Pediatric Surgery
Daniel A Saltzman
Sean J. Barnett
Nathan Kreykes
Robert D. Acton
Author’s Note: Pediatric surgery is an encompassing field that covers many aspects of the surgical diseases of infants and children. In this chapter, we have used five cases to illustrate the more common problems encountered in pediatric surgery. If you want more information, we encourage you to examine the numerous comprehensive texts that are available that cover the realm of pediatric surgery (see Suggested Readings).
A 2-day-old term infant boy was admitted to the neonatal intensive care unit (NICU) for feeding intolerance, progressive abdominal distention, and bilious emesis. His prenatal course has been unremarkable and he has been alert and active since birth. On examination, the baby appears well. His vital signs are normal and his abdomen is moderately distended. Rectal examination reveals an anatomically normal anus and there is no meconium in the rectal vault. A complete blood count (CBC) and serum electrolytes are normal. An abdominal radiograph reveals a distal gastrointestinal obstruction.
What is the differential diagnosis for this infant’s abdominal problem and how would you proceed with a workup?
View Answer
Differential diagnosis for a distal gastrointestinal obstruction includes the following:
Jejunal-ileal atresia
Neonatal small left colon syndrome
Meconium plug syndrome
Meconium ileus
Hirschsprung’s disease
Malrotation
Colonic atresia
The workup begins with a detailed history specifically looking for a diabetic mother, family history of jejunal-ileal atresias, or family history of Hirschsprung’s disease. Infants with neonatal small left colon syndrome have a diabetic mother.
Next, an abdominal radiograph is obtained. The air-gas pattern obtained on this simple test can point you to the right diagnosis. The absence of colonic gas may indicate a more proximal atresia, Hirschsprung’s disease, or neonatal small left colon syndrome. A nonspecific gas pattern may indicate a malrotation, whereas “soap bubbles” in the right lower quadrant may indicate a meconium ileus. If you suspect malrotation or a midgut volvulus, you must exclude these diagnoses.
What do you do next?
View Answer
In this case, abdominal radiograph revealed absent colonic gas with more proximal intestinal distention. If suspected, a limited upper gastrointestinal (UGI) series should be obtained to exclude a malrotation. A contrast enema with isotonic water-soluble contrast is indicated. This study demonstrated a microcolon, that is, unused colon, indicative of a jejunal-ileal atresia (Fig. 32.1).
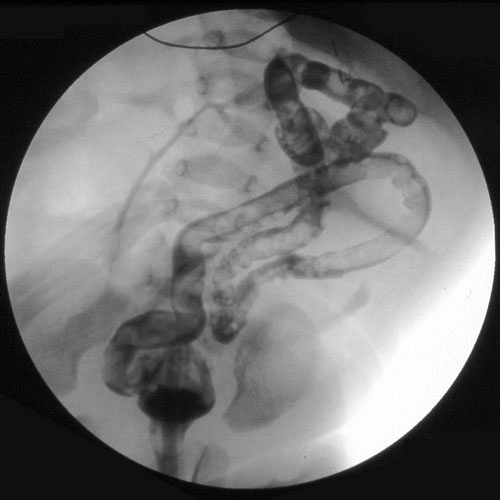 Figure 32.1. Contrast enema in newborn with jejunal-ileal atresia demonstrating a microcolon or unused colon. |
In meconium plug syndrome, intraluminal colonic masses would have been visualized.
A transition zone may be seen with Hirschsprung’s disease.
A small sigmoid and left colon with a normal caliber transverse colon is generally observed with neonatal small left colon syndrome.
A complete bowel obstruction secondary to malrotation is from the development of a volvulus. These patients are tender and appear septic and do not look generally healthy, in contrast to the way this patient presented.
Operative exploration is now indicated and no further studies are necessary.
What is the pathophysiology of jejunal-ileal atresias?
View Answer
Unlike duodenal atresia, which is thought to be a failure of recanalization, jejunal-ileal atresias are thought to arise from an intrauterine vascular accident with subsequent ischemic necrosis. Pathologically, one can see a spectrum of defects with intestinal atresias that range from a stenosis to multiple atretic segments throughout the intestine.
How are jejuno-ileal atresias treated?
View Answer




The operative procedure performed is dependent on the pathologic findings. Generally, a limited resection of the proximal dilated and hypertrophied bowel with a primary end-to-end anastomosis with or without tapering is commonly performed.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree







