and Andrea Bischoff1
(1)
Pediatric Surgery, Colorectal Center for Children Cincinnati Children’s Hospital, Cincinnati, OH, USA
5.1 Introduction
5.2 Stoma Locations
5.3 Ileostomies
5.7 Cecostomies
5.11 Colostomy Care
5.12 Colostomy Closure
5.13 Surgical Technique
5.16 Prolapse
5.1 Introduction
Colostomy is a procedure designed to divert the fecal stream from the normal passage to the rectum, creating an opening between the colon and the abdominal wall. This procedure was created to relieve the obstruction of the colon produced by acquired or congenital conditions. Another indication is to avoid the passing of stool through an operated area, trying to prevent complications, such as infection and/or dehiscence [1–6].
Historically, it is considered that the first colostomy in pediatrics was performed in 1783 by Antoine Dubois in a 3-day-old infant with an imperforate anus [7].
A colostomy can be permanent, when it is considered that there is no way to reconstruct the colon distal to the stoma or there is no way to establish bowel control, and it is considered that the quality of life is better with a stoma as compared without stoma.
Temporary colostomies are those created for a period of time until the anatomic or functional circumstances of the patients allow the reestablishment of the colonic transit. Colostomies can be divided into two groups: totally diverting and partially diverting.
Totally diverting colostomies are those that divert the entire fecal stream and do not allow the spillage or passing of stool into the bowel distal to the stoma. In order to achieve total diversion of the stool, it is necessary to separate the proximal and distal bowel after the colon is divided and to separate both stomas enough, as to allow the proximal (functional) stoma to be covered by a stoma bag without including the distal stoma (Fig. 5.1). Another way to achieve a totally diverting procedure is by closing the distal end, a maneuver that is known as a “Hartmann pouch.” The closure of the distal stoma leaves the patients with a completely closed blind loop distal bowel; this, in the absence of a fistula, creates a mucocele (accumulation of mucus) which will represent a serious problem for the patient, as most mucoceles eventually become infected. Mucoceles may also occur in cases in which the fistula that connects the colon with the urogenital tract is very narrow and does not allow the passing of mucus. In addition, patients with a Hartmann pouch cannot have contrast studies done through the distal stoma to evaluate their anatomy prior to reconstruction because there is no access to it. This is a serious deficiency, because we firmly believe the most valuable diagnostic test in patients with anorectal malformation consists in the injection of contrast material through the distal stoma (high-pressure distal colostogram) (see Chap. 6).
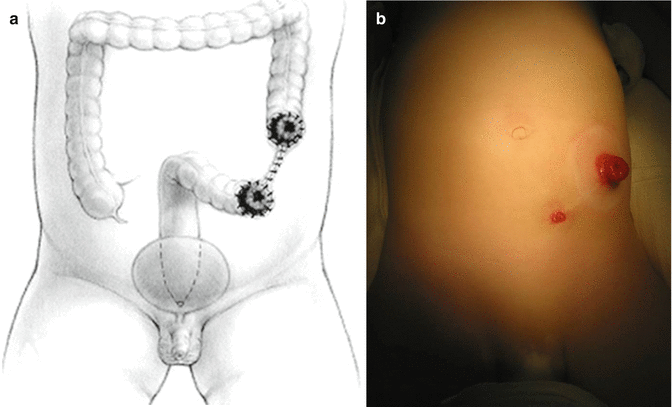

Fig. 5.1
Both stomas separated enough to cover only the proximal one with the stoma bag. (a) Diagram. (b) Picture
A partially diverting stoma, by definition, allows most of the stool to come out of the body, but some of the stool still may go into the distal colon. This happens when both stomas are together and covered by a single stoma bag, and the surgeons open a colostomy known as “loop colostomy” (Fig. 5.2).
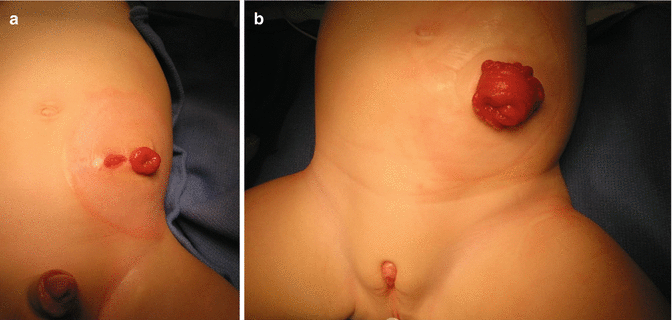

Fig. 5.2
Inadequate colostomy. (a) Both stomas located too close. (b) Loop colostomy
The indication to divert the fecal stream totally or partially depends on the specific problem of the patient. In cases of anorectal malformations, the surgeon should keep in mind that over 85 % of all the patients have a connection between the distal colon and the urogenital tract. In addition, 5 % of the total group of anorectal malformations has a completely blind distal bowel. This is very important to remember, because a partially diverting colostomy (loop or both stomas located too close one to the other) exposes the patient to the passing of stool into the urinary tract and/or to a distal impaction of stool that cannot pass through a narrow fistula. Loop colostomies are very appealing for most surgeons. We think the reason for this is that it is an easy operation that can be done fast and also can be closed in a fast and easy way. However, we consider that loop colostomies are formally contraindicated in patients with anorectal malformations due to the following reasons:
High chances of producing direct fecal contamination of the urinary tract
High chances of producing distal fecal impaction, megarectum, and consecutive severe constipation after colostomy is closed (Fig. 5.3)
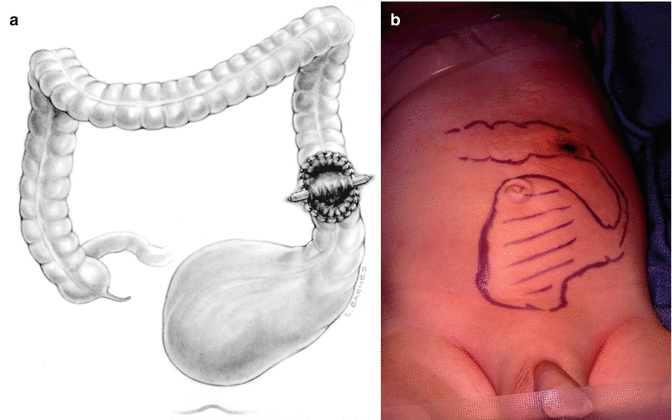
Fig. 5.3
Loop colostomy with distal fecal impaction. (a) Diagram. (b) Picture
Higher incidence of prolapse
5.2 Stoma Locations
The stoma can be opened in the abdomen in different locations. The most common locations are:
Right transverse colostomy (right upper quadrant): Some surgeons prefer this type of stoma consisting in dividing the right portion of the transverse colon and diverting it through the right upper quadrant of the abdomen (Fig. 5.4).
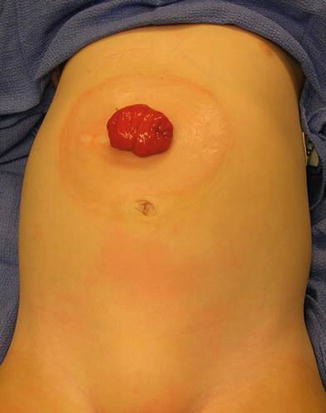
Fig. 5.4
Photograph of a right transverse colostomy
Left transverse colostomy: The left portion of the transverse colon is divided, and the stoma(s) is opened in the left upper quadrant of the abdomen (Fig. 5.5).
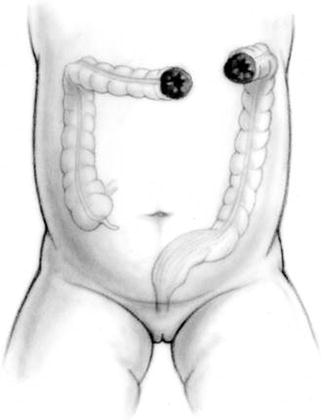
Fig. 5.5
Diagram of a left transverse colostomy
Descending colostomy: The bowel is divided immediately distal to the descending colon, in the first mobile portion of the sigmoid, and the stoma is usually opened in the left lower quadrant of the abdomen (Fig. 5.6). This is the type of colostomy that we recommend.
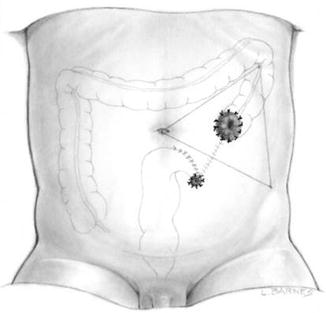
Fig. 5.6
Diagram showing a descending colostomy with separated stoma (preferred by the authors)
Sigmoid colostomy: The sigmoid colon is divided, and the stomas are usually opened somewhere in the lower abdomen. The problem with this kind of colostomy is that there is a possibility of creating the stoma too distal in the colon, leaving a very short piece of bowel available for the pull-through (Fig. 5.7).
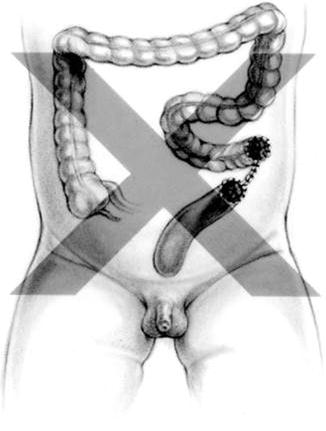
Fig. 5.7
Sigmoid colostomy, leaving a too short distal bowel that interferes with the pull-through
5.3 Ileostomies
Ileostomies are frequently performed in patients with colorectal problems. These are indicated when, for some specific reason, we cannot use the colon to perform the diversion. In other words, the entire colon does not function, such as in cases of total colonic aganglionosis or when the patient was born with no colon or has lost the entire colon. An ileostomy is sometimes used when a patient had a pull-through of the ascending colon, and therefore the patient needs a diversion proximal to this.
5.4 To Divert or Not to Divert, That Is the Question
In general, pediatric surgeons and general surgeons are looking for safe ways to perform colorectal procedures without a protective colostomy. By doing this, the patients are prevented from having two extra serious operations with significant morbidity (colostomy opening and colostomy closure). That is the reason why to perform colorectal surgery without a colostomy is always an attractive idea (see Chap. 4). Taking advantage of modern surgical technology, efficient methods to clean the colon, the possibility of keeping the patient with nothing by mouth for a period of time receiving parenteral nutrition, the use of sophisticated surgical techniques, and the availability of powerful antibiotics, allow, nowadays, to perform successful operations on the colorectal tract without a protective colostomy. Yet, catastrophic complications still happen [8]. It is true, the incidence of these complications is much less than in the past, but unfortunately they still occur. That is why the question whether “to divert or not to divert” is still unanswered and remains a matter of controversy.
In general, pediatric surgeons keep moving in the direction of doing more and more primary procedures without a protective colostomy. We believe that it is good to move in that direction, to save our patients from the potential morbidity associated with stomas that are still high [3, 9–30].
It is also very important to remember that in dealing with the treatment of anorectal malformations, a postoperative wound infection has consequences much more serious than in cases of other surgical conditions. A wound infection due to the repair of an anorectal malformation means not only that the patient will suffer the inconveniences and risks related with the infection itself, but, in addition, the final functional prognosis (bowel and urinary control) may be jeopardized.
We are against universal indications for a procedure. In other words, we believe that a colostomy is indicated under certain specific circumstances; a patient with a specific malformation may need a colostomy, and yet another patient with exactly the same type of defect, but under different surrounding circumstances, may not require a colostomy. This includes how sick the patient is, how severe are their associated defects, how advanced is the technology available for the patient, how much experience the surgeons have in the performance of primary procedures done without a colostomy, and how sophisticated is the infrastructure that surrounds the patient, including laboratory, intensive care, surgical technology, availability of central venous access, hyperalimentation, and a clean environment.
A colostomy definitely still has a recognized protective value in the postoperative course of most colorectal and anorectal operations. In other words, not opening a protective colostomy has a definite increased risk for the patient. Admittedly, many colorectal procedures can be done successfully without a protective colostomy, but cannot be done without the acceptance of a certain degree of risk.
Finally, we believe that when a surgeon is confronted with the difficult decision of whether to open or not to open a colostomy in a specific patient, he or she should always try to imagine what he would do if he was dealing with his own son or daughter.
Most of the patients, who come to us after the neonatal period, already have a colostomy, and therefore we do not have to deal with this dilemma.
In a full-term, newborn baby without severe associated defects, we do not open a colostomy if the baby has one of the following malformations: perineal fistula, vestibular fistula, imperforate anus with no fistula, and rectourethral bulbar fistula. In the case of the last two malformations (imperforate anus without fistula and rectourethral bulbar fistula), we expect to see the distal end of the rectum full of gas, located below the coccyx in a cross-table lateral film. Based on our experience, we can confidently operate primarily on these types of cases without a colostomy with good results. All other patients with anorectal malformations, at our institution, receive a colostomy, not only to protect the patient from the operation to repair the malformation, but also for other reasons, including the fact that we need a stoma in order to do a high-pressure distal colostogram which we consider the most valuable diagnostic test in patients with anorectal malformations. Other sophisticated, state-of-the-art imaging modalities still cannot compete with the accuracy of the anatomic information that we obtain with a high-pressure distal colostogram. Most of the serious catastrophes we have seen occurred in cases that were surgically explored at other institutions without a high-pressure distal colostogram [8]. In addition, higher anorectal malformations have a higher incidence of serious associated defects, mainly urologic, cardiac, and gastrointestinal, which means higher-risk patients.
5.5 Recommended Types of Colostomies
5.5.1 Newborn Babies with Anorectal Malformations
In newborn babies with anorectal malformations, in whom we consider that a colostomy is indicated, we prefer to open a descending colostomy, with widely separated stomas, located in the left lower quadrant of the abdomen (Fig. 5.6) [1, 30].
In our series of 2,032 patients, only 75 of them had a colostomy done at our institution. Over 200 cases underwent a primary repair without a colostomy; most of those suffered from perineal or vestibular fistula. All of the others came to our institution with a colostomy already open. As the reader can imagine, that means that we have seen almost all kinds of colostomies and have learned the advantages and disadvantages of each type. That gave us an illuminating experience related to colostomies [30]. Based on that experience, we concluded that a descending colostomy with separated stomas is the best one, for the following reasons:
(a)
It effectively diverts the entire fecal stream.
(b)
It significantly decreases the chances of urinary tract infection.
(c)
It avoids the formation of megarectosigmoid because it allows the irrigation and cleaning of the distal bowel and avoids distal fecal spillage.
(d)
(e)
It does not interfere with the pull-through.
(f)
It will not prolapse when done properly.
Transverse colostomies are not recommended in anorectal malformations for several reasons:
(a)
It is impossible to irrigate the distal colon that remains full of meconium for the weeks or months after the colostomy is created.
(b)
It has a tendency to provoke a severe megarectosigmoid, as a consequence of the presence of meconium that was never removed, plus the accumulation of mucus produced by the entire defunctionalized colon and desquamation of mucosa cells.
In fact, the longer the period of time between the colostomy opening and the final repair, the greater the megarectosigmoid (Fig. 5.8). This will translate eventually into severe constipation, difficult to manage, after the repair of the malformation.
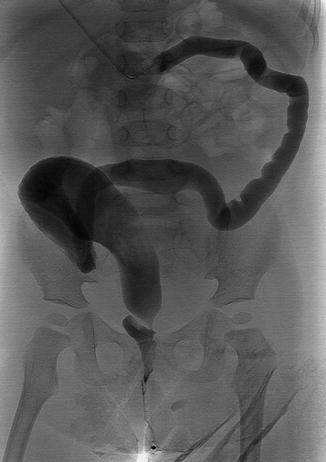

Fig. 5.8
Colostogram in a patient with transverse colostomy, showing the characteristic narrow (non-used) distal colon, with a megarectosigmoid
(c)
(d)
The incidence of urinary tract infection is higher than in cases with descending colostomies.
(e)
The high-pressure distal colostogram (the most valuable diagnostic study in anorectal malformations) is difficult to do, may not be accurate, and is risky. It is not accurate, because it is very difficult to exert enough hydrostatic pressure, when the injection of contrast material is done from the transverse colon to fill up and to demonstrate the fistula site, located all the way down to the rectum. In an attempt to demonstrate the location of the fistula, the colon may perforate. We have had two cases with such a complication. This incident has never happened in patients with descending colostomies.
The opening of a loop colostomy in the transverse colon is perhaps the worst type of colostomy that we have seen, because in addition to all of the problems that we have seen with transverse colostomies, the patients pass stool into the distal bowel which increases the chance of urinary tract infection and frequently produces fecal impaction in the distal stoma. Figure 5.8 shows the characteristic situation of a patient that had a bad loop transverse colostomy with fecal impaction in the distal bowel. Those fecal impactions cannot be relieved by washing the colon. It is sometimes necessary to perform a laparotomy to remove the hard stool from the distal bowel prior to the main repair. Loop colostomies, in general, also have a greater tendency to prolapse (Fig. 5.9).
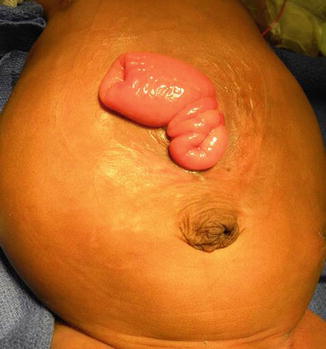

Fig. 5.9
Prolapsed transverse colostomy
5.6 Left Transverse Colostomy
The complications that we mentioned about right transverse colostomies are similar in a left transverse colostomy.
5.7 Cecostomies
Opening of colostomies in the cecum, in general, has no indication in anorectal malformations. All of the problems mentioned when discussing right transverse colostomies are more serious in cases of cecostomies.
In the type of descending colostomy that we recommend, the proximal stoma will not prolapse due to the fact that it belongs to the fixed portion of the descending colon. On the other hand, the distal stoma belongs to the mobile portion of the sigmoid, and therefore it has a higher risk of prolapse. To avoid that, we specifically recommend creating a very small (about 3 mm diameter) distal stoma (mucous fistula) (Fig. 5.6).
5.8 Creation of a Colostomy
5.8.1 Surgical Technique
In a newborn baby with anorectal malformation, we try to perform a colostomy not before 24 h after the baby is born. In the chapter dedicated to the management of a newborn with an anorectal malformation, we explain in detail the reasons why we want to wait 24 h. However, we do not want to wait much more than that time, because perforations of the bowel have been reported to occur in patients after 24 h of life. It is true that occasionally, patients can live many days passing meconium through the recto-urinary fistula without perforation, but that is an exception. There are reports of catastrophes that occurred in patients who suffered colon perforation and died because a colostomy was not done on time (see Chap. 4). The patient is taken to the operating room, and under general anesthesia, the abdominal wall is washed, prepped, and draped in the usual manner. The incision that we recommend is an oblique one, running from the left flank down to the left lower quadrant of the abdomen (Fig. 5.10). The upper part of the incision is located at the same site where we expect to create the proximal stoma. This point is located at equal distance between the umbilicus, the ribs, and the anterior superior iliac crest. We intentionally want the proximal, functional stoma to be surrounded by normal skin and to be located as far away as possible from a prominence, irregularity, or structure that may interfere with the placement of a stoma bag. These structures are the umbilicus, the rib cage, and the iliac bone. When the stomas are open too close to one of these structures, the stoma therapist, the nurses, and the mothers struggle trying to place a stoma bag that lays flat, avoiding leakage of stool and resultant skin irritation.
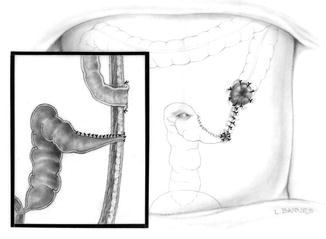

Fig. 5.10
Diagram showing an oblique preferred incision for a neonatal colostomy
The lower and medial end of the incision represents the location of the mucous fistula site, which we create intentionally very small (Fig. 5.10) to avoid prolapse. Both stomas must be separated enough so as to be able to use a stoma bag only on the proximal stoma, away from the mucous fistula.
The abdomen is opened, and it becomes very obvious that there is a big, dark loop of bowel (Fig. 5.11) that represents a very dilated sigmoid full of meconium. One should not try to manipulate this very tense, dilated sigmoid loop of bowel, because this may result in injuries to the seromuscular layer. Also, one should not try to create the stoma in the most dilated part of this colon, because that would make a huge stoma difficult to manage and more prone to suffer prolapse. We rather should look for the less-dilated descending colon, normally fixed to the left retroperitoneum. The descending colon detaches from the left parieto-colic space and becomes mobile (Fig. 5.12). At that particular point, we select a portion of the bowel, long and mobile enough, to comfortably reach the anterior abdominal wall. Before we divide the bowel at the selected location, we specifically suggest putting a purse-string suture with a 5-0 suture. In the center of the purse-string suture, we make an opening in the bowel wall and introduce a 12 Foley catheter into the lumen of the very dilated colon with meconium. The purse-string suture is tied to avoid leakage of meconium in the operative field (Fig. 5.13). The dilated colon is then irrigated with warm saline solution for a period of about 10–15 min until the entire sigmoid is completely decompressed and free of meconium. This maneuver is extremely valuable for several reasons. First, because it will allow the surgeon to manipulate a collapsed, well-perfused bowel (Fig. 5.14) and to perform a neat operation preserving the bowel integrity. In addition, the patient will have a clean, collapsed colon for the rest of the weeks or months before the pull-through or main repair is done. We have evidence to believe that this helps to avoid the formation of a megarectosigmoid and therefore decreases the incidence of severe constipation in these patients. In the same place where the purse-string suture was placed, we apply two Baby Allen clamps to divide the bowel (Fig. 5.15). Special care and attention must be given to the preservation of the colonic vascular arcade during the division of the bowel. The preservation of the arcade allows manipulating and mobilizing the distal bowel, at the time of the main repair, preserving a good blood supply. The proximal bowel will be exteriorized as a functional stoma at the left upper corner of our incision and the mucous fistula in the lower and medial end of the incision. The last 2 or 3 cm of the distal bowel is tapered, creating a little stoma (mucous fistula) of approximately 3–4 mm diameter (Fig. 5.15). The mucous fistula is necessary to do irrigations of the distal bowel if indicated and also to allow access to the distal stoma to perform a high-pressure distal colostogram. For this, we do not need a large stoma that may bleed and interfere with the quality of life of the patient. The tiny lumen also helps to avoid prolapse.
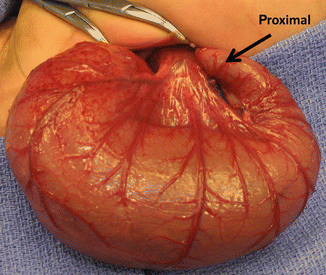
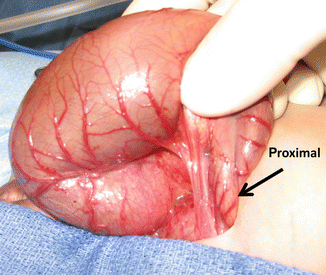
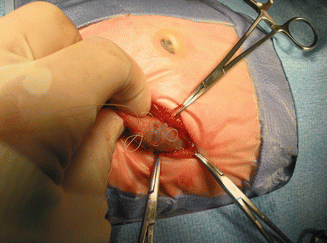
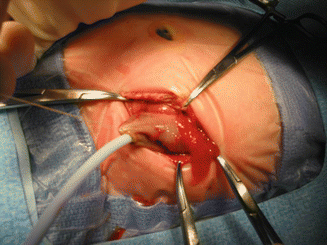
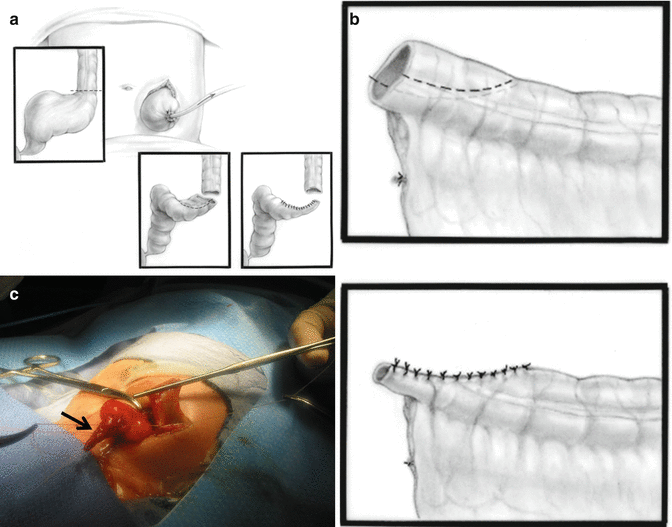

Fig. 5.11
Trans-operatory picture, a dilated sigmoid colon, full of meconium, is seen

Fig. 5.12
The proximal stoma must be created using the first mobile portion of the descending colon

Fig. 5.13
A purse-string suture is placed on the anterior wall of the selected loop of the colon, where the stoma will be located

Fig. 5.14
A catheter is introduced through the center of the purse string to irrigate and remove all the meconium. The bowel collapses and is well perfused

Fig. 5.15
The colon is divided at the same location of the purse-string suture, and the distal bowel is tapered. (a) Diagram showing the division of the colon. (b) Diagram showing the tapering of the distal bowel. (c) Intraoperative view. Arrow showing tapered distal bowel
The proximal stoma must be meticulously constructed. The bowel is sutured to the fascia and peritoneum, being sure not to produce a stricture and/or ischemia and being sure that it is perfectly open and patent. There are no concerns about prolapse because this stoma is placed at the first mobile portion of the sigmoid after the descending colon, which is normally fixed. The peritoneum and aponeurosis between both stomas are sutured together with long-term, absorbable sutures (5-0 Vicryl) (Fig. 5.16). The anterior aponeurosis is closed with the same suture material, as well as the subcutaneous tissue and Scarpa fascia. Both stomas, proximal and distal, are matured with 6-0 long-term absorbable sutures taking the skin edge, the bowel wall, and the bowel edge (Fig. 5.17).
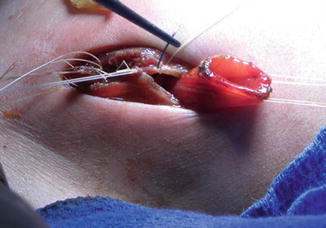
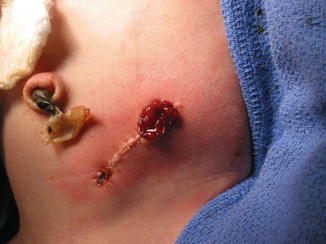

Fig. 5.16
Fixing the proximal stoma to the peritoneum and fascia. Closing the wound in between both stomas

Fig. 5.17




Both stomas are meticulously “matured.” The operation is finished
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree








