Peripheral Arterial Occlusive Disease
Charles W. Sternbergh III
David Brown is a 68-year-old retired carpenter who for the past 2 years has had cramps and aching in the right calf after walking. The discomfort has been gradually worsening and is now reproducible after he walks approximately two blocks; it subsides within 5 minutes of resting but reappears when he walks another two blocks. He denies having any pain in the left leg while walking or in the right calf or foot at rest, nor does he have any history of trauma to the extremities. He smokes two packs of cigarettes a day.
Mr. Brown’s medical history is significant for coronary artery disease (CAD), for which he underwent coronary artery bypass grafting (CABG) 3 years ago. Since the CABG, he has had no angina, dyspnea on exertion, or orthopnea. He has no history of stroke, transient ischemic attacks, or hypercholesterolemia. He has mild chronic obstructive pulmonary disease because of smoking. His only medications are diltiazem and aspirin.
A physical examination indicates that Mr. Brown is normotensive and in sinus rhythm; findings of the neck, chest, abdominal, and neurologic examinations are normal. Evaluation of his peripheral pulse reveals a 2+ carotid pulse bilaterally without bruits, 2+ radial pulses, and 2+ femoral pulses without bruits. Mr. Brown is bilaterally pulseless in the popliteal, posterior tibial, and dorsalis pedis arteries, but these vessels produce a monophasic signal when evaluated with a Doppler study. The right leg has a well-healed longitudinal scar from the excision of the saphenous vein for the CABG. There is no muscle atrophy, ulceration, or any other sign of tissue loss in either leg; capillary refill in the toes is good.
What is claudication?
View Answer
Claudication is exercise-induced intermittent discomfort in a particular muscle group that subsides within 1 to 5 minutes after the exercise is stopped. This discomfort may be described by the patient as pain, cramping, burning, or weariness. In the lower extremities, the calves, thighs, and buttocks are most frequently affected. Because the pain is reproducible by the same degree of exertion, claudication is typically quantified by the distance a patient can walk before its onset (e.g., two-block claudication).
What causes claudication?
View Answer
Claudication occurs when a particular muscle group becomes hypoxic because the increased metabolic demands for oxygen during exercise cannot be met. Normal arteries can increase flow 5- to 10-fold when regional metabolic demands rise; however, stenosed or occluded vessels have limited capacity to augment flow during exercise. The stenosis or occlusion is usually caused by progressive atherosclerosis.
What is the differential diagnosis for lower extremity pain?
View Answer
Claudication is a characteristic symptom in patients with significant chronic arterial occlusive disease. Because of the reproducibility of hypoxic muscle pain after exercise, a history and physical examination should be sufficient to rule out most other causes. The differential diagnosis for lower extremity pain includes the following:
Chronic peripheral arterial occlusive disease (PAOD): pain or weariness of the calf (most common), thigh or buttock that occurs with exercise but not at rest. The distance required to induce the discomfort should be fairly constant. The discomfort should be promptly relieved (1 to 5 min) by standing still.
Acute arterial embolism: the precipitous reduction of blood flow that results from acute arterial embolism can cause an acute onset of diffuse lower extremity pain at rest in a patient with no history of arterial occlusive disease.
Acute aortic dissection: dissection of the thoracic aorta can extend into an iliac artery, acutely compromising arterial flow and thus presenting like an acute embolus. Many patients will also complain of a “tearing” chest or back pain.
Neurologic disorders: lumbar disc herniation or spinal stenosis may cause characteristic shooting pain or extremity weakness that is sometimes quite distinct from claudication. However, other patients can have extremity complaints that are similar to that caused by PAOD. Patients who develop leg pain with standing only and those who must sit or lie down to relieve the discomfort after exercise typically have a neurologic etiology to their leg symptoms.
Diabetic neuropathy: many patients with long-standing diabetes develop significant burning pain in the feet at rest, which may be easily confused with pain caused by critical arterial ischemia.
Chronic venous disease: venous valve incompetence and the resulting relative stasis can cause chronic swelling, hyperpigmentation, and ulcers at or proximal to the malleoli.
Deep vein thrombosis: characterized by swelling in the extremities or vague pain, deep vein thrombosis cannot be accurately diagnosed from the history and physical examination.
Musculoskeletal disorders: patients with musculoskeletal disorders have a history of recent trauma or of pain associated with movement of a joint.
Infection: local erythema and tenderness that are not exacerbated by exercise are present.
What are some significant risk factors for arterial occlusive disease?
View Answer
Hypercholesterolemia, tobacco use, hypertension, diabetes mellitus, male gender, age, and hereditary influences are all significant risk factors (1).
What are the signs of significant arterial occlusive disease?
View Answer
These signs may be observed during a physical examination:
Lack of distal pulses
Pallor of the extremity on elevation and rubor on dependency
Trophic changes such as thinning of the skin, loss of hair, and thickening of the nails
Muscle atrophy
Tissue loss (e.g., ulcers distal to the malleolus or gangrene). Ulcers proximal to the malleolus are almost never primarily caused by arterial ischemia.
What is the natural course of lower extremity claudication?
View Answer
Symptomatic arterial occlusive disease has a surprisingly benign course; 75% to 80% of patients have stable or diminished claudication with conservative management (2). Reported amputation rates for all patients with claudication who are managed without surgery range from 1.6% to 7% after a 6- to 8-year follow-up (3,4). Approximately 20% of patients with claudication ultimately require invasive intervention for limb salvage.
What is an appropriate initial treatment for claudication?
View Answer
Because of the relatively benign natural course of this disease, an initial conservative approach is generally warranted. This includes the following measures:
Cessation of smoking. Tobacco use is clearly associated with a significant exacerbation of vascular occlusive disease. Smoking doubles an elderly patient’s risk of claudication (5). Most smokers with claudication show a significant improvement in exercise tolerance after quitting (6).
Exercise. A graded exercise program stimulates formation of collateral vessels. The resulting increase in blood flow can increase the walking distances by 80% to 120%. Unfortunately, these beneficial effects are sometimes difficult to achieve without a supervised and highly structured exercise program.
Aggressive modification of risk factors. PAOD is a strong marker for generalized atherosclerotic disease. As such, patients with PAOD, even if clinically asymptomatic, should be assessed for elevated cholesterol and triglycerides. Younger patients should be checked for elevations in homocysteine and perhaps LP(a). Appropriate dietary modifications and possibly drug therapy should be instituted.
Medications for claudication. Cilostazol (Pletal) has been available in the Unites States for the treatment of claudication since 1999. It significantly increases walking distance in approximately 50% of patients who take the medication. Pentoxifylline (Trental) is a less effective medication for claudication and is now rarely prescribed.
Mr. Brown’s physician instructs him to stop smoking and begin a graded exercise program, but his interest and participation in exercise are limited, and he does not stop smoking. He does not go to scheduled follow-up visits. Over the next 2 years, his walking distance before onset of the characteristic right calf pain gradually shortens. He also begins to have pain in his right foot at rest, especially at night; the discomfort is relieved by dangling the foot off the bed. The intensity and duration of the pain gradually increase, and after 3 weeks, he seeks help.
What is rest pain, and what causes it?
View Answer
Rest pain is caused by inadequate delivery of oxygen to the tissues during rest. This hypoperfusion inevitably manifests as ischemic pain in the foot at rest. The lower extremity muscles that are prone to claudication (the calf, thigh, and buttock muscles) rarely if ever exhibit rest pain because they are not at the end of the arterial tree. Conversely, the foot does not claudicate because it has relatively little muscle mass that is susceptible to exercise-induced hypoxia. By definition, the pain caused by claudication is intermittent, whereas rest pain can be continuous. Rest pain is characteristically worst at night, when the patient is supine, because the arterial flow to the foot is not aided by gravity. The pain is relieved by dangling the foot off the bed, walking a few paces, or sleeping in a chair.
What is the natural history of rest pain?
View Answer
In contrast to claudication, true ischemic rest pain ultimately progresses to limb loss in most untreated patients. An aggressive treatment regimen is therefore warranted in the absence of prohibitive comorbid medical conditions.
What are the indications for treatment of arterial occlusive disease?
View Answer
Rest pain.
Tissue loss. This may be a nonhealing inframalleolar ulcer, nonhealing distal amputation, or gangrenous changes in the toes.
Disabling claudication. The availability of minimally invasive endovascular treatments has resulted in a more liberal policy for interventional treatment of claudication in many centers.
How is arterial occlusive disease evaluated?
View Answer
A thorough history and physical examination are essential, and any comorbid medical conditions must be addressed. Segmental arterial Doppler studies and an ankle-brachial index (ABI) are obtained.
What does an arterial Doppler study measure? What is the ABI? What are pulse volume recordings (PVRs)?
View Answer
Segmental arterial Doppler studies measure the systolic pressure at several locations on the extremity. A pressure difference greater than 20 mm Hg between levels suggests significant occlusive disease. The ABI (obtained by dividing the ankle pressure by the highest brachial pressure) provides a value indicating distal perfusion. A normal ABI is 0.9 to 1.1; an ABI of 0.5 to 0.7 is typical of claudication; and an ABI of less than 0.5 may accompany rest pain or tissue loss. The ABI is only a relative number, and many patients with an ABI of 0.5 have no symptoms.
Because diabetic patients sometimes have heavily calcified arteries that are poorly compressible, their ABI may be misleadingly high. That is one reason PVRs should also be routinely obtained with the ABI. PVRs are arterial waveforms that give subjective but important information about arterial blood flow. Normal PVRs have a triphasic waveform whereas patients with significant PAOD will have a sigmoidal waveform. Patients with very severe PAOD may have a flat line PVR with no pulsatility whatsoever.
At what point does arterial stenosis become hemodynamically significant?
View Answer
The cutoff point is a 75% reduction of the cross-sectional area, which is equivalent to a 50% reduction of the diameter. At this level of stenosis, poststenotic pressure and blood flow are maintained at 90% to 95% of normal values; however, any further stenosis causes a precipitous fall in distal perfusion.
Mr. Brown’s physician orders a lower extremity segmental arterial Doppler study. It reveals a reference right brachial pressure of 130 mm Hg, high thigh pressure of 140 mm Hg, above-knee pressure of 73 mm Hg, below-knee pressure of 60 mm Hg, ankle pressure of 51 mm Hg, and toe pressure of 45 mm Hg. The ABI is calculated to be 0.39. The contralateral leg has fairly similar pressures and an ABI of 0.5.
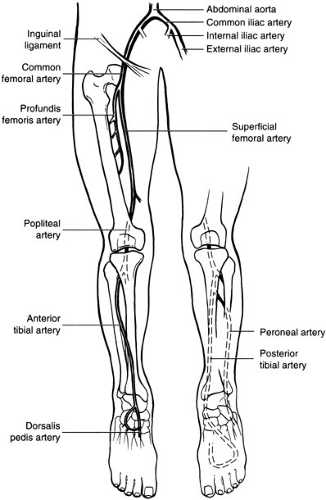
What is the anatomy of the vascular tree in the lower extremities?
How does the location of the pain suggest the probable area of stenosis or occlusion?
View Answer




In 60% to 70% of patients, the arterial lesion is one level above the claudicating muscle group. Calf claudication, as in Mr. Brown’s case, therefore suggests superficial femoral artery (SFA) or popliteal artery disease, whereas thigh or buttock claudication indicates more proximal aortoiliac occlusive disease. However, up to 40% of patients with aortoiliac disease may have calf claudication without thigh or buttock symptoms.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree