and Andrea Bischoff1
(1)
Pediatric Surgery, Colorectal Center for Children Cincinnati Children’s Hospital, Cincinnati, OH, USA
Electronic supplementary material
Supplementary material is available in the online version of this chapter at 10.1007/978-3-319-14989-9_25.
25.1 Definition and Terminology
The term idiopathic constipation refers to the incapacity or difficulty to pass stool regularly and efficiently. In addition, we believe that it also means incapacity to empty the colon.
We use the term “idiopathic” because we do not know the etiology of this condition. We are aware of many proposed explanations to understand the pathophysiology of this condition, but we firmly believe that none of those explanations have solid scientific basis. In agreement with Benjamin Disraeli, we believe that “to be conscious that you are ignorant is a great step to knowledge” [1].
We intentionally avoided other terms frequently used in the literature, basically because many of those names implied an accepted etiology. Some of those names include: “puborectalis spasm syndrome,” “descending perineum syndrome,” “chronic obstipation,” and “spastic pelvic floor syndrome.” In addition and most importantly the treatments that we have to offer to patients with constipation are not different, regardless of the category or type of constipation that the patient suffers from.
We also refer to idiopathic constipation as the central subject of this chapter because, by far, the greatest number of patients coming to our clinic with a colonic motility disorder, requesting a surgical consultation, belongs to this particular group.
25.2 Incidence, Social Impact, and Relevance
Idiopathic constipation is by far the most common defecation disorder and colonic motility disorder seen in children. It represents a common cause for surgical consultation [2–4]. It affects millions of Americans, as well as patients of other countries, but perhaps most important is the fact that it is an incapacitating condition when it is not treated properly. In fact, it produces a form of fecal incontinence known as encopresis or overflow pseudoincontinence that makes the patient socially rejected and discriminated.
25.3 Etiology
We are aware of multiple publications proposing different possible causes for this condition. However, most of those explanations have no scientific basis, and therefore we do not embrace them. We prefer to take a healthy and potentially more productive attitude by declaring our ignorance about the origin of this condition.
Some authors believe that diet is very important as an etiologic factor of constipation [5, 6]. There is no question that different types of food have either a laxative or a constipating effect on our bodies. In addition, we recognize the existence of personal idiosyncrasies that explain why one type of food may act as a laxative for one individual and have a constipating effect for another one. Although we recognize that diet is important to regulate colonic motility, we believe that the therapeutic value of diet is negligible in the most serious forms of constipation. We must keep in mind that this chapter belongs to a book of surgical treatments of colorectal problems in children. The type of constipation that is manageable by diet belongs to the pediatric clinics. Those patients do not come to our clinic because they are treated either by a pediatrician or gastroenterologist. The patients that come for surgical consultation are patients that have already received all kinds of unsuccessful medical managements previously.
There are also many articles [7–12] that try to explain the problem of idiopathic constipation on psychological basis. The psychodynamic mechanisms proposed are interesting and sometimes picturesque; including, strict demanding parents. Strict demanding parents who impose rigid rules on a child during the toilet training process, children that supposedly retain the stool to manipulate the parents to achieve their own purposes. All these mechanisms may have an element of truth, but we do not believe that they can explain the severe forms of constipation in patients with fecal pseudoincontinence, giant megacolon, sometimes megabladder, serious nutritional and developmental disturbances, and sometimes death. We think that it is certainly not easy to retain stool voluntarily in an otherwise autonomous normal rectosigmoid with normal peristalsis.
It is true that most patients suffering from idiopathic constipation also have a psychological disorder, but we do not think it is a primary one. Any human being suffering from severe constipation and soiling, ostracized and discriminated understandably, must have a very significant secondary psychological problem.
Surgeons, on the other hand, have proposed different potential mechanisms to explain this problem. For instance, a rather simplistic explanation is that there is a lack of relaxation of the “internal sphincter” also known as achalasia of the internal sphincter [13–16]. This is, obviously, a very attractive and popular idea. In other words, a simplistic logic dictates that incontinence means “lack of sphincter”; therefore, constipation most likely means “too much sphincter.” However, as discussed in the chapter of ultrashort Hirschsprung’s, we do not believe that the “achalasia of the internal sphincter” is an entity that can explain the symptoms of these patients.
Many patients suffering from idiopathic constipation are subjected to rectal manometry. Many of them have no relaxation reflex. The lack of relaxation has been described as a diagnostic of Hirschsprung’s disease, and therefore the next step is usually to take a rectal biopsy. If the rectum has no ganglion cells, the diagnosis of Hirschsprung’s disease is confirmed. On the other hand, if the rectal biopsy shows ganglion cells, the patient then receives the diagnosis of “achalasia of the internal sphincter.”
25.3.1 Ultrashort Segment Hirschsprung’s Disease
Ultrashort Hirschsprung’s disease has been defined as a condition in which a small length of the distal bowel has no ganglion cells. The specific length of this aganglionic zone has not been defined. Under normal circumstances, human beings have an area of aganglionosis above the pectinate line [43–45]. The length of this normal aganglionic zone has not been well established at different ages from premature life to the adult size. Consequently, it is very difficult to know if a biopsy that shows absent ganglion cells was taken from this normal aganglionic area of the rectum. At what point an aganglionic zone is considered normal and at what point is considered typical Hirschsprung’s? Both are unanswered questions.
Many authors believe that this is a common cause of constipation [39–42]. We believe that “ultrashort segment Hirschsprung’s disease” and the so-called internal sphincter achalasia are highly debatable conditions. From the clinical and radiologic point of view, patients who have been labeled with these conditions cannot be differentiated from those suffering from idiopathic constipation clinically or from the radiologic point of view. In other words, the three groups of patients suffer from severe constipation, they have a tendency to soil the underwear when the constipation is severe, they have a very dilated rectum, and most importantly, the three groups respond to the use of laxatives. Those authors who support the existence of these two conditions (ultrashort segment Hirschsprung’s and internal sphincter acatalasia) [13–16, 33–40] claim that they can make the diagnosis based on manometric studies [17–21] and confirmed by sophisticated histochemical techniques not always available to the clinician.
We have serious questions about the existence of these conditions for several reasons:
25.3.2 Rectal Manometry
During a regular rectal manometry study, a balloon is placed inside the lumen of the rectum, and the pressure of the anal canal is recorded. Under normal circumstances, the inflation of the balloon in the rectum elicits a response from the patient consisting in a drop of pressure in the anal canal, which the manometrists interpret as “relaxation of the internal sphincter.” The first question that comes to our mind is how do they know that the internal sphincter is the structure that is relaxing? If we think about the real anatomy of normal individuals (see Chap. 2), we find that the so-called internal sphincter has been defined as a thickening of the circular layer of smooth muscle of the most distal portion of the bowel. However, surrounding the entire rectum, there is an obvious and powerful striated skeletal muscle structure or voluntary sphincter mechanism. During very early manometric studies, some investigators used paralyzing agents in animals and even in human volunteers in order to be able to discriminate the relaxation of the striated muscle, from relaxation of the smooth muscle (internal sphincter), and they concluded that it was the smooth muscle that was relaxing. In addition, they even reached the conclusion that 85 % of the bowel control depended on the “internal anal sphincter!” Yet, during all the clinical manometric evaluations of patients, muscle relaxants are not used, and therefore, we do not know if the drop of pressure in the anal canal is due to a relaxation of the striated muscle complex or to the smooth muscle.
Another very serious question that comes to our mind when discussing rectal manometry is the fact that most patients evaluated manometrically suffer from constipation, and, by definition, most of them have a very dilated rectum. In order for the patient to have a relaxation reflex, it is necessary to stretch the rectal wall with the inflated balloon. That means that we are supposed to use different volume balloons for different patients depending on the size of the rectum. We are unaware of this kind of methodology. Most manometries use the same size balloon for all patients, and certainly we have never seen 1 or 2 L balloons, yet we have seen many patients with giant rectums. As a consequence, it is conceivable that the inflation of a relatively small balloon that does not stretch the rectum would produce a negative reflex. In other words, the pressure in the anal canal would not drop because actually the rectum was never distended due to the fact that they used a standard size balloon in a megarectum. When we asked these questions to different proponents of manometry, we do not have a reasonable answer.
25.3.3 Doubts and Questions About the Anatomy of the Internal Sphincter
The “internal sphincter” has been defined as a thickening of the circular layer of the smooth muscle of the bowel in its most distal portion, the anorectum. Yet, real photographs documenting the presence of this structure are extremely unusual to see (see Chap. 2). A description of the specific thickness and upper and lower limits of this elusive structure at different ages is inexistent. There are plenty of diagrams but very few photographs, and those photographs do not show the limits of that structure and the way to separate it from the striated sphincter mechanism. Recently, endoanal sonography illustrates a series of circular structures that are interpreted arbitrarily with an arrow as “internal sphincter.” In addition, most of those endoanal study publications do not specify how much they introduce the device and how the so-called internal sphincter looks at different depths in the anal canal and the rectum.
Our experience in the surgical exploration of the normal rectum via posterior sagittal for the repair of urethral problems or tumors did not allow us to identify a structure that looked similar to the descriptions of the so-called internal sphincter (see Chap. 2). With a posterior sagittal incision, we can identify and clean the entire posterior rectal wall all the way down to the skin and evaluate the thickness of the bowel wall. We have been unable to see a thickening of the bowel wall layer. With the use of an electrical stimulator, we can clearly differentiate what is a striated muscle from a smooth muscle, and, again, we have not seen the so-called internal sphincter. Another problem is that all anatomic structures have different sizes depending on the patient’s age, and we are unaware of a study of the characteristics and size of the anatomic structures such as the so-called internal sphincter at different ages.
25.3.4 Questions About Myectomy Technique
The treatment proposed for the treatment of ultrashort Hirschsprung’s and internal sphincter achalasia is an operation called myotomy or “myectomy,” myotomy being just dissection of the internal sphincter and myectomy a resection of part of that [22–25]. The description of this operation is rather vague; the surgeon must make an incision at the posterior aspect of the mucocutaneous junction in the anus and create a plane of dissection between the mucosa and the posterior wall of the rectum. All the tissue that remains between the mucosa and the posterior wall of the rectum is smooth muscle, and once the surgeon created those two planes, he is supposed to resect a strip of that tissue. The length of this strip has not been defined for different ages. That specimen should be oriented and should be sent to pathology. The pathologist is supposed to look for ganglion cells in a well-oriented specimen, and he is going to find absent ganglion cells in the most distal part and present ganglion cells in the proximal portion. However, again, the question is how do we know what is a normal length of aganglionosis in a human being? We are unaware of publications describing the specific technique followed by different pathologists. The study of the specimens must show that only included smooth muscle. In addition, looking at the pictures of the intraoperative operations as well as the description of the surgical technique used by different surgeons, one gets the feeling that every surgeon is doing a different technique, and they do not really know exactly what is included in the specimen that they send to pathology. Interestingly, for those who believe that the internal sphincter is the key for bowel control, it is difficult to conciliate the concept with the idea of doing an operation to cut that “important structure.”
25.3.5 Botulinum Toxin Injection
Recently, the injection of botulinum toxin is becoming popular to paralyze the “internal sphincter” and by doing that to improve the symptoms consecutive to the lack of relaxation of this structure [102–104]. A detailed, meticulous description of the injection has not been published. The injection is performed rather blindly. There are some reports on the endosonographic control of the injection, but again, the fact that we see an endosonographic image does not tell us exactly where we are injecting the toxin. The effect of this toxin, as we know, is to paralyze the muscle, but it also paralyzes the striated muscle. How do we know if we are actually injecting the voluntary sphincter mechanism rather than the internal sphincter? In addition, the effect of the injection of botulinum toxin is transient and must be repeated to continue the effect, and that is another reason why we are so skeptical about it.
As can be concluded from all this discussion, until all these questions can be answered in a satisfactory way, we will continue thinking that we need more scientific and systematic studies to clarify this rather confusing subject.
There are many publications of authors who propose the intestinal neuronal dysplasia (IND) as a potential explanation for some cases of constipation [26–31]. Again, we are rather skeptical about this. A critical, comprehensive evaluation of the literature on neuronal intestinal dysplasia was conducted by us [32]. The most obvious impression that we obtained from this review was that there is no basic agreement between pathologists about this histologic diagnosis [33]. In addition, we are not aware of the existence of topographic studies that describe the extension of this histologic disorder in different patients. For a surgeon to be able to offer a rational treatment for this condition, we need to know the extent of the affected bowel that will be resected. In theory that will cure the patient. This has never been done or has never been reported. In addition, the symptoms described in patients with neuronal intestinal dysplasia vary from patient to patient. The treatments vary from laxatives to enemas and to different types of resections, and finally, the follow-up of the patients has not been consistent. To complicate the problem even more, some patients recover spontaneously. We believe that “neuronal intestinal dysplasia” represents an interesting histologic disorder that deserves further scientific evaluation to try to establish a truthful clinicopathologic correlation, but at the present time, the concept has very little clinical application.
“Hypoganglionosis” has also been invoked as a potential explanation for patients with severe constipation [34–38]. Again, we have raised several serious questions about the existence of such entity. We do not know if the number of ganglion cells remains constant through our lifetime. Assuming that the number of ganglion cells remains the same in patients who develop constipation and megacolon, it is conceivable that in a specimen taken from the colon in a case with a giant megasigmoid the pathologist will see relatively less ganglion cells in every field and that may give him the impression of dealing with a case of hypoganglionosis. Yet, what the pathologist really sees in that case is only the result of stretching a normal ganglionic colon. We have never heard a coherent answer to this question, and therefore we believe that at the present time we have no basis to make such diagnosis. In addition, the treatment for such condition, assuming that exists, is the same that we offer for idiopathic constipation.
As we discussed in the Chap. 24 and specifically in the paragraph dedicated to “ultrashort Hirschsprung’s,” most of the patients that come to our center for consultation for severe idiopathic constipation already had manometric studies of the colon and the rectum, as well as rectal biopsies, with different inconsistent types of results. The protocol of management that we propose for all these patients is the same. We believe that there is no way clinically to differentiate those patients with idiopathic constipation and so-called ultrashort Hirschsprung’s, and we believe that the treatment should be the same.
We try to follow closely the developments related to newly described histologic disorders that may explain the problem of constipation including a deficiency of the substance P [46], abnormalities found with the use of monoclonal anti-neurofilament antibodies [47], and abnormalities in the cells of Cajal [48]; also we are recently learning more about the increased plasma level of pancreatic polypeptide and a decreased plasma level of motilin in children with encopresis [49]. All these deserve future investigation but at the present time have no clinical application.
We believe that patients with idiopathic constipation are born with a colonic hypomotility, not a well-characterized disorder, that affects mainly the rectosigmoid, but also may extend to the rest of the colon. We also strongly believe that this is a spectrum type of condition that may include patients who have very mild constipation, manageable with diet, as well as very severe cases that overlap with a condition known as “intestinal pseudo-obstruction” and may also kill patients. We also believe that the motility disorder frequently affects also the urinary tract simultaneously. We do not believe that the urinary problems seen in some of these patients are consecutive to the mechanical effect of the dilatation of the colon, but rather that these patients suffer from a similar idiopathic malfunction (hypotonic, large) of the bladder associated to the hypomotility of the rectosigmoid.
The concept of spectrum of the disease cannot be overemphasized. Most of the proposed treatments for constipation [50–55] do not take this concept into consideration. The authors rather offer standard therapeutic protocols, like if all patients suffered from the same degree of constipation. In other words, the treatments proposed are not individualized. Interestingly, the different modalities of treatment proposed in the literature [56–64] report percentages of success that varies from 50 to 80 %, but there is always a group of patients who do not respond. We believe that this is another manifestation of a spectrum type of condition. We also believe that we, pediatric surgeons, most likely will be dealing with the group of patients in whom the traditional therapeutic strategies failed.
25.4 Pathogenesis
Although we do not know the cause of idiopathic constipation, we have learned a great deal about its natural history due to the long-term follow-up of our patients. Idiopathic constipation is a self-perpetuating and self-aggravating incurable condition, incurable but manageable. We assume that the babies are born with a primary hypomotility disorder that affects mainly the rectosigmoid but may affect the entire colon. This motility disorder incapacitates the patient to empty the rectum. This produces accumulation of stool, which is responsible for the dilatation of the rectosigmoid or sometimes other portions of the colon.
We have learned that in patients that are born with atresias of different hollow viscus, reconnecting or reanastomosing an extremely dilated, chronically obstructed hollow viscus to a tiny, nonused microintestine produces poor results in terms of function which is attributed to a lack of peristalsis of the most dilated part of the bowel or hollow viscus. Therefore, the recommendation is to resect the most dilated part of the bowel or to taper it. This has been observed when dealing with the small bowel, colon, esophagus, or ureter. It seems like it is necessary for the hollow viscus to have a specific diameter in order for the peristalsis to be optimal and efficient. It seems to us that the dilatation of the rectosigmoid has the same effect, affecting the peristalsis. In other words, retention of stool produces dilatation, and dilatation produces poor peristalsis. Poor peristalsis produces more retention, and more retention produces more inefficient peristalsis, creating a vicious cycle (Fig. 25.1).
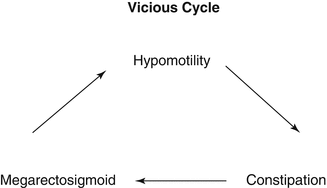

Fig. 25.1
Vicious cycle of idiopathic constipation. Poor colonic motility produces fecal retention; fecal retention produces dilatation; rectal and colonic dilatation produces poor peristalsis which continues producing more severe constipation
Eventually the passage of a large, hard piece of stool through the anus may produce a laceration (fissure), understandably producing pain during defecation. This explains the voluntary attempt of the patient to retain the stool and avoid bowel movements. In other words, the patient is born with a certain degree of rectosigmoid malfunction, but eventually, another factor is added to the equation which is the voluntary intention to hold the stool to avoid pain. This happens often in these patients, but we do not believe that it is a primary phenomenon (Fig. 25.2). We believe that the patient retains the stool because he learned that passing the stool is painful. Therefore, the treatment of fissures in patients with constipation consists in providing the parents with the necessary information, for them to understand the pathophysiology of this condition. In other words, in order for the fissure to heal, we have to guarantee that the patient does not pass a hard piece of solid stool through the anus, which could reopen the fissures contributing to the aggravation of the symptoms. Stool softeners, laxatives, and time will make the fissure heal, provided the patient does not have another episode of impaction, passing hard stool which will reopen the laceration of the anus (fissure).
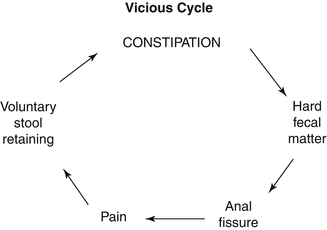

Fig. 25.2
Vicious cycle of patients with idiopathic constipation and painful bowel movements. Poor rectosigmoid motility produces stool retention. This eventually becomes fecal impaction, which is the presence of hard fecal matter in the rectum. When this finally passes through the anus, it produces a fissure. The fissure produces pain, and the pain induces the patient to try to hold the stool and avoid bowel movements, which exacerbates the stool retention
The concept of incurability of this condition is also fundamental for a successful management. Not understanding and not accepting the idea that this condition is incurable explains in part the high recurrence rates reported in the literature [56–64]. Treatments are provided frequently on a temporary basis based on the rather naive assumption that the condition is cured. Subsequently, the treatments are tapered or interrupted, assuming that the patient has been cured, only to find that the patient suffers a recurrence. This creates frustration for the patients and parents which may explain why most of these patients go from institution to institution looking for an answer. Sometimes, colostomies or enemas are performed, also on a temporary basis. Opening a proximal colostomy or applying enemas may produce a decrease in the size of the dilated viscera and give the impression that the patient has been cured. In fact, the patients actually may show symptoms of improvement after the colostomies are closed or when the enemas are discontinued. However, if the patient does not receive further treatment, symptoms most likely will come back.
Figure 25.2 shows a cycle of constipation and megarectum that we believe occurs in these patients. Many publications support the idea that the problem of constipation starts during the toilet training process [50–55]. We believe that the toilet training stage of life is rather the time when the symptoms become more evident; however, we think the patients are born with this condition. Babies who are breastfed may not show symptoms because of the well-known laxative effect of the human breast milk. However, when the breastfeeding is discontinued and the patient receives formulas and other kinds of food, the symptoms become obvious. Babies who have symptoms of constipation while receiving breast milk most likely suffer from a more severe type of constipation. Many times, the parents tell us that the problem started during the preschool years. However, when we inquire specifically about the bowel movement pattern since birth, we frequently find evidence of constipation from very early in life. Actually, the parents remember most vividly the episode of the first fecal impaction, and they may refer to that event as the initiation of symptoms. Yet, we all know that a symptomatic episode of fecal impaction represents the final step of a chain of events that started a long time before.
Many pediatricians believe that normal individuals can go 2 or 3 days without a bowel movement through life without having any significant implications. We believe that that is true for many human beings; however, in dealing with patients with idiopathic constipation, it is extremely important to expect the patient to have bowel movements every day as a manifestation of the response to our treatment. Allowing the patient to go one or several days without bowel movements would generate again the vicious cycle that we have been referring to (Figs. 25.1 and 25.2).
25.5 Natural History and Clinical Manifestations
A meticulous, detailed clinical history may show sometimes that babies did not pass meconium in the first 24 h and started having symptoms of constipation even when they were young babies and were taking breast milk. As the patient grows, the symptoms of constipation become more severe. The parents describe vividly how the patient suffered for the first time a painful bowel movement with blood in the stool. After that, the patient became a “stool retainer”; he goes to a corner of a room and hides while passing stool, trying to avoid the bowel movement. The patient refuses to sit on the toilet because he knows that what follows is a painful experience. Eventually, the patient has the first episode of fecal impaction. This is a very stressful event in the life of the patient and the parents. We refer to fecal impaction as a situation in which the patient has in the rectum a very large, solid piece of stool that has been there for days or weeks. When laxatives are prescribed to a patient who has fecal impaction, the result is exacerbation of severe, crampy abdominal pain and sometimes vomiting. This may resemble the symptomatology of colonic obstruction. For this reason, we consider it contraindicated the use of laxatives in a patient with fecal impaction. Occasionally, the laxatives produce diarrhea, and the patient keeps passing liquid stool around the impacted fecal matter (this is known as “paradoxical diarrhea”). This gives the parents the false impression that they are overusing laxative and may induce them to reduce the dosage, which of course, will exacerbate the problem.
Usually it is during the preschool or school age, when the patient starts showing a very bad prognostic sign which is soiling the underwear also known as “encopresis.” This is a phenomenon that we call overflow pseudoincontinence. Sometimes, constipated patients have 1, 2, 3, 5, or even 10 bowel movements every day, giving the parents and the doctors the false impression that the patient is not constipated. Actually, this may be a manifestation of a serious constipation problem. The patient passes a very small amount of stool, but never empties the rectum. Eventually, he/she will suffer from chronic fecal impaction. The impaction produces dilatation of the entire rectum including the anal canal. The anal canal represents the sensitive part of our bowel that allows us to know when stool is coming down to the anus and allows us to determine when to use our voluntary sphincter. However, we believe that perhaps the presence of a large mass of solid stool stretching the rectum on a chronic basis, eventually, makes the patient accustomed to the presence of that mass and then starts soiling on a chronic basis without the patient’s awareness. This is an ominous sign. This means that the condition has already advanced very significantly and will require a very aggressive management. The patient soils the underwear day and night and basically does not have spontaneous bowel movements. At this stage, the patient basically behaves like a fecally incontinent patient, with all the implications that come with this diagnosis. In other words, the patient smells bad, and the family starts fighting with him/her and rejects them. In addition, the patient becomes accustomed to his/her own smell and is not accepted at school, and as a consequence, the patients develop serious psychological sequelae which we believe again are not primary.
Eventually, the parents believe that the patient is intentionally trying to upset them by sitting at home in the living room, obviously smelling very badly and not doing anything to solve the problem. In fact, the patient does not perceive the bad odor. These ideas in the parents are supported sometimes by the explanations given by psychiatrists in the sense that they believe that the patient is trying to manipulate the family by holding the stool intentionally. The emotional interrelations in the family are severely affected, and that is when the psychological problems become worse. We do not believe that the patients do this intentionally. We believe that if an individual wants to manipulate his/her parents, he could select many other ways to do so. Nobody wants to have stool-stained underwear, to smell bad, and to be rejected by society.
The family may put a lot of emphasis on the lack of cooperation from the patient and make the patient feel guilty. By the time these patients come for surgical consultation, they are withdrawn, shy, negative, and reluctant to be examined by the surgeon. They usually have been subjected to many painful rectal examinations. They have scars from previous fissures in the anus. The family is usually in distress. These patients have also been subjected to unsuccessful therapeutic programs including biofeedback [65–67], behavior modification [68–74], and psychological and sometimes psychiatric treatments without positive results.
As we will see, a successful, efficient, adequate management of these patients will make the problem of encopresis disappear. Very occasionally, we see patients that we treat efficiently; in other words, we are sure that the patient no longer carries large amounts of stool in the rectum and yet they keep behaving like if they are incontinent. Those patients deserve a more meticulous study to rule out neurologic problems such as tethered cord, spina bifida, tumors, or a more severe psychological disorder. Fortunately, this particular situation is rare.
25.6 Diagnosis
The diagnosis of idiopathic constipation is a clinical one, supported by a radiologic evaluation. A patient that presents with the symptoms already described most likely has a problem of idiopathic constipation. Patients with Hirschsprung’s disease do not soil. In addition, when left unattended without surgical treatment, patients with Hirschsprung’s disease are at risk of dying. They frequently suffer from severe enterocolitis. The patients who survive and go undiagnosed with Hirschsprung’s disease are frequently malnourished and have a history of episodes of enterocolitis. Most patients with idiopathic constipation are well nourished. It is extremely unusual to see a clinical picture similar to enterocolitis in patients with idiopathic constipations. We have seen something similar in cases with extremely severe idiopathic constipation.
Obviously, the patient must be examined with special emphasis in the characteristics of the anus, to be sure that there is no stricture and/or anterior mislocation of the anal orifice.
A contrast enema performed with a hydrosoluble material (Fig. 25.3) is the most valuable diagnostic study to confirm the diagnosis of idiopathic constipation. The characteristic image of a contrast enema in a child with a megarectosigmoid is shown in Fig. 25.4. Most of the times the dilatation of the colon affects the rectosigmoid all the way down to the level of the levator muscle which is recognized because it coincides with the pubococcygeal line (Fig. 25.4). The lack of dilatation of the rectum below the levator mechanism (pubococcygeal line) should not be interpreted as a transition zone or non-dilated rectosigmoid. Unfortunately, we have seen many patients that suffer from idiopathic constipation; somebody misinterpreted the radiologic study and erroneously treated the patient like Hirschsprung’s disease.
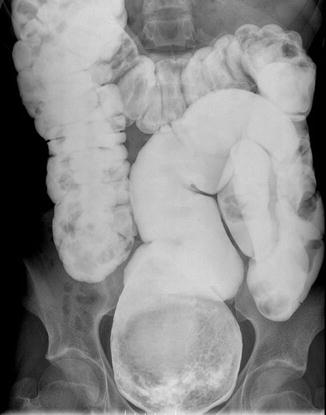
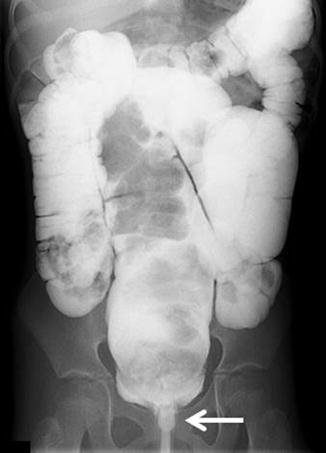

Fig. 25.3
Characteristic image of a contrast enema performed in a patient with severe idiopathic constipation. Typically the most dilated part of the colon is the rectosigmoid, and the descending and transverse colon seem to be normal in caliber

Fig. 25.4
Megarectosigmoid extending all the way down to the pubococcygeal line. Below this line, the rectum is not dilated because it is compressed by the funnel-like sphincter mechanism. Arrow shows the rectum compressed by the sphincter
In cases of idiopathic constipation, the rectum, above the anal canal, and the sigmoid are extremely dilated. This provokes an image that has been described many times in the literature as a “posterior shelf” (Fig. 25.4). This “posterior shelf” has been interpreted by some authors as evidence of an anteriorly located anus [75–78]. Many surgeons adopt this concept and treat these patients on the basis of that idea. We believe that such diagnosis has no scientific basis. We have never seen a real anteriorly located anus, defined as a normal anus, nonstrictured, with normal anal canal, surrounded by the sphincteric mechanism 360°. The contrast enema in patients with idiopathic constipation shows different degrees of dilatation of the rectosigmoid as expected in this spectrum of disease (Fig. 25.5a, b). Most interestingly, most of the times, there is a dramatic size discrepancy between a normal size transverse and descending colon and the very dilated megarectosigmoid (Fig. 25.5a). These changes are actually the reverse from what we see in Hirschsprung’s disease (Fig. 25.6). In Hirschsprung’s disease, the aganglionic segment is the most distal part of the rectosigmoid, and the dilatation is located in the proximal colon (normoganglionic).
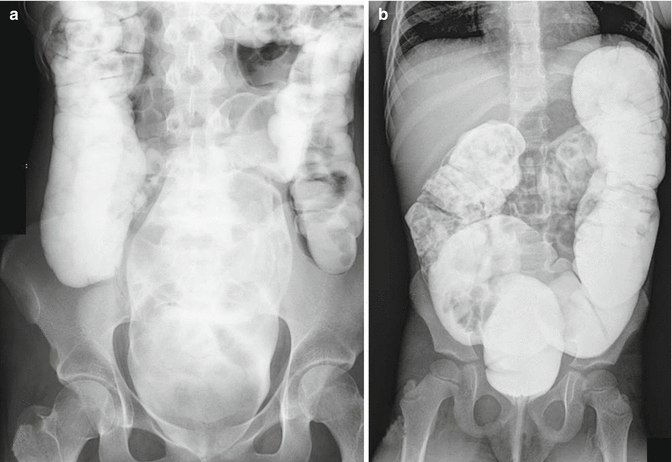


Fig. 25.5
Two different types of colonic dilatation in patients with idiopathic constipation. (a) Dilated rectosigmoid with normal caliber proximal colon. (b) Generalized colonic dilatation

Fig. 25.6
Characteristic changes of the rectosigmoid in a patient with the most common type of Hirschsprung’s disease. Arrow shows the transition zone
We learned that patients with a more localized rectosigmoid dilatation have a better prognosis and respond better to the treatment. When the patients have a dilatation of the entire colon, we consider that a bad prognostic sign (Fig. 25.5b). We formally contraindicate the use of barium in these patients. The term “barium enema” is widely used. In addition, adult radiologists like to use barium because the barium lines the mucosa of the colon and allows an accurate diagnosis of mucosal abnormalities such as diverticula, ulcers, and/or polyps. In our patients, on the other hand, we are not looking for mucosal abnormalities; we rather want to see the degree, location, and extension of the dilatation of the colon, and also in addition, we want to know how well or how bad the colon empties after it has been filled up with a contrast material. In other words, we want to see sequential imaging of the filling up of the colon and then a post-evacuation film.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree








