Stone Disease
Kidney stones: epidemiology
What is the risk of de novo stone formation?
Previous editions of this book have stated that ˜10% of Caucasian men will develop a kidney stone by the age of 70. This is very much an average figure since lifetime stone risk is multifactorial, being dependent on a variety of intrinsic (inherent to the patient—sex, age, family history, comorbid conditions) and extrinsic factors (fluid intake, diet, lifestyle, climate, country of residence). In the United States of America (USA), the lifetime prevalence of stones is ˜12% for men and ˜7% for women. In other western countries, the lifetime risk is probably lower, but the gap between lifetime risk in the USA and that in other countries is probably narrowing as our lifestyles move closer to a USA one.
The prevalence of stone disease is increasing in all western societies. In the USA, the prevalence of stone disease increased from affecting 3.6% of the population in the period 1976-1980 to 5.2% between1988 and 1994.1 While some of this increase may reflect better diagnostic tests (e.g. the advent of CTU) diagnosing asymptomatic stones, much of this increase is likely to be real. Certainly in the UK, rates of treatment for stones have shown a very substantial rise over the last 10y at a time when there have been no substantial changes in technology or technique of stone treatment. Thus, the use of ESWL for treating upper tract stones increased by 55% between 2000 and 2010 with a 127% increase in the number of ureteroscopic stone treatments, 49% of this increase occurring between the periods 2007-8 and 2009-10.2
Of 5047 men and women (mean age 57y) undergoing CT colonography screening in 2004-2008 and with no symptoms of stone disease, a staggering 395 (7.8%) had stones (an average of 2 stones per patient, mean stone size 3mm).3 The prevalence in men was 9.7% and in women 6.3%, but was not (surprisingly) related to diabetes, obesity, and age >60. A substantial proportion of these initially asymptomatic stones became symptomatic over time. Over 10y of follow-up, 81 of these 395 patients (21%) went on to develop at least one symptomatic stone event.
What is the risk of recurrent stone formation in those who have already had a stone?
Once a stone has formed, the risk of future stone disease is very substantially increased. Within 1y of a calcium oxalate stone, 10% of men will form another calcium oxalate stone, ˜27-50% will have formed another stone within a mean of 7.54 to 9y.5
Once a second stone has formed, the frequency of recurrences increases and the interval between relapses becomes smaller.
Factors affecting stone formation
The prevalence of renal tract stone disease is determined by factors intrinsic to the individual and by extrinsic (environmental) factors. A combination of factors often contributes to risk of stone formation.
Intrinsic factors
The prevalence of stone disease and incidence of new stone events is increasing. Much of this change may relate to the epidemic of obesity sweeping western societies (obesity is associated with increased urinary excretion of stone-promoting substances, e.g. calcium, oxalate, uric acid, and decreased excretion of stone-preventing substances, e.g. citrate). Obese patients have a lower urinary pH which encourages urate stone formation.
Age: the peak incidence of stones occurs between the ages of 20-50y.
Sex: previous editions of this book have stated that males are affected three times as frequently as females, but the gender gap is closing, at least in the USA so that between 1997 and 2002, the male : female ratio for treated stones fell from 1.7:1 to 1.3:1.6 Testosterone may cause increased oxalate production in the liver (predisposing to calcium oxalate stones) and women have higher urinary citrate concentrations (citrate inhibits calcium oxalate stone formation).
Genetic: kidney stones are relatively uncommon in Native Americans, Black Africans, and American Blacks and more common in Caucasians and Asians. About 25% of patients with kidney stones report a family history of stone disease (the relative risk of stone formation remaining high after adjusting for dietary calcium intake). Familial renal tubular acidosis (predisposing to calcium phosphate stones) and cystinuria (predisposing to cystine stones) are inherited.7
Extrinsic (environmental) factors
Geographical location, climate, and season: the relationship between these factors and stone risk is complex. While renal stone disease is more common in hot climates, some indigenous populations of hot climates have a low incidence of stones (e.g. Black Africans, Aborigines) and many temperate areas have a high incidence of stones (e.g. Northern Europe and Scandinavia). This may relate to western lifestyle—excess food, inadequate fluid intake, limited exercise— combined with a genetic predisposition to stone formation.
Ureteric stones become more prevalent during the summer: the highest incidence occurs a month or so after peak summertime temperatures, presumably because of higher urinary concentration in the summer (encourages crystallization). The number of patients presenting acutely with urinary calculi increases by 2.8% for each degree increase in temperature and 0.2% for each hour increase in sunlight hours.8 Concentrated urine has a lower pH, encouraging cystine and uric acid stone formation. Exposure to sunlight may also increase endogenous vitamin D production, leading to hypercalciuria.
Water intake: low fluid intake (<1200mL/day) predisposes to stone formation9 and patients who relapse after experiencing a stone are less likely to have increased their fluid intake than those who remain stone-free. Increasing water ‘hardness’ (high calcium content) may reduce the risk of stone formation, by decreasing urinary oxalate.10
Diet: high animal protein intake increases the risk of stone disease (high urinary oxalate, low pH, low urinary citrate).11, 12 High salt intake causes hypercalciuria (through a sodium:calcium co-transport mechanism). Contrary to conventional teaching, epidemiological studies show that in populations, low calcium diets predispose to calcium stone disease and high calcium intake is protective.13
Occupation: sedentary occupations predispose to stones compared with manual workers.
1 Stamatelou KK, Francis ME, Jones CA, Nyberg LM, Curhan GC (2003) Time trends in reported prevalence of kidney stones in the United States: 1976-1994. Kidney Int 63:1817-23.
2 Turney BW, Reynard JM, Noble JG, Keoghane SR. Trends in urological stone disease. Br J Urol Int 2011.
3 Boyce CJ, Pickhardt PJ, Lawrence EM, Kim DH, Bruce RJ (2010) Prevalance of urolithiasis in asymptomatic adults: objective determination using low dose non-contrast computerized tomography. J Urol 183:1017-21.
4 Trinchieri A, Ostini F, Nespoli R, Rovera F, Montanari E, Zanetti G (1999) A prospective study of recurrence rate and risk factors for recurrence after a first renal stone. J Urol 162:27-30.
5 Sutherland JW, Parks JH, Coe FL (1985) Recurrence after a single stone in a community practice. Mineral Electrolyte Metab 11:267-9.
6 Scales CD, Curtis LH, Norris RD, et al. (2007) Changing gender prevalence of stone disease. J Urol 177:979-82.
7 Curhan GC, Willett WC, Rimm EB, Stampfer MJ (1997) Family history and risk of kidney stones. J Am Soc Nephrol 8:1568-73.
8 Lo SS, Johnston R, Al Sameraaii A, et al. (2009) Seasonal variation in the acute presentation of urinary calculi over 8y in Auckland, New Zealand. BJU Int 106:96-101.
9 Borghi L, Meschi T, Amato F, Briganti A, Novarini A, Giannini A (1996) Urinary volume, water and recurrences in idiopathic calcium nephrolithiasis: a 5-year randomized prospective study. J Urol 155:839-43.
10 Strauss AL, Coe FL, Deutsch L, Parks JH (1982) Factors that predict relapse of calcium nephrolithiasis during treatment. Am J Med 72:17-24.
11 Curhan GC, Willett WC, Speizer FE, Spiegelman D, Stampfer MJ (1997) Comparison of dietary calcium with supplemental calcium and other nutrients as factors affecting the risk for kidney stones in women. Ann Int Med 126:497-504.
12 Borghi L, Schianchi T, Meschi T, et al. (2002) Comparison of 2 diets for the prevention of recurrent stones in idiopathic hypercalciuria. N Engl J Med 346:77-84.
13 Curhan GC, Willett WC, Rimm EB, Stampfer MJ (1993) A prospective study of dietary calcium and other nutrients and the risk of symptomatic kidney stones. N Engl J Med 328:833-8.
Kidney stones: types and predisposing factors
Stones may be classified according to composition (Table 9.1), X-ray appearance, size, and shape.
Table 9.1 Composition of stones | ||||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| ||||||||||||||||
Other rare stone types (all of which are radiolucent): indinavir (a protease inhibitor used for treatment of HIV), triamterene (a relatively insoluble potassium-sparing diuretic, most of which is excreted in urine), xanthine.
Radiodensity on X-ray
Three broad categories of stones are described, based on their X-ray appearance. This gives some indication of the likely stone composition and helps, to some extent, to determine treatment options. However, in only 40% of cases is the stone composition correctly identified from visual estimation of the radiodensity on plain X-ray.3
Radio-opaque
Opacity implies the presence of substantial amounts of calcium within the stone. Calcium phosphate stones are the most radiodense stones, being almost as dense as bone. Calcium oxalate stones are slightly less radiodense.
Relatively radiolucent on plain X-ray
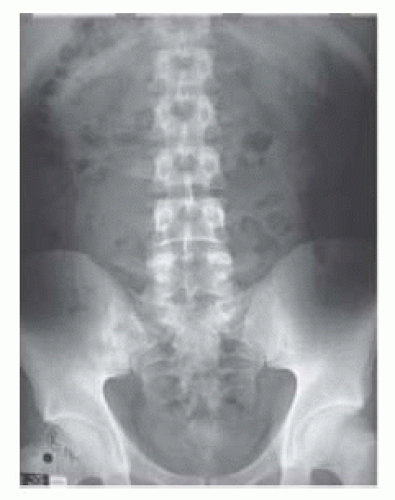
Cystine stones are relatively radiodense because they contain sulphur (Fig. 9.1). Magnesium ammonium phosphate (struvite) stones are less radiodense than calcium-containing stones.
Size and shape
Stones can be characterized by their size, in mm or cm. Stones which grow to occupy the renal collecting system (the pelvis and one or more renal calyces) are known as staghorn calculi since they resemble the horns of a stag (Fig. 9.2). They are most commonly composed of struvite— magnesium ammonium phosphate (being caused by infection and forming under the alkaline conditions induced by urea-splitting bacteria), but may be composed of uric acid, cystine, or calcium oxalate monohydrate.
1 Ramakumar S, Patterson DE, LeRoy AJ, et al. (1999) Prediction of stone composition from plain radiographs: a prospective study. J Endo Urol 13:397-401.
Kidney stones: mechanisms of formation
The driving force behind stone formation is the supersaturation of urine. Supersaturation is expressed as the ratio of urinary calcium oxalate (for example) to its solubility. Below a supersaturation of 1, crystals of calcium oxalate remain soluble. Above a supersaturation of 1, crystals of calcium oxalate nucleate and grow, thereby promoting stone formation.
Urine is said to be saturated with, for example, calcium and oxalate when the product of the concentrations of calcium and oxalate exceeds the solubility product (Ksp). Below Ksp, crystals of calcium and oxalate will not form and the urine is said to be undersaturated. Above Ksp, crystals of calcium and oxalate should form, but they do not because of the presence of inhibitors of crystal formation. However, above a certain concentration of calcium and oxalate, inhibitors of crystallization become ineffective and crystals of calcium oxalate start to form. The concentration of calcium and oxalate at which this is reached (i.e. at which crystallization starts) is known as the formation product (Kf) and the urine is said to be supersaturated with the substance or substances in question at concentrations above this level. Urine is described as being metastable for calcium and oxalate at concentrations between the Ksp of calcium and oxalate and the Kf (Box 9.1).
The ability of urine to hold more solute in solution than can pure water is due partly to the presence of various inhibitors of crystallization (e.g. citrate forms a soluble complex with calcium, preventing it from combining with oxalate or phosphate to form calcium oxalate or calcium phosphate stones). Other inhibitors of crystallization include magnesium, glycosamin-oglycans, and Tamm-Horsfall protein. From a practical perspective, the only inhibitor of stone formation that is open to manipulation is citrate.
Periods of intermittent supersaturation of urine with various substances can occur as a consequence of dehydration and following meals.
The earliest phase of crystal formation is known as nucleation. Crystal nuclei usually form on the surfaces of epithelial cells or on other crystals. Crystal nuclei form into clumps—a process known as aggregation. Citrate and magnesium not only inhibit crystallization, but also inhibit aggregation. Calcium oxalate stones form over a nucleus of calcium phosphate (Randall’s plaques on the surface of a renal papilla).
Box 9.1 Steps leading to stone formation
Calcium and oxalate concentration <A onclick="get_content(event,'AB3-M1'); return false;" onmouseover="window.status=this.title; return true;" onmouseout="window.status=''; return true;" title="< solubility product → NO STONE FORMATION.
Metastable calcium and oxalate concentrations → NO STONE FORMATION.
Calcium and oxalate concentrations ” class=LK href=”javascript:void(0)” target=right xpath=”/CT{06b9ee1beed594192fe83c602fef4af9a59e63f847d6df62927a64e26327cf0c0e58d45b6bfdac2767fce92dc3549f3a}/ID(AB2-M1)”>> formation product → STONE.
Factors predisposing to specific stone types
Calcium oxalate (˜85% of stones)
Although most patients with calcium oxalate stones have at least one metabolic abnormality (e.g. hypercalciuria, hyperoxaluria, hypocitatruria), the majority of calcium oxalate stones are idiopathic, i.e. the cause of that metabolic abnormality is unknown.
Hypercalciuria: excretion of >7mmol of calcium per day in men and >6mmol per day in women. The major metabolic risk factor for calcium oxalate stone formation is that it increases the relative supersaturation of urine. Some series suggest that as many as 50% of patients with calcium stone disease have hypercalciuria although the proportion of hypercalciuric patients in other series is lower. There are three types:
Absorptive: increased intestinal absorption of calcium.
Renal: renal leak of calcium.
Resorptive: increased demineralization of bone (due to hyperparathyroidism).
Diet has a major influence on hypercalciuria.
Hypercalcaemia: almost all patients with hypercalcaemia who form stones have primary hyperparathyroidism. Of hyperparathyroid patients, about 1% form stones (the other 99% do not because of early detection of hyperparathyroidism by screening serum calcium).
Hyperoxaluria: is due to the following.
Altered membrane transport of oxalate, leading to increased renal leak of oxalate.
Primary hyperoxaluria: increased hepatic oxalate production—rare.
Increased oxalate absorption in short bowel syndrome or malabsorption (enteric hyperoxaluria): the colon is exposed to more bile salts and this increases its permeability to oxalate.
Ascorbic acid and high protein intake increase oxalate production.
Hypocitraturia: citrate forms a soluble complex with calcium (so-called chelation), thus preventing the complexing of calcium with oxalate to form calcium oxalate stones. Distal renal tubular acidosis, hypokalaemia, and carbonic anhydrase inhibitors lead to hypocitatruria.
Hyperuricosuria: high urinary uric acid levels lead to the formation of uric acid crystals on the surface of which calcium oxalate crystals form.
Uric acid (˜5-10% of stones)
Humans (unlike birds) are unable to convert uric acid (which is relatively insoluble) into allantoin (which is very soluble). Human urine is supersaturated with insoluble uric acid. Uric acid exists in two forms in urine—uric acid and sodium urate. Sodium urate is 20 times more soluble than uric acid. At a urine pH of 5, <20% of uric acid is present as soluble sodium urate. At urine pH 5.5, half of the uric acid is ionized as sodium urate (soluble) and half is non-ionized as free uric acid (insoluble). At a urine pH of 6.5, >90% of uric acid is present as soluble sodium urate.
Thus, uric acid is essentially insoluble in acid urine and soluble in alkaline urine. Human urine is acidic (because the end products of metabolism are acid) and this low pH, combined with supersaturation of urine with uric acid, predisposes to uric acid stone formation.
Thus, uric acid is essentially insoluble in acid urine and soluble in alkaline urine. Human urine is acidic (because the end products of metabolism are acid) and this low pH, combined with supersaturation of urine with uric acid, predisposes to uric acid stone formation.
About 20% of patients with gout have uric acid stones. Patients with uric acid stones may have:
Gout: 50% of patients with uric acid stones have gout. The chance of forming a uric acid stone if you have gout is in the order of 1% per year from the time of the first attack of gout.
Myeloproliferative disorders: particularly following treatment with cytotoxic drugs, cell necrosis results in release of large quantities of nucleic acids which are converted to uric acid. A large plug of uric acid crystals may form in the collecting system of the kidney in the absence of ureteric colic, causing oliguria or anuria.
Idiopathic uric acid stones: no associated condition.
Calcium phosphate (calcium phosphate + calcium oxalate = 10% of stones)
Occur in patients with renal tubular acidosis (RTA)—a defect of renal tubular H+ secretion resulting in an impaired ability of the kidney to acidify urine. The urine is, therefore, of high pH and the patient has a metabolic acidosis. The high urine pH increases supersaturation of the urine with calcium and phosphate, leading to their precipitation as stones.
Types of renal tubular acidosis
Type 1 or distal RTA: the distal tubule is unable to maintain a proton gradient between the blood and the tubular fluid; 70% of such patients have stones. When the urine pH is >5.5, the patient has a metabolic acidosis and hypokalaemia, urinary citrate is low, and hypercalciuria is present.
Type 2 or proximal RTA: due to failure of bicarbonate resorption in the proximal tubule. There is associated increased urinary citrate excretion which protects against stone formation.
Type 3: a variant of type 1 RTA.
Type 4: seen in diabetic nephropathy and interstitial renal disease. These patients do not make stones.
If urine pH is >5.5, use the ammonium chloride loading test. Urine pH that remains above 5.5 after an oral dose of ammonium chloride = incomplete distal RTA.
Struvite (infection or triple phosphate stones) (2-20% of stones)
These stones are composed of magnesium, ammonium, and phosphate. They form as a consequence of urease-producing bacteria which produce ammonia from the breakdown of urea (urease hydrolyses urea to carbon dioxide and ammonium) and in so doing, alkalinize urine as in the following equation:

Under alkaline conditions, crystals of magnesium, ammonium, and phosphate precipitate.
Cystine (1% of all stones)
Occur only in patients with cystinuria—an inherited (autosomal recessive) disorder of transmembrane cystine transport, resulting in decreased absorption of cystine from the intestine and in the proximal tubule of the kidney. Cystine is very insoluble so reduced absorption of cystine from the proximal tubule results in supersaturation with cystine and cystine crystal formation. Cystine is poorly soluble in acid urine (300mg/L at pH 5, 400mg/L at pH 7).
Evaluation of the stone former
Determination of stone type and a metabolic evaluation allows the identification of the factors that led to stone formation so advice can be given to prevent future stone formation.
Metabolic evaluation depends, to an extent, on the stone type (Table 9.2). In many cases, a stone is retrieved. Stone type is analysed by polarizing microscopy, X-ray diffraction, and infrared spectroscopy rather than by chemical analysis. Where no stone is retrieved, its nature must be inferred from its radiological appearance (e.g. a completely radiolucent stone is likely to be composed of uric acid) or from more detailed metabolic evaluation.
In most patients, multiple factors are involved in the genesis of kidney stones and as a general guide, the following evaluation is appropriate in most patients.
Risk factors for stone disease
Diet: enquire about volume of fluid intake, meat consumption (causes hypercalciuria, high uric acid levels, low urine pH, low urinary citrate), multivitamins (vitamin D increases intestinal calcium absorption, although in healthy post-menopausal women with no history of stone formation vitamin D supplementation does not increase urinary calcium excretion), high doses of vitamin C (ascorbic acid causes hyperoxaluria).
Drugs: corticosteroids (increase enteric absorption of calcium, leading to hypercalciuria), chemotherapeutic agents (breakdown products of malignant cells leads to hyperuricaemia).
UTI: urease-producing bacteria (Proteus, Klebsiella, Serratia, Enterobacter) predispose to struvite stones.
Mobility: low activity levels predispose to bone demineralization and hypercalciuria.
Systemic disease: gout, primary hyperparathyroidism, sarcoidosis.
Family history: cystinuria, RTA.
Renal anatomy: PUJO, horseshoe kidney, MSK (up to 2% of patients with calcium-containing stones have MSK).
Previous bowel resection or inflammatory bowel disease: causes intestinal hyperoxaluria.
Metabolic evaluation of the stone former
Patients can be categorized as low risk and high risk for subsequent stone formation. High risk: previous history of a stone (i.e. multiple stone formers), bilateral stones, family history of stones, GI disease, uric acid stones or gout, chronic UTI, nephrocalcinosis, patients with solitary kidneys, staghorn calculi, children and young adults.
Low-risk patient evaluation
U & E, FBC (to detect undiagnosed haematological malignancy), serum calcium (corrected for serum albumin) and uric acid, urine culture, urine dipstick for pH.
Table 9.2 Characteristics of stone types | |||||||||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| |||||||||||||||||||||
High-risk patient evaluation
As for low-risk patients plus 24h urine for calcium, oxalate, uric acid, cystine; evaluation for RTA.
Urine pH
Urine pH in normal individuals shows variation from pH 5-7. After a meal, pH is initially acid because of acid production from metabolism of purines (nucleic acids in, for example, meat). This is followed by an ‘alkaline tide’, pH rising to >6.5. Urine pH can help establish what type of stone the patient may have (if a stone is not available for analysis) and can help the urologist and patient in determining whether preventative measures are likely to be effective or not.
pH <6 in a patient with radiolucent stones suggests the presence of uric acid stones.
pH consistently >5.5 suggests type 1 (distal) RTA (˜70% of such patients will form calcium phosphate stones).
Evaluation for RTA
Evaluate for RTA if: calcium phosphate stones, bilateral stones, nephro-calcinosis, MSK, hypocitraturia.
If fasting morning urine pH (i.e. first urine of the day) is >5.5, the patient has complete distal RTA.
First and second morning urine pH are a useful screening test for thedetection of incomplete distal RTA, >90% of cases of RTA having a pH >6 on both specimens. The ammonium chloride loading test involves an oral dose of ammonium chloride (0.1g per kg; an acid load). If serum pH falls <7.3 or serum bicarbonate falls <16mmol/L, but urine pH remains >5.5, the patient has incomplete distal RTA.
Diagnostic tests for suspected cystinuria
Cyanide-nitroprusside colorimetric test (‘cystine spot test’): if positive, a24h urine collection is done. A 24h cystine >250mg is diagnostic of cystinuria.1
1 Millman S, Strauss AL, Parks JH, Coe FL (1982) Pathogenesis and clinical course of mixed calcium oxalate and uric acid nephrolithiasis. Kidney Int 22:366-70.
Kidney stones: presentation and diagnosis
Kidney stones may present with symptoms or be found incidentally during investigation of other problems. Presenting symptoms include pain or haematuria (microscopic or occasionally macroscopic). Struvite staghorn calculi classically present with recurrent UTIs. Malaise, weakness, and loss of appetite can also occur. Less commonly, struvite stones present with infective complications (pyonephrosis, perinephric abscess, septicaemia, xanthogranulomatous pyelonephritis).
Diagnostic tests
Plain abdominal radiography: calculi that contain calcium are radiodense. Sulphur-containing stones (cystine) are relatively radiolucent on plain radiography.
Radiodensity of stones in decreasing order: calcium phosphate ” class=LK href=”javascript:void(0)” target=right xpath=”/CT{06b9ee1beed594192fe83c602fef4af9a59e63f847d6df62927a64e26327cf0c0e58d45b6bfdac2767fce92dc3549f3a}/ID(AB2-M1)”>> calcium oxalate ” class=LK href=”javascript:void(0)” target=right xpath=”/CT{06b9ee1beed594192fe83c602fef4af9a59e63f847d6df62927a64e26327cf0c0e58d45b6bfdac2767fce92dc3549f3a}/ID(AB2-M1)”>> struvite (magnesium ammonium phosphate) ” class=LK href=”javascript:void(0)” target=right xpath=”/CT{06b9ee1beed594192fe83c602fef4af9a59e63f847d6df62927a64e26327cf0c0e58d45b6bfdac2767fce92dc3549f3a}/ID(AB2-M1)”>>> cystine.
Completely radiolucent stones (e.g. uric acid, triamterene, indinavir) are usually suspected on the basis of the patient’s history and/or urine pH (pH <6—gout; drug history—triamterene, indinavir) and the diagnosis may be confirmed by USS, CT-KUB, or MRU.
Renal USS: its sensitivity for detecting renal calculi is variable depending on the series. Some series suggest ˜95% sensitivity for detecting stones, others just 50%.1 A combination of plain abdominal radiography and renal ultrasonography is a useful screening test for renal calculi.
IVU: virtually a historical investigation now having, to all intents and purposes, been replaced by CT-KUB. Useful for the rare patient with suspected indinavir stones (which are not visible on CT).
CTU: a very accurate method of diagnosing renal and ureteric stones (except) indinavir stones. Allows accurate determination of stone size and location and good definition of pelvicalyceal anatomy.
MRU: cannot visualize stones, but is able to demonstrate the presence of hydronephrosis.
1 Haddad MC, Sharif HS, Abomelha ME, et al. (1992) Management of renal colic: redefining the role of the urogram. Radiology 184:35-6.
Kidney stone treatment options: watchful waiting and the natural history of stones
The traditional indications for intervention are pain, infection, and obstruction. Haematuria caused by a stone is only very rarely severe or frequent enough to be the only reason to warrant treatment.
Before embarking on treatment of a stone which you think is the cause of the patient’s pain or infections, warn them that though you may be able to remove the stone successfully, their pain or infections may persist (i.e. the stone may be coincidental to their pain or infections which may be due to something else). Remember, UTIs are common in women as are stones and it is not, therefore, surprising that the two may coexist in the same patient, but be otherwise unrelated.
Options for stone management are watchful waiting, ESWL, flexible ureteroscopy, PCNL, open surgery, and medical ‘dissolution’ therapy.
When to watch and wait—and when not to
It is not necessary to treat every kidney stone. As a rule of thumb, the younger the patient, the larger the stone and the more symptoms it is causing, the more inclined we are to recommend treatment. Thus, one would be inclined to do nothing about a 1cm symptomless stone in the kidney of a patient aged 95y. On the other hand, a 1cm stone in a symptomless patient aged 20y runs the risk over the remaining (many) years of the patient’s life of causing problems. It could drop into the ureter, causing ureteric colic or it could increase in size and affect kidney function or cause pain.
The results of observational studies are conflicting, some suggesting most renal stones progress—increase in size, cause symptoms, or require intervention while others suggest many do not. In a series of 80 calyceal stones followed over 7.5y (stone size not reported), 45% of the stones increased in size and the authors concluded that 80% would require intervention within 5y.1 Conversely, 68% of patients with small renal stones remained asymptomatic over 2.5y in Glowacki’s study2 and in Keeley’s RCT of ESWL vs watchful waiting for small calyceal stones, only 9% required surgery over an average follow-up of 2y.3
Burger’s paper4 is helpful because it relates the risk of intervention to stone size and location, allowing a more tailored approach to decision making. Asymptomatic stones followed over a 3y period were more likely to require intervention (surgery or ESWL) or to increase in size or cause pain if they were >4mm in diameter or if located in a middle or lower pole calyx.4 The approximate risks over 3y of follow-up of requiring intervention, developing pain, or of increase in stone size relative to stone size is shown in Table 9.3.
Another factor determining the need for treatment is the patient’s job. Airline pilots are not allowed to fly if they have kidney stones for fear that the stones could drop into the ureter at 30 000 ft with disastrous consequences! They will only be deemed fit to fly when they are radiologically
stone-free. It is sensible to warn any one whose job entrusts them with the safety of others (pilots, train drivers, drivers of buses and lorries) that they are not fit to carry out these occupations until stone-free or, at the very least, that they should contact the relevant regulatory authority to seek guidance (the Civil Aviation Authority (CAA) for pilots and the Drivers Vehicle Licensing Agency (DVLA) for drivers).5
stone-free. It is sensible to warn any one whose job entrusts them with the safety of others (pilots, train drivers, drivers of buses and lorries) that they are not fit to carry out these occupations until stone-free or, at the very least, that they should contact the relevant regulatory authority to seek guidance (the Civil Aviation Authority (CAA) for pilots and the Drivers Vehicle Licensing Agency (DVLA) for drivers).5
Some stones are definitely not suitable for watchful waiting. Untreated struvite (i.e. infection-related) staghorn calculi will eventually destroy the kidney if untreated and are a significant risk to the patient’s life. Watchful waiting is, therefore, NOT recommended for staghorn calculi unless patient comorbidity is such that surgery would be a higher risk than watchful waiting. Historical series suggest that somewhere between 9 and 30% of patients with staghorn calculi who did not undergo surgical removal (from choice or because of comorbidity) died of renal-related causes— renal failure, urosepsis (septicaemia, pyonephrosis, perinephric abscess).6, 7 and 8 A combination of a neurogenic bladder and staghorn calculus seems to be particularly associated with a poor outcome.9
1 Hubner WA, Porpaczy P (1990) Treatment of calyceal calculi. Br J Urol 66:9-11.
2 Glowacki LS, Beecroft ML, Cook RJ, Pahl D, Churchill DN (1992) The natural history of asymptomatic urolithiasis. J Urol 147:319-21.
3 Keeley FX, Tilling K, Elves A, et al. (2001) Preliminary results of a randomized controlled trial of prophylactic shock wave lithotripsy for small asymptomatic renal calyceal stones. BJU Int 87:1-8.
4 Burgher A, Beman M, Holtzman JL, Monga M (2004) Progression of nephrolithiasis: long-term outcomes with observation of asymptomatic calculi J Endourol 18:534-9.
5 Borley NC, Rainford D, Anson KM, Watkin N. (2007) What activities are safe with kidney stones? A review of occupational and travel advice in the UK. Br J Urol Int 99:494-6.
6 Blandy JP, Singh M (1976) The case for a more aggressive approach to staghorn stones. J Urol 115:505-6.
7 Rous SN, Turner WR (1977) Retrospective study of 95 patients with staghorn calculus disease. J Urol 118:902.
8 Vargas AD, Bragin SD, Mendez R (1982) Staghorn calculi: clinical presentation, complications and management J Urol 127:860-2.
9 Teichmann J (1995) Long-term renal fate and prognosis after staghorn calculus management. J Urol 153:1403-7.
Stone fragmentation techniques: extracorporeal lithotripsy (ESWL)
The technique of focusing externally generated shock waves at a target (the stone). First used in humans in 1980. The first commercial lithotriptor, the Dornier HM3, became available in 1983.1 ESWL revolutionized kidney and ureteric stone treatment.
Three methods of shock wave generation are commercially available— electrohydraulic, electromagnetic, and piezoelectric.
Electrohydraulic: application of a high voltage electrical current between two electrodes about 1mm apart under water causes discharge of a spark. Water around the tip of the electrode is vaporized by the high temperature, resulting in a rapidly expanding gas bubble. The rapid expansion and then the rapid collapse of this bubble generate a shock wave that is focused by a metal reflector shaped as a hemiellipsoid. Used in the original Dornier HM3 lithotriptor.
Electromagnetic: two electrically conducting cylindrical plates are separated by a thin membrane of insulating material. Passage of an electrical current through the plates generates a strong magnetic field between them, the subsequent movement of which generates a shock wave. An ‘acoustic’ lens is used to focus the shock wave.
Piezoelectric: a spherical dish is covered with about 3000 small ceramic elements, each of which expands rapidly when a high voltage is applied across them. This rapid expansion generates a shock wave. X-ray, USS, or a combination of both are used to locate the stone on which the shock waves are focused. Older machines required general or regional anaesthesia because the shock waves were powerful and caused severe pain. Newer lithotriptors generate less powerful shock waves, allowing ESWL with oral or parenteral analgesia in many cases, but they are less efficient at stone fragmentation.
Efficacy of ESWL
The likelihood of fragmentation with ESWL depends on the stone size and location, anatomy of renal collecting system, degree of obesity, and stone composition. Most effective for stones <1cm in diameter and in favourable anatomical locations. Less effective for stones >1cm diameter, in lower pole stones in a calyceal diverticulum (poor drainage), and those composed of cystine or calcium oxalate monohydrate (very hard).
Randomized studies show that a lower shock wave rate (60 vs 120 per min) achieves better stone fragmentation and clearance. Animal studies also demonstrate less renal injury and a smaller decrease in renal blood flow from lower shock wave rates.2
There have been no randomized studies comparing stone-free rates between different lithotriptors. In non-randomized studies, rather surprisingly, when it comes to the efficacy of stone fragmentation, older (the original Dornier HM3 machine) is better (but with a higher requirement for analgesia and sedation or general anaesthesia). Less powerful (modern) lithotriptors have lower stone-free rates and higher retreatment rates.
Side effects of ESWL (see Fig. 9.3)
ESWL causes a certain amount of structural and functional renal damage (found more frequently the harder you look). Haematuria (microscopic, macroscopic—due to the rupture of intraparencyhmal vessels) and oedema are common, perirenal haematomas less so (0.5% detected on USS with modern machines, although reported in as many as 30% with the Dornier HM3). Effective renal plasma flow (measured by renography) has been reported to fall in ˜30% of treated kidneys.
Renal injury during ESWL is significantly reduced by slowing the rate of shock wave delivery from 120 to 30 shock waves per min.3
There are data suggesting that ESWL may increase the likelihood of development of hypertension. Acute renal injury may be more likely to occur in patients with pre-existing hypertension, prolonged coagulation time, coexisting coronary heart disease, diabetes, and in those withsolitary kidneys. A retrospective case control study with 19y follow-up has raised the possibility that ESWL may cause pancreatic damage, leading to a higher risk of diabetes—diabetes developed in 16.8% of patients undergoing ESWL vs 6.6% of controls.4
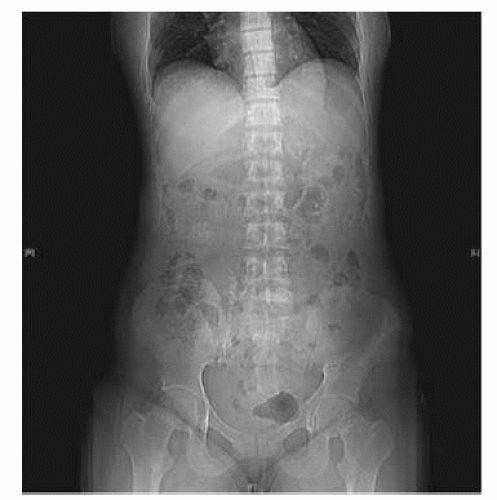 Fig. 9.3 Side effects of ESWL: steinstrasse (= Stone Street) or ‘log-jam’. |
Should a stent be inserted prior to ESWL to renal (or ureteric) calculi?
Is ESWL more effective in the absence of pre-ESWL stenting? Probably yes.5 Does pre-ESWL stenting reduce the risk of ESWL complications? Probably not. When ESWL was first introduced, stones of all sizes were treated. It soon became apparent that multiple fragments from large stones could obstruct the ureter, causing a so-called steinstrasse (incidence of steinstrasse 2-3% for stones 1.5-2cm diameter; 56% for stones 3-3.5cm).
Whether stenting prior to ESWL can reduce the risk of steinstrasse remains controversial. Pre-ESWL stenting does not reduce the chances of spontaneous resolution of the steinstrasse (spontaneous passage of the stones). We nowadays see steinstrasse only rarely because ESWL tends to be reserved for smaller stones (<2cm) and PCNL for larger stones. Steinstrasse is managed expectantly (since 50% will resolve spontaneously), with ESWL of the so-called ‘lead’ fragment or ureteroscopy being required where the stones fail to pass.
The overall consensus is that pre-ESWL stenting is probably not necessary in most cases. For patients with solitary kidneys undergoing ESWL, prestenting is an option to reduce the risk of renal obstruction. The alternative is closer monitoring in the days and weeks after ESWL and emergency ureteroscopy where anuria develops.
Contraindications to ESWL
Absolute contraindications: pregnancy, uncorrected blood clotting disorders (including anticoagulation); known renal artery.
BAUS procedure-specific consent form: potential complications after ESWL
Common
Bleeding on passing urine for short period after procedure.
Pain in the kidney as small fragments of stone pass after fragmentation. UTI from bacteria released from the stone, needing antibiotic treatment.
Occasional
Stone will not break as too hard, requiring an alternative treatment.
Repeated ESWL treatments may be required.
Recurrence of stones.
Rare
Kidney damage (bruising) or infection, needing further treatment.
Stone fragments occasionally get stuck in the tube between the kidney and the bladder, requiring hospital attendance and sometimes surgery to remove the stone fragment.
Severe infection requiring IV antibiotics and sometimes drainage of the kidney by a small drain placed through the back into the kidney.
Alternative therapy
Telescopic surgery, open surgery, or observation to allow spontaneous passage.
What is the fate of the ‘clinically insignificant fragment’ after ESWL?
Clinically insignificant residual fragments (CIRFs) are residual stone fragments 4mm in size or less after ESWL. ‘Clinically insignificant’ is something of a misnomer for 12-46% of such fragments will increase in size over a period of 2-3y.6, 7, 8, 9 and 10 Given that there is a significant risk of increase in stone size and given our knowledge that stones that grow are likely to continue to do so and, therefore, require intervention or to become symptomatic and so require intervention, radiological follow-up of such patients seems to be sensible. How (plain X-ray if the stones are visible, USS or CT), how often and by whom (in primary care or by urologists) are contentious issues?
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree