and Andrea Bischoff1
(1)
Pediatric Surgery, Colorectal Center for Children Cincinnati Children’s Hospital, Cincinnati, OH, USA
12.1 Introduction
Imperforate anus without fistula is a very unique kind of defect (Fig. 12.1). Most likely, it has a very different embryologic origin, considering its uniqueness, type of associated defects, and intrinsic anatomy. In the spectrum of anorectal malformations, one can see that the frequency of associated defects is very much related with the height of the location of the fistula. Thus, a perineal fistula type of malformation usually is rarely associated to other defects, whereas a recto-bladder neck fistula seems to have the highest incidence of associations with other malformations mainly in the urinary tract. From that point of view, an imperforate anus with no fistula represents an exception because it is extremely unusual for these patients to have other associated defects such as tethered cord and abnormal sacrum.
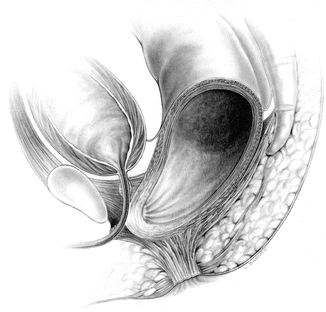

Fig. 12.1
Diagram showing the intrinsic anatomy of imperforate anus without a fistula
The most important feature of this particular defect is the fact that it represents approximately 4 % of all anorectal malformations, and half of the cases are Down syndrome [1]. In addition, from all patients with Down syndrome suffering from anorectal malformations, over 95 % of them have this specific type of defect. This fact represents a fascinating and unique opportunity to speculate and investigate anorectal malformations from the genetic point of view. It is also interesting to know that, as mentioned before, half of the anorectal malformations without fistula suffer from Down syndrome and the other half seem to have a higher incidence of association with other neurologic defects such as absent corpus callosum.
Approximately 1.1–2.2 % of patients with Down syndrome have an anorectal malformation [2–4], and the overwhelming majority has no fistula.
The association of Down syndrome and anorectal malformation without fistula may occur in identical twins [5].
The literature, prior to 1980, reported a high incidence of this defect [6]. Stephens reviewed his own series and those of eight authors and found that approximately 10 % of all cases of ARM suffered from this condition. We believe that those series included many misdiagnosed cases, in whom a fistula was not demonstrated due to a lack of adequate imaging technology. Even at present time, we see cases that come to our center with a diagnosis of anorectal malformation “without fistula,” based on a distal colostogram done with an inadequate technique (lack of hydrostatic pressure). When we repeat the distal colostogram, applying enough hydrostatic pressure, a fistula is demonstrated (Fig. 12.2).
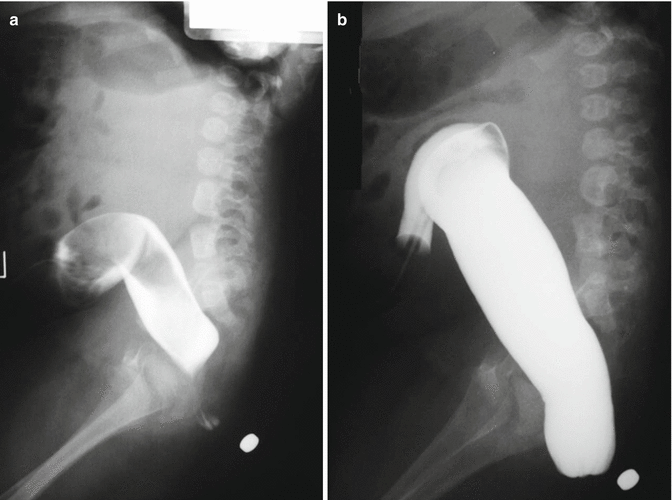

Fig. 12.2
Distal colostogram done in a patient without a fistula. (a) The lack of hydrostatic pressure gives the false impression that the rectum ends at the pubococcygeal line. (b) Increased hydrostatic pressure allows us to see the real location of the blind end of the bowel
12.2 Anatomic Characteristics
Figure 12.1 shows a diagram of an imperforate anus with no fistula. Interestingly, the blind end of the rectum is located at the same level of the bulbar urethra in the overwhelming majority of cases. In the past, the literature referred to imperforate anus with no fistula, dividing the cases into “high” and “low” location of the rectum [6].
In our series of 83 cases, 76 of them had the rectum located at the level of the bulbar urethra. Five cases had the blind rectum located at the level of the prostatic urethra, and we have only seen two blind rectums, floating into the peritoneum [7]. That is an extremely unusual defect, and we believe it belongs to another category. This is a debatable issue [8].
Some authors suggest that the absence of fistula may contribute for these patients to suffer from colon perforation earlier than those with fistula [9]. The diagram in Fig. 12.1 shows that the rectum and the posterior urethra share a long common wall. This means that the repair of this malformation is not necessarily easier than the one of a rectourethral fistula since the surgeon has to work in that common wall and separate the rectum from the urinary tract preserving intact the last one.
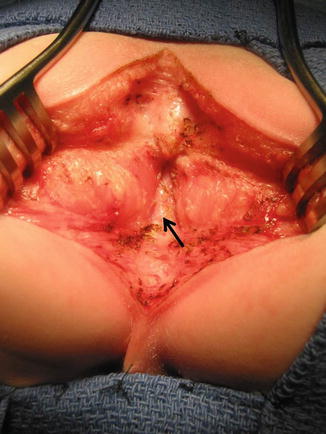
12.3 Main Repair
The posterior sagittal approach represents the ideal way to repair this malformation [1, 7, 10]. A Foley catheter is inserted in the bladder. The patient is turned into the prone position, with the pelvis elevated. The skin of the perineum and both buttocks are washed, prepped, and draped in the usual manner. A midline incision is done with the needle-tip cautery running from the middle portion of the sacrum down to the base of the scrotum. The incision divides the skin, subcutaneous tissue, parasagittal fibers, and muscle complex. After the parasagittal fibers have been divided, we go through the ischiorectal fossa to find the levator mechanism. When the levator muscle is divided, a white fascia appears very clearly (Fig. 12.3). This white fascia must be divided and separated from the real bowel wall. There is no way to injure the urinary tract in these patients because the rectum bulges right through the wound. Two 5-0 silk stitches are placed taking the posterior rectal wall, and the wall is opened with the needle-tip cautery. We continue opening the rectum distally to reach its blind end, to confirm that there is no fistula. As we open the posterior rectal wall, 5-0 silk stitches are placed taking the edges of the rectum to expose the inside lumen of the rectum. Figure 12.4 shows the lumen of the rectum in a patient with imperforate anus with no fistula. The surgeon must remember at this point that the anterior rectal wall is intimately attached to the posterior urethra and will require a meticulous dissection in order to separate the rectum without injuring the urinary tract. For that, multiple 5-0 silk stitches are placed taking the edge of the rectum in its lowest portion, and the dissection is done using uniform traction. Applying uniform traction with multiple silk stitches, a circumferential dissection is performed dividing bands and vessels that held the rectum up in the pelvis (Fig. 12.5). Since the rectum is located significantly low, once it is completely separated, usually it requires a rather minor dissection to gain enough length to achieve a low-tension anoplasty. In this particular malformation, it is not uncommon to find a very dilated rectum since the patient had no fistula. Therefore, the chances for this patient to require tapering of the rectum are higher than in other cases of anorectal malformations. This is particularly true in those patients who have spent a long time, from the time of colostomy until the time of the main repair. If the rectum is too bulky, it must be tapered, and for that, we resect the posterior aspect of the rectal wall and closed the rectum with two layers of interrupted long-term absorbable sutures (Fig. 12.6). The rectum is then placed in front of the levator mechanism, which is closed with 5-0 interrupted long-term absorbable sutures. The posterior edges of the muscle complex on each side of the midline are reapproximated in the midline and sutured with interrupted 5-0 long-term absorbable sutures, taking a bite of the posterior rectal wall to anchor the rectum in a good position. The anoplasty is performed in the center of the sphincter with 16 circumferential stitches of 6-0 Vicryl sutures. The ischiorectal fossa is obliterated with the same suture material as well as the subcutaneous tissue, and the skin is closed with a subcuticular monofilament absorbable suture. These patients require minimal medication for pain. They can eat and drink the same day as surgery. The Foley catheter can be removed the next day. Dilatations are started 2 weeks after surgery according to our protocol.