Picture Quiz, MCQs, and Brief Information
Q-1. This patient presented upper abdominal pain radiating to the back with abdominal distension. On examination, hepato-splenomegaly, ascites, and a palpable gallbladder were found. The patient also had peripheral edema. He recently developed jaundice. What is the likely diagnosis?

Figure 106
MCQ-1. The following are true or false for carcinoma pancreas?
1. Cigarette smoking increases the risk 1.5 times?
2. The classical triad of symptoms is pain, abdominal mass, and diarrhea?
3. Painless jaundice as a presentation for pancreatic head tumors has a poor prognosis?
4. Tumor-related antigens offer little help in diagnosis even in late disease?
Ans. to MCQ.
1. True (risk is proportional to number of cigarettes smoked).
2. False (the classical triad is pain, jaundice, and weight loss with anorexia).
3. False (it has a good prognosis, as there is early obstruction and early detection).
4. False (carcinoembryonic antigen, pancreatic oncofetal antigen, CA 19-9, DuPan-2, pancreatic cancer-associated antigen, and CA 50 offer a good chance of diagnosis, but are present late in disease).
Applied medicine. Pancreatic cancer.
• About 90 percent of the pancreatic cancers are ductal adenocarcinomas of exocrine pancreas.
• Pancreatic head tumors are twice as common.
• The five-year survival is about 5 percent.
• Risk factors include cigarette smoking, obesity, and nonhereditary chronic pancreatitis.
• Glucose intolerance can occur.
• In CT, look for pancreatic mass, dilated bile, or pancreatic ducts or evidence of metastasis.
• ERCP is also widely used for diagnosis of pancreatic cancer, especially when CT and ultrasound are negative. It can also provide brushing samples for cytology or for stenting a stricture.
• MRI does not offer any advantages over CT, but MRCP may be better than CT for defining the anatomy of the pancreatic duct and biliary tree.
• CA 19-9 has a sensitivity and specificity of about 80 to 90 percent. It is more of a prognostic indicator.
Ref: Harrison’s Principles of Internal Medicine.
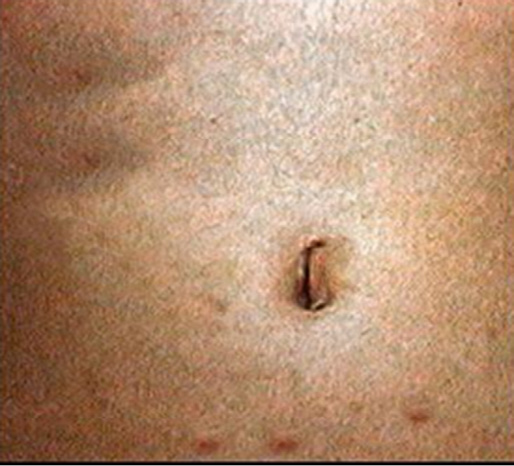
Figure 107
MCQ-2. The following are true or false for typhoid fever?
1. Relapses usually occur at the peak of antibody titer?
2. Intestinal bleeding occurs in the first week after fever?
3. Perforation is usually sterile?
4. When Vi antigen is positive, the O and H may be negative?
Ans-MCQ.
1. True.
2. False (usually in the second or third week of fever).
3. True (frank signs of peritonitis are usually lacking).
4. True (Vi antigen inhibits O and H agglutination).
Applied medicine. Typhoid fever.
• Typhoid is acquired through contaminated food or water.
• Decreasing the stomach acidity increases the susceptibility.
• Fever at presentation is present in around 75 percent of the cases. It can continue for four weeks in untreated cases.
• Abdominal pain is reported in only 30 to 40 percent.
• The incubation period is 10 to 14 days (range 3 to 21 days).
• GI symptoms included anorexia (55 percent), abdominal pain (30 to 40 percent), nausea (18 to 24 percent), vomiting (18 percent), diarrhea (22 to 28 percent), or constipation (13 to 16 percent).
• On examination, one may find a coated tongue (51 to 56 percent), splenomegaly (5 to 6 percent), and abdominal tenderness (4 to 5 percent). Rash (rose spots seen in 30 percent by the seventh day), hepatosplenomegaly (3 to 6 percent), and epistaxis. A relative bradycardia at the peak of high fever is also indicative of typhoid (also seen in viral fevers).
• Common complications include gastrointestinal bleeding (10 to 20 percent) and intestinal perforation (1 to 3 percent) usually seen in the third and fourth weeks of illness from hyperplasia, ulceration, and necrosis of the ileocecal Peyer’s patches at the initial site of salmonella infiltration.
• Neurologic manifestations occur in 2 to 40 percent and include meningitis, Guillain–Barré syndrome, neuritis, and neuropsychiatric feature (muttering delirium or coma vigil), with picking at bedclothes or imaginary objects.
Ref: Harrison’s Principles of Internal Medicine.

Figure 108
MCQ-3. Give true or false in relation to cirrhosis of the liver?
1. Rarely, spider angioma may be found on the lower limbs?
2. Asterixis is present in grade IV hepatic encephalopathy?
3. Dupuytren’s contracture and parotid enlargement are predominantly seen in alcoholic cirrhosis?
4. Cyanosis with clubbing may be seen in cirrhosis?
Ans-3. The patient has spider angioma on the face with mild jaundice.
This along with history of abdominal distension and recent hematemesis suggests cirrhosis and variceal bleeding.
Ans-MCQ.
1. True (this was described by Gabuzda, therefore called Gabuzda spider).
2. False (asterixis is present in grade-1 and II encephalopathy. In grade IV, patient is in deep coma).
3. True (Dupuytren’s contracture is related to alcoholism and not to cirrhosis).
4. True (cyanosis is a rare feature of cirrhosis due to marked intrapulmonary shunting. It is called hepato-pulmonary syndrome. Mild clubbing is more common in primary biliary cirrhosis).
Applied medicine. Alcoholic liver disease.
• The spectrum of alcoholic liver disease varies from asymptomatic patient, fatty liver, or steatosis, acute alcoholic hepatitis to cirrhosis of the liver.
• Lab features suggesting alcohol liver disease include high gamma-glutamyl transferase, peripheral blood marcocytosis, and AST is much greater than ALT, and the ratio is usually greater than 1.5.
• Stopping alcohol is the most important step in treatment. Fatty liver might disappear within three months of abstinence.
• With acute alcoholic hepatitis about 30 percent patients may die if the PT is significantly prolonged.
• In alcoholic cirrhosis, only 50 percent patients might survive for five years.
• In alcoholic hepatitis, there is a long history of heavy alcohol intake jaundice, anorexia, fever, and tender hepatomegaly. A bruit heard over the liver in half the cases.
Ref: Davidson principle and practice of medicine.

Figure 109
MCQ-4. Give true or false for each of the following statements?
1. Values of antithrombin-III only slightly below normal increasing the risk of thrombosis?
2. Portal vein thrombosis (PVT) may occur in cirrhosis?
3. Patients with antithrombin deficiency with acute thrombosis or embolism can be treated with antiplatelets?
4. Deficiency of protein C (a vitamin K-dependent hepatic protein) is associated with bleeding tendency?
Ans-MCQ.
1. True.
2. True.
3. False (heparin is given).
4. False (recurrent thrombosis).
Applied medicine. Portal vein thrombosis.
• There is portal hypertension and reduction in the blood supply of the liver.
• It may be complete or incomplete. It is also important to know how extensive it is, for example, whether involving the superior mesenteric vein.
• It may be a complication of cirrhosis of liver or hepatocellular carcinoma.
• Another important underlying cause is portal pyemia from abdominal sepsis, and occasionally associated with acute pancreatitis.
• It is a known complication of splenectomy.
• Do power Doppler, while CT angiography (venous phase) is not always required.
• Patient may be asymptomatic (especially in chronic PVT) and first diagnosed after hematemesis due to bleeding esophageal varices.
• Signs of chronic liver disease are present if underlying cirrhosis is present.
• Ascites and splenomegaly may be seen.
• Acute PVT causes intestinal congestion and ischemia, which is associated with abdominal pain, diarrhea, rectal bleeding, abdominal distention, nausea, vomiting, anorexia, fever. Lactic acidosis and sepsis may be found. Splenomegaly is due to portal hypertension.
Ref: Harrison’s Principles of Internal Medicine.
Q-5. This is a barium swallow of a patient with hematemesis. What does it show?

Figure 110
MCQ-5. Give true or false for each of the following statements?
1. Wedged hepatic vein pressure is normal in sinusoidal and postsinusoidal portal hypertension and elevated in presinusoidal portal hypertension?
2. Portal-systemic shunt surgery improves survival rates in patients with cirrhosis?
3. Beta-blockers reduce the splanchnic arterial and portal venous pressure?
4. Dose of propranolol is titrated to reduce the blood pressure (BP) by 25 percent?
Ans-MCQ.
1. False (elevated in sinusoidal and postsinusoidal and normal in presinusoidal portal hypertension).
2. False (only incidence of variceal bleeding is reduced, but encephalopathic complication increases).
3. True.
4. False (dose is adjusted to reduce the resting pulse by 25 percent).
Applied medicine. Esophageal varices.
• Variceal hemorrhage has 20 to 30 percent mortality with each episode of bleeding.
• About one-third of the patients with cirrhosis have varices.
• About one-third of the patients with varices will develop bleeding.
• Predictors of variceal bleeding include severity of cirrhosis (Child’s class); higher wedged-hepatic vein pressure; larger the size of varices; the location of the varix; and endoscopic stigmata like red wale signs, hematocystic spots, diffuse erythema, bluish color, cherry-red spots, or white-nipple spots. Patients with tense ascites also have an increased risk.
• Treatment of esophageal varices includes prophylaxis with beta blockade or primary prophylaxis with EVL.
 Endoscopic variceal ligation (EVL) or endoscopic sclerotherapy.
Endoscopic variceal ligation (EVL) or endoscopic sclerotherapy.
 Octreotide or somatostatin as splanchnic vasoconstrictors.
Octreotide or somatostatin as splanchnic vasoconstrictors.
 Balloon tamponade (Sengstaken–Blakemore tube or Minnesota tube) if endoscopy is not available or awaiting surgery in rare cases.
Balloon tamponade (Sengstaken–Blakemore tube or Minnesota tube) if endoscopy is not available or awaiting surgery in rare cases.
 Transjugular intrahepatic portosystemic shunt (TIPS) is considered for patients who fail to respond to the aforementioned measures.
Transjugular intrahepatic portosystemic shunt (TIPS) is considered for patients who fail to respond to the aforementioned measures.
• Surgical esophageal transection is rarely required.
Ref: Harrison’s Principles of Internal Medicine.

Figure 111
MCQ-6. In relation to gynecomastia, give true or false.
1. In Klinfelter’s syndrome, it is bilateral and painless?
2. True gynecomastia can be separated from lipomastia by mammography or ultrasonography?
3. Early gynecomastia is characterized by proliferation in the breast of the fibroblastic stroma?
4. The normal ratio of production of testosterone to estradiol in adult men is 50:1?
Ans-6. Cimetidine, ranitidine, mesoprostal, and omeprazole.
Ans-MCQ.
1. True
2. True.
3. False (there is proliferation of both fibroblastic stroma and the ductal system).
4. False (100:1).
Applied medicine. Peptic ulcer disease.
• Duodenal and gastric ulcers are most commonly found in association with NSAID or H. pylori.
• The most well-known complications include bleeding, perforation, and gastric outlet obstruction.
• Tests for H. pylori include rapid urease, histology, serology, urea breath test, and stool antigen (all being about 90 percent specific and sensitive). Culture can also be done and may suggest the sensitivity to drugs. Serology will remain positive after previous exposure and treatment.
• The classical and historical features of peptic ulcer disease (PUD) include chronicity, periodicity, pointing sign, and relation to meals.
• Zollinger–Ellison syndrome is suspected and a fasting gastrin level sent when there are multiple ulcers, at unusual sites, strong family history of ulcer disease, there are recurrences, there is basal hyperchlorhydria, unexplained diarrhea, hypercalcemia suspicion of multiple endocrine adenomatosis, or prominent gastric or duodenal folds.
• Type A chronic gastritis affects the fundus and body with antral sparing classically associated with pernicious anemia.
• Type B chronic gastritis is antral predominant and associated with H. pylori.
Ref: Harrison’s Principles of Internal Medicine.

Figure 112
MCQ-7. In relation to jaundice, give true or false for each of the following statements.
1. Obstructive jaundice has a greenish tinge?
2. Hemolytic jaundice has an orange tinge?
3. Dark coca cola urine suggests obstructive jaundice?
4. Bradycardia is feature of hemolytic jaundice?
Ans-MCQ.
1. False (hemolytic jaundice has a greenish tinge).
2. False (obstructive jaundice has an orange tinge).
3. False (it is a feature of hemolytic jaundice).
4. False (it is a feature of obstructive jaundice).
Applied medicine. Obstructive jaundice.
• Conjugated biliary obstruction, intrahepatic cholestasis, hepatocellular injury, or an inherited condition.
• With high probability of obstruction, do ultrasound, magnetic resonance cholangiopancreatography (MRCP), endoscopic retrograde cholangiopancreatography, to look for evidence of intra- or extra-hepatic bile duct dilation.
• Also, do antimitochondrial antibody for primary biliary cholangitis.
• If negative, look for hepatocellular disease.
• With high probability of extra-hepatic obstruction, endoscopic ultrasound may be useful.
• For suspected hepatic injury, do serologic tests for viral hepatitis, antimitochondrial antibodies, antinuclear anti-smooth muscle, liver-kidney microsomal antibodies for autoimmune hepatitis, serum iron, transferrin, and ferritin for hemochromatosis. Also, do ceruloplasmin for Wilson disease, alpha-1 antitrypsin activity for alpha-1 antitrypsin deficiency, thyroid function tests, antibody screening for celiac disease, and test for adrenal insufficiency where clinically indicated.
• Inherited conditions associated with conjugated hyperbilirubinemia include Dubin–Johnson syndrome and Rotor syndrome.
Ref: UpToDate medicine.

Figure 113
MCQ-8. In relation to the diagnosis, give true or false for each of the following statements.
1. There is history of eating canned food?
2. There is an ascending paralysis?
3. Unilateral cranial palsies are common?
4. Patients may die of cardiac failure?
Ans-MCQ.
1. True.
2. False (descending).
3. False (bilateral).
4. False (respiratory).
Applied medicine. Botulism.
• It is caused by neurotoxin elaborated by the clostridium botulinum. A disease acquired via contaminated food with predominant neurological features.
• It can be food-borne (enteric infectious botulism), via inhalational and through wound and rarely iatrogenic botulism via receiving the toxin for cosmetic reasons.
• Classical features include acute onset of bilateral cranial neuropathies associated with symmetric descending weakness without sensory defects. There is no fever. There may be bradycardia.
• Myasthenia gravis, Eaton–Lambert syndrome, Guillain– Barré syndrome, tick paralysis, poliomyelitis, stroke, and heavy metal intoxication need to be excluded as differential diagnosis.
• Demonstration of toxin in the blood is diagnostic. Analysis of stool, vomitus, and suspected food items may also reveal the toxin. EMG studies may help in the diagnosis.
• Patients may die of respiratory failure.
• Antitoxin with penicillin G or metronidazole is used in most cases.
Ref: Harrison’s Principles of Internal Medicine.

Figure 114
MCQ-9. In relation to the Budd–Chiari syndrome, give true or false for each of the following statements.
1. Paroxysmal nocturnal hemoglobinuria may be responsible?
2. It may be seen in essential thrombocythemia?
3. It may be associated with lupus anticoagulant?
4. It is associated with pregnancy?
Ans-9. Abdominal ultrasound with Doppler may confirm the Budd–
Chiari syndrome. The ascites in this case is usually resistant to diuretics and salt restriction.
Ans-MCQ.
1. True.
2. True.
3. True (it is associated venous and arterial thrombosis and recurrent miscarriages).
4. False.
Applied medicine. Budd–Chiari syndrome.
In any suspected or confirmed case, look for an underlying cause, for example, hepatocellular carcinoma (most common), other malignancies, myeloproliferative disorders, JAK2 mutation. Predisposition increases with exposure to oral contraceptives, in pregnancy, and postpartum period.
• Look for hypercoaguable states, including Factor-V Leiden gene mutation, protein C deficiency, protein S deficiency, antithrombin III deficiency, antiphospholipid syndrome, and hyperhomocysteinemia. Rarely, it may be associated with paroxysmal nocturnal hemoglobinuria and Behcet’s syndrome.
• Subacute or chronic Budd–Chiari syndrome usually presents with ascites hepatomegaly and varices (right upper quadrant pain seen more with acute presentation), and normal or mild to moderate elevations liver function tests without jaundice. Encephalopathy is infrequent.
• The serum-ascites albumin gradient or gap (SAAG) in ascites has a gradient greater than 1.1.
• There is hypertrophy of the caudate lobe of the liver (separate blood supply).
• For diagnosis, one or more of the following investigations may be done. Doppler ultrasound of liver, triphasic CT abdomen, MRI with contrast, venography, and arteriography.
•
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree





