aspirating the outer lumen of the Heyer-Schulte vaginal stent and deflating it, gently removing the stent, and leaving the skin graft intact within the vaginal vault. If there is any difficulty with this maneuver, mineral oil can be injected between the stent and the skin graft using a soft rubber catheter. This lubricates the interface between the stent and the skin graft so that disruption and shearing of the skin graft are avoided when the stent is removed. The perineum can be cleansed, and the stent can be washed and replaced immediately. Subsequently, a perineal binder can be applied, and the patient can be allowed to ambulate; the constipating medicine is then discontinued.
After vaginal reconstruction, a conformer must be worn for a minimum of 6 months postoperatively. If this is not done, contraction of the vaginal vault will ensue. After 3 or 4 months, as the skin graft matures, vaginal intercourse should be encouraged. This procedure should not be done unless intercourse is anticipated. Intercourse provides an excellent obturator and conformer. After 6 months, the conformer can be eliminated during the day but should be worn at night. If the patient is active sexually and has intercourse two to three times per week, the conformer can be eliminated. However, if there is a time when intercourse is not anticipated for weeks or months, the conformer should be worn at night (Figs. 99-7 to 99-10). Because the skin grafts do not have the same properties as normal vaginal mucosa and do not have secretory abilities, most patients require the application of lubricants before intercourse.30,31
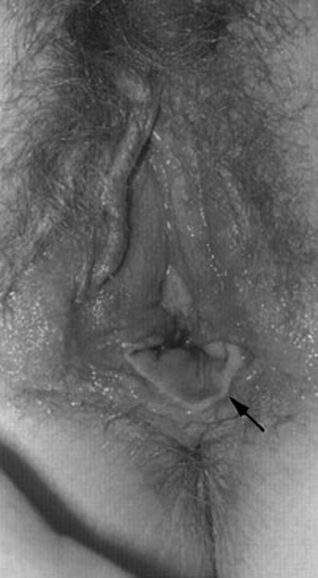
Figure 99-8 Discrepancy in the skin graft color of the neovagina.
(From Lesavoy MA, Carter EJ: Vaginal reconstruction. In Raz S [ed]: Female Urology, 2nd ed. Philadelphia, WB Saunders, 1996, pp 605-616.)
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree