Chapter 1 The History of Gastrointestinal Endoscopy
Early Efforts
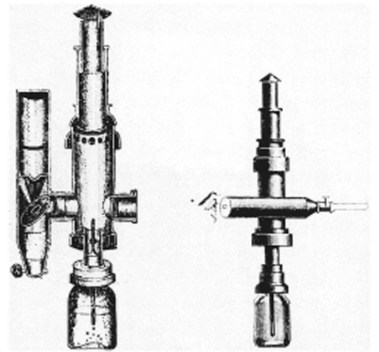
Bozini is credited with the earliest known attempt to visualize the interior of a body cavity with a primitive endoscope (Fig. 1.1). He published his work in 1805.1–3 Bozini devised a tin tube illuminated by a candle from which light was reflected by a mirror, a device he called a lichtleiter (light conductor). He used this device to examine the urethra, urinary bladder, and vagina, but it was an impractical instrument that never gained wide acceptance. Although there were multiple attempts to develop more usable instruments, all directed toward the GU tract, none were widely used. The most notable efforts were by Segalas in France in 1826 and Fisher in Boston in 1827,2 both using straight metal tubes, but the lack of a satisfactory light source remained a major impediment.

Fig. 1.1 Bozzini’s lichtleiter, 1805.
(From Edmonson JM: History of the instruments for gastrointestinal endoscopy. Gastrointest Endosc 37:S28, 1991.)
The next significant development was the instrument of Desormeaux in France.2 Desormeaux’s contribution in 1855 was a better, although still inadequate, light source using a lamp fueled with alcohol and turpentine (“gazogene”) (Fig. 1.2). His instrument was based on that of Segalas. Others continued with efforts to improve the light source and the means to deliver it, but the devices were unsatisfactory for the more inaccessible areas of the GI tract.
Rigid Gastrointestinal Endoscopes
Kussmaul is credited as being the first to perform gastroscopy in 1868, using a straight rigid metal tube passed over a flexible obturator and a cooperative sword swallower (Fig. 1.3).1–4 For a light source, he used a mirror reflecting light from the Desormeaux device but found it inadequate. He also quickly discovered that gastric secretions were a problem, despite using a flexible tube he had developed earlier to empty the stomach before the procedure. The value of his efforts was the demonstration that the curves and bends of the esophagus and esophagogastric junction could be traversed with careful manipulation and that the gastric pouch could be visualized. Kussmaul apparently demonstrated his “gastroscope” several times, but the illumination was too poor to allow a clinically useful image,4 and he abandoned his efforts.

Fig. 1.3 Kussmaul’s gastroscope, 1868.
(From Edmonson JM: History of the instruments for gastrointestinal endoscopy. Gastrointest Endosc 37:S30, 1991.)
Encouraged by the efforts of Kussmaul, others switched their attention to developing esophagoscopes because the esophagus is much easier to visualize, and a less complex design than the gastroscope was required. The problems of perforation, at that time usually fatal, and of illumination remained major obstacles. Before the late 19th century, illumination of light reflected by a mirror into a straight metal tube continued to be used. As noted earlier, several light sources were developed, but the intensity left much to be desired. Several innovations were developed to solve this problem, including a burning magnesium wire, which produced a brilliant light but unacceptable heat and smoke. The most promising device seemed to be the brilliant light from a loop of platinum wire charged with direct current, introduced simultaneously by Bruck in Breslau and Milliot of Paris in 1882.2 Although the illumination was good, major difficulties were encountered with the considerable heat generated, necessitating a water cooling system, and the cumbersome batteries used for a power source. Nevertheless, the platinum wire device was an encouraging development and was used in several instruments that saw relatively wide use.
At the turn of the 20th century, Jackson, an otolaryngologist, also examined the esophagus and the stomach using a straight rigid tube and a distal electric light bulb, but few could match his talents in the GI tract. Under his influence, esophagoscopy was considered the exclusive province of ear, nose, and throat (ENT) departments in many community hospitals in the United States as late as the 1950s. The design of the esophagoscope remained a straight rigid tube, usually with a rubber finger–tipped obturator to make insertion safer. With the later addition of a 4× power lens on the proximal end and a distal incandescent bulb, various models were popular until the introduction of fiberoptics in 1961. The Eder-Hufford rigid esophagoscope (Fig. 1.4), introduced in 1949, was popular and still in use during my training in 1960–1962.
It was not until after 1900 that persistent efforts to develop a usable gastroscope were successful. All attempts to build a flexible instrument using a multiplicity of lenses were designed to be straightened after introduction and were fragile, easily damaged, and cumbersome. Straight tubes with simpler optics were useful, but perforations were still a problem.1 In 1911, Elsner introduced a rigid gastroscope with an outer tube through which could be passed a separate inner optical tube with a flexible rubber tip and side-viewing portal (Fig. 1.5). The rubber tip, previously used in the esophagoscope obturator, was more crucial than it might appear, for it seemed to be, along with the later addition of a flexible metal coil proximal to it, the single feature that reduced the rate of perforation. Elsner’s instrument worked as designed and was widely used, especially by Schindler, then in his native Germany, who called it the “mother of all instruments until 1932.”5
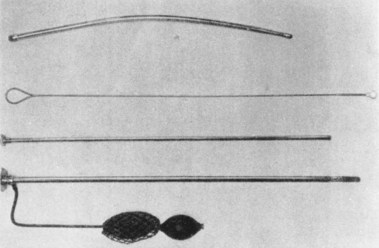
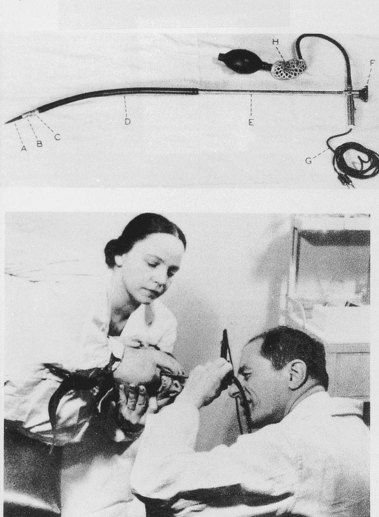
Fig. 1.5 Elsner’s gastroscope, 1911.
(From Edmonson JM: History of the instruments for gastrointestinal endoscopy. Gastrointest Endosc 37:S35, 1991.)
Semiflexible Gastroscopes
In 1911, Hoffman showed that an image could be transmitted through a curved line by linking several short-focus prisms. Using this principle, several instruments were constructed, but these were unsatisfactory or were not widely accepted. Schindler, working with Wolf, the renowned instrument maker, constructed a semiflexible instrument with a rigid proximal portion and a distal portion made elastic by coiled copper wire and terminating with first a rubber finger and later a small rubber ball. Illumination was with a distal incandescent light bulb. Air insufflation was made possible with a rubber bulb, expanding the stomach wall to beyond the focal length of the prisms, which were manufactured by Zeiss. In 1932, the sixth and final version was patented. This instrument, known as the Wolf-Schindler gastroscope, greatly improved the safety and efficacy of gastroscopy and was used throughout the world (Fig. 1.6).
Thanks to the published meticulous work and enthusiasm of Schindler, whose designation as the “father of gastroscopy” is well deserved, the procedure was finally widely accepted as a valuable extension of the physical examination. The era of the semiflexible gastroscope from 1932–1957 has been called “the Schindler era.” Schindler was chiefly responsible for transforming gastroscopy from a dangerous and seldom used procedure to one that was relatively safe and indispensable for evaluation of known or suspected disease of the stomach. He insisted that all clinicians who planned to use the instrument be properly trained and that “… no manipulation inside of the body is without danger; therefore no endoscopic examination should be done without reasonable indication.”6 In today’s vernacular, the risk approaches infinity if the benefit approaches zero.
Schindler was born in Berlin in 1888. He gained considerable experience as an Army physician in World War I, where he became convinced that gastritis, then an often disparaged cause of symptoms, was a bona fide disease. His interest in gastritis lasted throughout his career and undoubtedly stimulated his interest in gastroscopy. The Wolf-Schindler endoscope of 1932 and Schindler’s publications with drawings further enhanced what thereafter rapidly became a discipline. His enthusiasm for and talent in using the gastroscope led to what has been called his “gospel of gastroscopy,” which he and others spread throughout academia and to the community of practicing physicians. Because of his Jewish background, Schindler was put in “protective custody” by the Nazis, but with the help of the physicians Ortmeyer and Palmer and philanthropists in Chicago, he was able to immigrate to the United States in 1934.1–47
Chicago became the hub of GI endoscopy, and it was here, in Schindler’s home, that the first discussions were held about forming a new organization for GI endoscopy, now known, after several name changes, as the American Society of Gastrointestinal Endoscopy. In 1943, just 9 years after his arrival in the United States, Schindler left Chicago for Loma Linda University. In 1958, he accepted an appointment as Professor of Medicine at the University of Minas Gerais in Belo Horizone, Brazil. He came back to the United States in 1960 because of an eventually fatal illness of his wife and returned to his native Berlin in 1964, where he died in 1968 at the age of 80.1 Despite his acclaim in endoscopy, Schindler insisted that one must be a physician first and an endoscopist second. He was very knowledgeable in the field of general gastroenterology and published, without coauthors, a synopsis of the entire field in 1957.6
The Wolf-Schindler endoscope was introduced into the United States by Benedict, Borland, and many others. Schindler’s immigration to Chicago inspired a surge of interest in the United States, but with the outbreak of war in Europe, the German source of instruments disappeared. Several U.S. companies working with Schindler and others produced many popular gastroscopes that were significant variations on the Wolf-Schindler, including Cameron Co., which produced its first instrument in 1940.8 The Eder-Hufford semiflexible gastroscope followed in 1946,9 and American Cystoscope Makers, Inc. (ACMI) produced a gastroscope in 1950. A combination of the Eder-Hufford esophagoscope with a semiflexible gastroscope to be passed through it was the Eder-Palmer transesophagoscopic flexible gastroscope produced by the Eder Company in 1953. Each gastroscope had its proponents.
Biopsy
With the availability of instruments for visualization, it became apparent that tissue must be obtained to identify the nature of the observed abnormalities. Instruments for blind biopsies were used early on, but a device was needed that would allow the operator to obtain a biopsy specimen of abnormal tissue directly when seen at endoscopy. The Benedict Operating Gastroscope was produced in 1948 based on a 1940 model by Kenamore (Fig. 1.7).10
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree