Fig. 18.1
This figure shows the major vessels of the colon that must be identified during open left colectomy. The marginal artery of Drummond is the collateral vessel between the superior and inferior mesenteric arteries
The venous drainage mirrors the arterial supply. The small and intermediate veins eventually join to become the inferior mesenteric vein. The inferior mesenteric vein courses within the mesentery just lateral to the duodenum and eventually drains into the splenic vein. The splenic and superior mesenteric veins then merge to create the portal vein.
Lymphatic drainage follows the vascular supply. Colonic resection is often determined by the margins of devascularized colon following an adequate lymphadenectomy. As the lymphatics are thought to be an early site of tumor metastasis, it is imperative to have an appropriate sampling of paracolic and intermediate lymph nodes to be considered an adequate oncologic resection. A minimum retrieval of 12 lymph nodes has been adopted as a quality measure by many groups. However, node count is influenced not only by surgical technique, but also by adequacy of pathologic assessment, patient-related factors (e.g., age) and tumor-related factors (e.g., tumor location, T stage, or microsatellite status).
There is debate as to the extent of lymphadenectomy required for optimal oncologic clearance. Several authors have advocated the widespread adoption of “complete mesocolic excision” (CME) with anatomic dissection of the mesocolon along its embryological fascial planes and high ligation of the vascular pedicle (e.g., for left colon cancer, the origin of the inferior mesenteric artery and vein). While excellent results have been reported by experienced CME surgeons, randomized trials comparing CME to conventional resection have not been performed.
Preoperative Management
A thorough preoperative workup is necessary to afford patients the greatest chance for a positive outcome following surgery. All patients should undergo a complete history and physical exam. All medical comorbidities should be optimized prior to surgery and any further cardiovascular or pulmonary workup should be performed when deemed appropriate.
If a complete colonoscopic evaluation was not previously performed, it should be done to rule out synchronous tumors and polyps. The tumor should be tattooed in at least 3 and preferably 4 quadrants to aid in intraoperative identification of the area in question. Tattooing becomes especially important when operating for smaller lesions or endoscopically unresectable/high-risk polyps. Basic lab work including hemoglobin, platelet count, comprehensive metabolic panel to check for renal and hepatic function, and carcinoembryonic antigen (CEA) should be performed. Not all colon malignancies will secrete CEA, but for those that do it is helpful in the surveillance of patients postoperatively as it is usually one of the first signs of recurrence.
A complete metastatic workup should also be performed consisting of a computed tomographic (CT) scan of the chest, abdomen, and pelvis with oral and intravenous (IV) contrast. If the tumor is found to be locally invasive, i.e., involving any surrounding organs or structures, preoperative consultation with surgical specialists would be beneficial to ensure that an en bloc, curative resection could be performed at the time of surgery. If there is any question to the resectability of a locally invasive lesion or if there are indeterminate hepatic lesions, a magnetic resonance imaging (MRI) scan can be helpful in aiding preoperative decision making.
If distant disease is identified and the patient is otherwise asymptomatic from the primary lesion, consideration should be given to systemic therapy with chemotherapy prior to surgery. In the situation of distant disease, overall survival will be tied to the effectiveness of systemic treatment and not to the resection of the primary tumor. After treatment with chemotherapy, restaging should be performed. For patients with resectable metastases, options include resection of the metastases first, resection of the primary first, or in patients with hepatic metastases, minimal medical comorbidities, and good performance status, a synchronous procedure to remove both the primary and metastatic lesions. Resection of the primary tumor in the face of unresectable metastases is a controversial issue, but in general, resection should be avoided unless the patient is symptomatic from the primary lesion or if there is clear evidence of impending obstruction.
The day prior to surgery the patient should be maintained on a clear liquid diet and consideration of a mechanical bowel preparation. There have been numerous studies to demonstrate the safety and potential benefits of performing elective colon resections without prior mechanical bowel preparation. However, in cases involving small tumors or malignant polyps, consideration should be given to mechanical bowel preparation to allow the possibility of performing intraoperative colonoscopy for possible localization of the lesion.
Perioperative Preparation
Prior to the patient being transferred into the operating room, a prophylactic dose of antibiotic as well as 5,000 units of subcutaneous heparin should be administered within 1 h of incision. Various antibiotic regimens are acceptable, but our preference is to use 1 g of IV ertapenem (Merck, Whitehouse Station, NJ) as it is a single dose that will last for 24 h. In addition, patients should be maintained with an active warming device in the preoperative area to achieve normothermia (>36 °C).
After the induction of general anesthesia, the patient is placed into a modified low lithotomy position. The arms are abducted in such a position to allow for future placement of a self-retaining retractor. Care must be taken to ensure that both shoulders, elbows, and calves are appropriately positioned/padded to avoid positional neuropathies. A sterile Foley catheter and an orogastric tube are placed. The abdomen is then prepped with a chlorhexidine solution and towels are used to square off the operative field. A plastic adhesive is then placed over the abdomen to secure the towels in place. A “time out” is performed to confirm the patient’s identity and the planned operation.
Incision
A midline laparotomy incision is made (Fig. 18.2). The extent of the incision will vary depending on the portion of the left colon being removed. For distal lesions, a lower midline incision down to the pubic bone may be sufficient. For proximal lesions near the splenic flexure, extension of the incision to the xiphoid process may be required. Once an adequate incision has been made, a plastic wound protector is placed into the wound to not only aid in prevention of contamination of the wound itself, but also to aid in maximizing the exposure for any given incision.
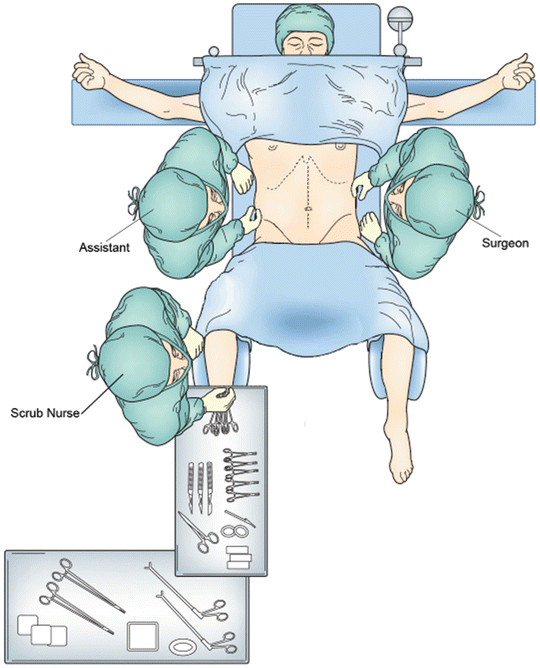

Fig. 18.2
The figure shows patient positioning for open left colectomy. The arms are abducted and the legs are placed in lithotomy position
Examination of the Peritoneal Cavity
A complete abdominal exploration should then be undertaken to rule out the presence of metastatic disease as well as to confirm the location of the lesion in question. Both lobes of the liver should be palpated and the peritoneal surfaces visually inspected. Both ovaries should be inspected for possible metastatic disease. Unexpected masses/nodules should be biopsied and sent for frozen section. If carcinomatosis is encountered, closure of the abdomen and referral for either systemic therapy or heated intraperitoneal chemotherapy and tumor debulking may be warranted.
Once distant disease has been ruled out, a self-retaining retractor should be placed to maintain exposure. For distal lesions it is advantageous to keep the ring of the retractor close to the patient’s skin and center the ring at the lower portion of the incision. For proximal lesions and splenic flexure mobilization it is helpful to position the ring more cephalad and to the left. It is often helpful during splenic flexure mobilization to place the ring at an angle, with the left/superior aspect of the ring elevated several inches off the abdominal wall to provide anterior retraction and improve visualization of the flexure. The surgeon should not hesitate to move the ring and reset the retractors to optimize exposure during various phases of the case. The small bowel is then packed into the right upper quadrant with moist laparotomy pads.
Extent of Resection
Once proper exposure has been established, it is necessary to determine the extent of resection that will be required. The lymphadenectomy will often times dictate the margins of resection. For splenic flexure lesions, proper lymphadenectomy will require ligation of the left branch of the middle colic artery at its base as well as ligation of the left colic artery as it takes off from the inferior mesenteric artery. For left colon cancers the left branch of the middle colic, left colic, and possibly the first sigmoidal branch need to be ligated depending on the location of the tumor. For sigmoid lesions the superior hemorrhoidal artery is ligated distal to the takeoff of the left colic artery and the distal extent will be within the proximal rectal mesentery (Fig. 18.3). We do not advocate routine ligation of the inferior mesenteric artery itself, as there have been no studies to prove an oncologic benefit to a high ligation. Occasionally this may be necessary if a concerning lymph node is identified or to obtain adequate length for a tension-free anastomosis. High ligation is also easier when the entire left side of the colon (including sigmoid) is being removed, such as in the case of synchronous lesions, uncertain location of a previously resected malignant polyp, or the presence of significant diverticular disease when operating for descending colon cancer.
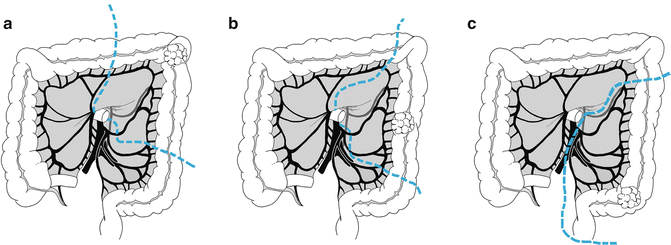





Fig. 18.3
The figure illustrates the extent of resection for (a) splenic flexure lesion, (b) descending colon lesion, and (c) sigmoid colon lesion
< div class='tao-gold-member'>
Only gold members can continue reading. Log In or Register to continue
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree








