and Andrea Bischoff1
(1)
Pediatric Surgery, Colorectal Center for Children Cincinnati Children’s Hospital, Cincinnati, OH, USA
21.1 Introduction
As discussed in our previous chapter, the bowel management program, consisting mainly in the administration of enemas, plus sometimes treatment with specific medication and a specific diet, greatly changes the quality of life of many children. Giving an enema to a small child is a relatively easy task. It is easy for the parents to position the child on their lap for the enema, and usually the child tolerates this procedure very well. As times goes by, as the patients grow, particularly in those patients that require an enema for long periods of time or on a permanent basis, it becomes logistically more difficult, simply because of the size of the patient. If one tries to imagine how to give an enema in a teenager, taking advantage of gravity, it is easy to understand that is difficult. Sometimes the patients’ squat on the tub to give themselves the enema, and the whole procedure becomes very messy. We have been trying to use different methods to teach teenagers to administer their own enemas while sitting on the toilet, which is not easy, because the enema is then given against gravity. We teach them to pass a Foley catheter into the rectum, to inflate the balloon inside the rectum, and while they are applying traction on the catheter, to administer the enema. This is easy to say but not easy to do. As a consequence, most teenagers need some help from another person to receive the enema, which is an embarrassing event. Imagine a 13-year-old girl receiving enemas every day with the assistance of her father or the other way around, a 14-year-old boy assisted by his mother to have an enema.
Malone, Ransley, and Kiely had a great idea [1] of creating a mechanism for the administration of an enema in an antegrade fashion. They thought that an enema could be given through an orifice created in the abdominal wall, connected to the appendix, which allowed the passage of a small catheter directly into the colon to give the enema while the patient is sitting on the toilet [2–7]. This was a very creative concept that gained popularity quickly. The original idea of Malone, Ransley, and Kiely included a technique consisting of dividing the base of the appendix, rotating the appendix 180°, and reimplanting it in the wall of the cecum, in a submucosal fashion, to avoid leakage of stool through the appendix. In retrospect, this represents a complex maneuver that we now believe is unnecessary. The basic idea of Malone and Kiely is still extremely valuable, but now we know that we do not have to go through all the surgical maneuvers they described. They also advocated the opening of the orifice in the right lower quadrant, which is something that we do not do at the present time; we prefer the umbilicus [8–10].
Fairly soon, after Malone and Kiely popularized their idea, many others [11–16] came up with different ways to achieve the same goal. Other variants included a “noninvasive” or “minimally invasive” procedure to introduce a Silastic button into the cecum. That technique became very attractive because it is minimally invasive, it does not require a big operation, and it is technically simple. It can be done under fluoroscopy, with endoscopy, or with laparoscopy. However, we have been exposed to several patients who had a button cecostomy in the past; they came to our clinic very unhappy about the multiple long-term complications and sequelae of that procedure that included malfunction of the button, leakage of stool around the device, prolapse of the colonic mucosa, and granulation tissue around the button. These problems have been seen by others [17, 18]. Many patients also dislike the visible foreign body on the abdomen and are self-conscious about it, avoiding swimming and other activities. Those patients required a revision, removal of the button, and creation of a continent appendicostomy. It is because of that experience that we do not favor the insertion of button cecostomies.
21.2 Our Preferred Technique
We believe that the essential purpose of this type of procedure is to improve the quality of life of the patient. Therefore, our goal is to perform an operation that will allow the patient to have an active life, play sports, swim, and not be embarrassed of an orifice that rather looks like a colostomy or to have to hide a plastic device protruding from the abdomen. We believe that these patients benefit the most by the creation of a little hidden, umbilical orifice that should be as inconspicuous as possible (Fig. 21.1). We create that little orifice in the deepest portion of the umbilicus, making it invisible. Yet, making a tiny orifice and avoiding stricture requires a technically challenging and meticulous surgical technique.
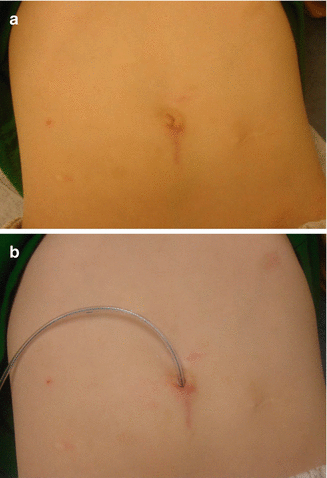

Fig. 21.1
External aspect of the abdomen of a child who underwent a continent appendicostomy operation (Malone procedure). (a) Without a feeding tube. (b) With a feeding tube
We think that we should use the appendix as much as possible. Yet, we are limited by the fact that about 30 % of the patients in whom we plan to do this operation have no appendix because it had been removed in the past for other reasons. The old surgical tradition of doing an appendectomy as part of a laparotomy luckily seems to be disappearing as surgeons become more cognizant of the potential use of the appendix for the care of the incontinent child. In addition, nowadays, urologists are using the appendix to create a conduit that goes from the abdominal wall to the bladder for intermittent catheterization which is known as a Mitrofanoff procedure (see Chap. 23, Sect. 23.13). That is another reason why the appendix is not always available for us for this operation. Because of that, we had to learn to make appendices out of the colonic or small bowel tissue. We call that a “continent neo-appendicostomy” [10]. We make the appendix out of a flap of the colonic wall that is tubularized around a feeding tube to make a new appendix. We have been doing this, mainly from the ascending colon, but we have cases in which, because of anatomic circumstances, we were obligated to make the neo-appendix from the transverse or the sigmoid colon. We have done this, in cases with multiple peritoneal adhesions or “frozen abdomens.” In such cases, we have no choice but to use that part of the colon that we have access to. Ideally, we prefer to create the new appendix from the ascending colon near the cecum but away from the ileocecal valve.
We have done approximately 200 of these operations (appendicostomies and neo-appendicostomies). On two occasions, we opened the abdomen and for a couple of hours tried to divide the multiple peritoneal adhesions between the loops of bowel and decided to abort the procedure, because we had the feeling that we would do more harm than benefit to the patient.
A patient that has his or her native appendix does not need colonic preparation to do this operation. The operation in a patient with minimal peritoneal adhesions, a thin abdominal wall, a normal appendix, and a mobile cecum becomes minimally invasive, although non-laparoscopic, because it only requires a small incision (about 4 cm long) running from the umbilicus down. The whole procedure can be done through that incision in about 1 hour; the patient can be fed the same day and discharged the following day from the hospital. On the other hand, when the patient has the appendix located in a rather bizarre position (behind the duodenum or behind the liver) or has multiple peritoneal adhesions, in addition, suffers from obesity, and has no appendix, the procedure becomes technically very demanding, taking an unpredictable number of hours. In similar cases, provided the peritoneal adhesions are not too dense, the laparoscopy may be helpful to avoid a laparotomy in mobilizing the cecum.
It is very important, prior to the planning of these operations, to know whether or not the patient has an appendix. Some radiologists are very optimistic and believe that an ultrasound is a reliable study to determine whether or not the patient has an appendix, but we all know that such a study is not 100 % accurate in visualizing a normal appendix. A contrast enema that shows an appendix gives us 100 % evidence that the patient has one, but if the contrast enema does not show an appendix, it does not mean necessarily that the patient does not have an appendix. A CT scan seems to be a better study.
The importance of learning about the presence or absence of an appendix prior to the operation resides in the fact that creation of a neo-appendix requires full bowel preparation with administration of GoLYTELY. It is not advisable to make a new appendix with a colon full of stool which would increase the chances of infection. We are very proud of the fact that we have not had any cases of infection. In case of doubt, therefore, we go ahead with a total bowel preparation the day before surgery with GoLYTELY as described in the corresponding chapter in this book (see Chap. 7).
Continent appendicostomy and neo-appendicostomy, in our experience, have two main late sequelae or complications: one is stricture (or acquired atresia) of the little stoma that we create between the tip of the appendix or neo-appendix and the skin of the umbilicus. The other is the problem of leakage of stool.
In our series, the frequency of stricture or acquired atresia was 18 %. In trying to avoid this problem, we have been practicing a technique that takes time to learn and to master, but we believe will eventually decrease the frequency of stricture. This technique consists of creating a triangle of skin from the umbilicus that will be accommodated in a spatulated appendix (Fig. 21.3) [9].
Concerning the problem of leakage of stool through the appendix, it is very common to hear that some authors believe that the appendix is naturally continent. This we found to be true, half of the time. The leakage of stool through the Malone orifice occurred in 2.9 % of our cases who underwent a plication of the cecum around the appendix, and in contrast, it occurred in 29 % of those cases without plication. In addition, during the performance of many of our continent appendicostomy procedures, prior to making a decision about plication or no plication of the cecum around the appendix, we tested the natural continence of the appendix by finger clamping the ascending colon and the terminal ileum and injecting saline solution through a feeding tube introduced in the cecum through the tip of the appendix. Once the cecum was full with saline solution, the feeding tube was removed, and we then observed if the saline solution leaked through the tip of the appendix. Interestingly, we found that about half of the appendices that we tested leaked. In addition, some patients who had no leakage during this test turned out to leak stool after the operation. Because of that, we recommend to create an anti-leakage mechanism by plicating the wall of the cecum around the appendix or the neo-appendix. This plication does not guarantee that the patient will not leak, since about 2.9 % of our cases still leak, despite the plication. But we believe that we should give the patient the maximum possibility of avoiding leakage, which is a very uncomfortable complication and requires a full reoperation to tighten the cecal plication.
The laparoscopic approach to perform operations for the administration of antegrade enemas, of course, is very appealing [19–24]. For those who believe that these patients do not need plication of the colon around the appendix, the laparoscopic approach becomes the ideal way to do this operation, since all the surgeons have to do is to find the appendix, grab it, and exteriorize it and to perform the anastomosis to the deepest portion of the umbilicus. This becomes an extremely easy and fast procedure. However, some of those patients eventually may leak (29 % in our experience) stool through the Malone orifice. The plication of the cecum around the appendix is usually not done laparoscopically; it must be done through an infraumbilical incision of the same size of the incision that we use. Laparoscopy is essentially used to mobilize the cecum. Also, if the patient has no appendix, one has to make one from a flap of the colon. That has not been done laparoscopically as far as we know.
One way to approach this problem in a patient in whom we do not know whether he/she has an appendix, and we do not know whether the patient has many peritoneal adhesions and also do not know where the appendix is located, could be to start the operation laparoscopically. Using one or two ports to examine the peritoneal cavity, if it turns out that the patient has a mobile appendix and cecum, a 4-cm subumbilical incision is created through which the operation (including the cecal plication) is performed. If the patient has a fixed cecum and appendix or a retrocecal or mislocated appendix in a difficult location, the laparoscopic part of the procedure is extremely beneficial to mobilize the cecum and appendix, avoiding a big laparotomy.
Pediatric urologists have been using the appendix, implanted in the bladder, as a conduit to perform intermittent catheterization, a procedure that is known as “Mitrofanoff operation” in recognition to the doctor who designed the operation (see Chap. 23) [25]. They frequently must perform this procedure in patients who suffer from both urinary and fecal incontinence. As a consequence, many pediatric urologists are doing the Malone procedure or one of its variants [26–35].
There is no question that the Malone procedure benefits many patients, and that explains why this operation is so popular [36–48].
Some surgeons and gastroenterologists advocate the Malone procedure in cases of constipation “resistant to medical management” [49–52]. We are skeptical about this indication and have the feeling that it represents an overuse of the procedure, a “quick way” to take care of a rather serious problem (see Chap. 25). The doctors who perform a Malone procedure in patients suffering from “non-manageable constipation” do not define what “non-manageable” means, and we feel that many of the operated patients could be managed medically following our protocol.
21.3 Surgical Technique: Continent Appendicostomy
We recommend not performing this operation in an extremely obese patient, because the abdominal wall may be so thick that the entire length of the appendix is not enough to reach the skin comfortably. We encourage these types of patients to lose weight prior to these operations. The risk of infection also increases significantly in obese patients.
If we have evidence that the patient has no appendix, or we are not sure, we perform a full bowel preparation with GoLYTELY (see Chap. 7). If we have evidence that the patient has an appendix, then the patient does not need bowel preparation.
The patient is taken to the operating room and the skin of the abdomen is prepared, with special emphasis on the umbilicus. We open with an incision in the midline, running from the deepest portion of the umbilicus down in the midline for approximately 4 cm, which is enough for us to introduce two fingers into the peritoneal cavity. We explore the right lower quadrant.
Frequently, we find a very mobile cecum with a very healthy appendix which we can exteriorize through the little incision below the umbilicus. When laparoscopy is used, the cecum is mobilized and then the small infraumbilical incision is made. Occasionally the surgeon may find that the patient has a very short appendix. Fig. 21.6 illustrates a surgical technique designed to elongate the appendix.
The appendix and cecum are exteriorized. Then, we create windows between the appendiceal vessels (Fig. 21.2a, b). We use these windows to pass the wall of the cecum through them, to be able to plicate the cecum around the appendix, without producing vascular compression that may produce appendiceal ischemia. We use 5-0 silk stitches to plicate the cecum around the appendix (Fig. 21.2c). Prior to the plication, we place two 6-0 silk stitches at the tip of the appendix. The tip of the appendix is then opened with a needle-tip cautery in between both stitches. A no. 8 feeding tube is passed through the tip of the appendix into the cecum. The plication of the cecum should be done on the lateral wall of the cecum and not into the medial portion. If we make it into the medial portion of the cecum, there is a possibility that we produce an obstruction of the ileocecal valve (Fig. 21.2d, e). The stitches of the plication take a full thickness bite of the cecum and a small bite of the seromuscular layer of the appendix. Every time we tie the stitches, we have to be sure that we are not compressing the blood supply of the appendix, and we make sure we are not narrowing the channel, checking by passing the catheter through it. We look at the blood supply of the tip of the appendix to be sure that it is viable. The cecum is then sutured to the anterior abdominal wall around the umbilicus with interrupted 5-0 long-term absorbable sutures. The ventral part of the tip of the appendix then is spatulated by making an incision (Fig. 21.3a–c). Special care must be taken to cauterize the distal end of the appendiceal artery, and we do not hesitate to ligate it with a 5-0 suture. A triangle of skin at the umbilicus is created (Fig. 21.3a–c). The tip of the triangle is sutured to the angle of the spatulated appendix (Fig. 21.3d); the edges of the triangular skin flap are sutured to the edges of the spatulated appendix with interrupted 6-0 long-term absorbable sutures (Fig. 21.3d–g) creating a Y-to-V anastomosis. The midline aponeurosis of the abdomen is closed with long-term absorbable sutures, as well as the subcutaneous tissue taking care to recreate the interior umbilical fold. The skin is closed with subcuticular 5-0 long-term absorbable monofilament suture. The no. 8 feeding tube is left in place fixed to the skin with a silk stitch (Fig. 21.3h). The cosmetic effect of this operation is excellent. This operation takes approximately 45 min in a patient who is thin, has minimal peritoneal adhesions, and has a mobile cecum and appendix. As I previously mentioned, the operative time may get much longer in an obese patient with peritoneal adhesions, a fixed cecum, a mislocated appendix, or an absent appendix.
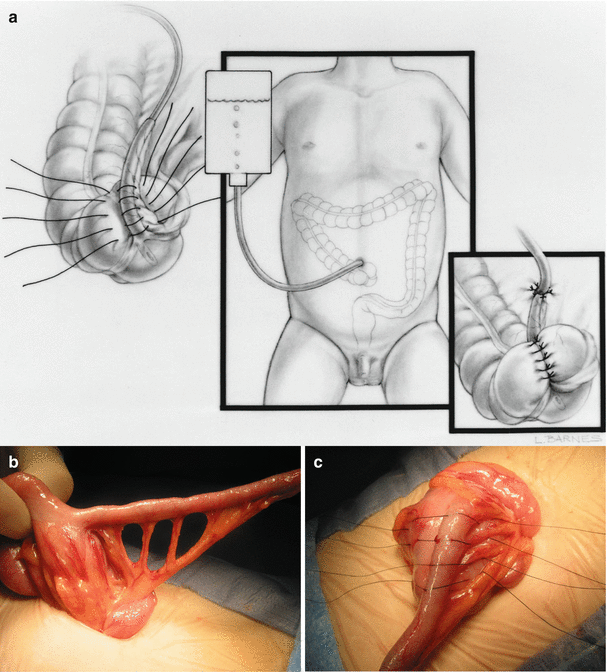
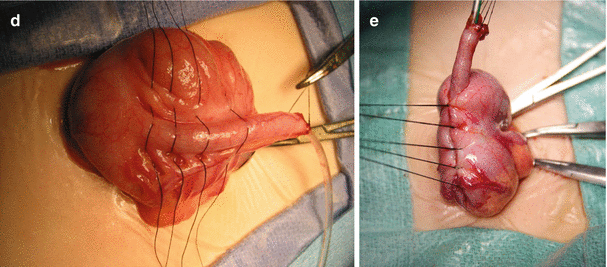
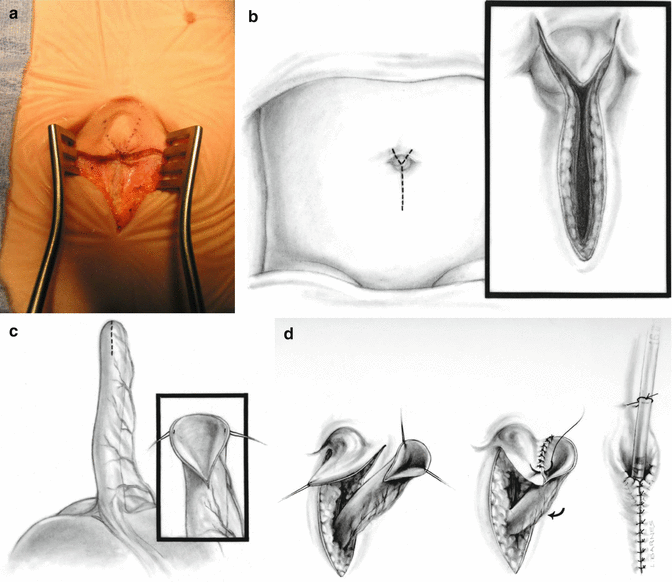
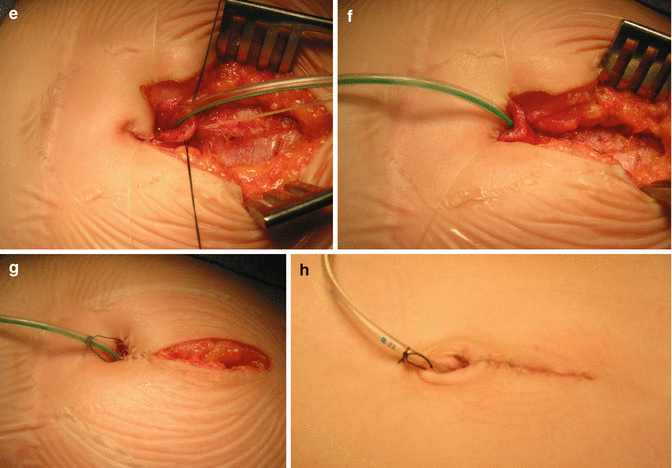


Fig. 21.2
Continent appendicostomy. (a) Diagram. (b) Creation of windows between the appendiceal vessels. (c) Placing sutures for the cecal plication, avoiding the vessels. (d) Appendix laid down lateral to the cecum, away from ileocecal valve. (e) Plication finished


Fig. 21.3
Anastomosis of appendix to the skin of the umbilicus. (a) Intraoperative picture. (b) Diagram. (c) The tip of the appendix is spatulated (diagram). (d) The triangular skin is accommodated into spatulated space, created at the tip of the appendix. Many 6-0 Vicryl sutures are used (diagram). (e–g) Intraoperative aspect of the reconstruction. (h) Final aspect of the maneuver
Sometimes, we open the abdomen with the incision that we described, only to find that the cecum is not located in the right lower quadrant, and we cannot feel it with our fingers. At that point, the alternative is to extend the incision all of the way to the lower abdomen and the upper abdomen and look for the cecum that sometimes is located in the area of the duodenum or located retrocecally, with the tip of the appendix located all of the way up into the area of the liver. Alternatively, we can use the laparoscope to look for the cecum and the appendix to mobilize and bring them through the small incision previously described.
21.4 Continent Neo-appendicostomy
The patient receives a total bowel preparation. The skin is prepared in the way described for a continent appendicostomy. The midline abdominal incision is made, long enough to mobilize the cecum and most of the ascending colon.
Usually, this type of procedure requires dividing of the normal attachments of the cecum and ascending colon from the right gutter. We have to take down those attachments in order to bring the cecum and part of the ascending colon through the wound with no tension.
We have learned through the performance of over 50 cases of continent neo-appendicostomy to create a narrow and long vascularized flap of the colonic bowel and yet to preserve an excellent blood supply to the tip of the flap. This is achieved by creating the flap following the direction of the mesenteric vessels that run in the colon (Fig. 21.4a). Looking at the normal blood supply of the colon, one can see that the mesenteric vessels of the ascending, transverse, and descending colon run perpendicular to the main axis of the colon. Therefore, the flaps that we develop in the colon should be created perpendicular to the main axis of the colon (Fig. 24.1a, b). That way, one can make a very long, narrow flap, narrow enough to be tubularized around a no. 8 feeding tube (Fig. 21.4d) with an excellent blood supply running through the length of the flap. When making this flap in the ascending colon, the surgeon must keep in mind that the right ascending colon is going to be moved toward the midline in order for the tip of the neo-appendix to be exteriorized through the umbilicus. Therefore, we specifically recommend making the base of the flap in the lateral part of the ascending colon away from the ileocecal valve. The flap must be created identifying two good mesenteric vessels at the center of the base of the flap (Fig. 21.4a, b). Those vessels run in the main direction of the longitudinal axis of the flap. The flap is raised (Fig. 21.4c). The anterior wall of the colon is closed with two layers of sutures; the first one is a running locked suture of 5-0 long-term absorbable sutures, and the second one is done with interrupted 5-0 long-term absorbable sutures. The flap is tubularized and sutured around a no. 8 feeding tube with multiple interrupted 6-0 long-term absorbable sutures. The area of the taenia of the colon is not elastic, and therefore, we intentionally leave more tissue in that part of the flap in order to be able to surround the no. 8 feeding tube. We have been happily surprised by the good blood supply of these long narrow neo-appendices, provided we preserve the mesenteric vessels. The neo-appendix is then laid down on the anterior wall of the colon somewhat askew so the suture line of the neo-appendix does not lie on the suture line of the colonic wall, which is plicated using 5-0 silk stitches in the way that was described before, when we discussed the continent appendicostomy (Fig. 21.2c, d).
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree








