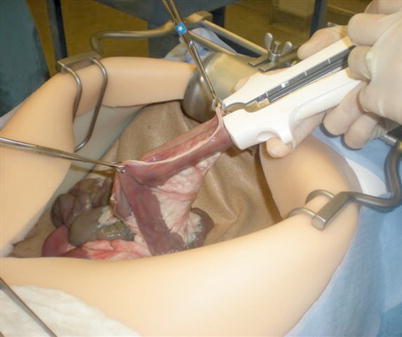
Fig. 37.1
Laparoscopic colectomy in a porcine model
Simple box trainers for laparoscopic skills such as the validated MISTELS (McGill Inanimate System for Training and Evaluation of Laparoscopic Skills) are effective at the junior trainee level and should be readily incorporated into any laboratory curricula. VR platforms have also been shown to improve performance in the operating room. More specifically, dedicated practice with VR simulators has correlated with improved operative times and efficiency of movement for clinical laparoscopic cholecystectomy [20]. Seymour et al. evaluated 16 residents of varying levels and compared clinical laparoscopic cholecystectomy outcomes between residents who received training on a VR system and those who did not. They found no difference in baseline assessments between the two groups, but found that residents who trained on the simulator were faster, made fewer errors, and were less likely to injure the gallbladder in the operating room [20]. Grantcharov et al. also evaluated 16 residents and compared training on a VR simulator to a control group. They found improved economy of movements and fewer errors in residents who were trained on a VR simulator [21]. Beyer and colleagues evaluated transfer of skills from simulators to the operating room using the Global Operative Assessment of Laparoscopic Skills (GOALS), a validated laparoscopic skills assessment model [22]. Their prospective trial involving 19 residents found improved GOAL scores in residents who were trained on a simulator when compared to those who were not.
Simbionix (Cleveland, OH) offers a VR (LAP Mentor) model for laparoscopic sigmoid colectomy that more accurately portrays resection in the operating room than previous hybrid systems [23]. Of the five types of validity, face, content, and construct have been established for general procedures with the LAP Mentor VRS [24, 25]. More recently, construct validity, i.e., the ability of the simulator to distinguish between different levels of skills, was established for certain metrics specifically with the laparoscopic sigmoid model [26]. In this study, the metrics assessing the instrument path length, the accuracy of the medial peritoneal mobilization, and the quality of the IMA dissection demonstrated the strongest ability to differentiate between general surgeons and laparoscopic colorectal surgeons. However, construct validity was not established for technical errors, as the model could not distinguish between experts and novice surgeons.
The successful application for procedure-specific training with VR systems has recently been demonstrated in two randomized trials. Grantcharov et al. developed a comprehensive ex vivo preoperative training curriculum that improved performance for LC [27]. Calatayud et al. tested “warm-up” with a VR system prior to laparoscopic cholecystectomy and found that OSATS global rating scales were better after practice [28]. The colectomy study involved preparation with simulation, cognitive training, and participation in a cadaver lab. In this study, residents were PGY-2 through 4, having previously completed FLS and possessing some advanced laparoscopic experience. Using an entire curriculum that addressed multiple aspects of performance, which included procedure-specific simulation, overall LC skills were enhanced. This impressive approach was successful; however, having all trainees perform this labor intense program prior to the procedure may not be practical. The cost and time requirements of the model are likely not likely sustainable in most training programs outside of a trial. However, this well-designed trial most importantly demonstrates that preparation can improve performance for LC. Each academic institution may choose to incorporate one of these preparation models or a variation on this theme. The VR studies for basic laparoscopic skills training have routinely incorporated a proficiency-based model, whereby trainees have proficiency targets to meet, rather than time on task as a training goal [20, 27]. For the cognitive component of procedures, different modalities have been used. For example, in an effort to simplify this “rehearsal” and hasten the learning curve for laparoscopic right colectomy, we designed an ongoing multicenter trial with an edited 15-min “voice-over” instructional video for residents to review before performing laparoscopic right colectomy. The results are unknown, but the early feedback has been encouraging.
In addition to simulation and nontraditional preparation, several very basic but underutilized modalities should be considered to improve the educational quality of each LC case for the trainee. Residents must fulfill their responsibility by coming to the operating room with a detailed knowledge of the relevant anatomy, the indications for surgery, steps of the procedure, and the potential complications. Additionally, they should possess, to a certain degree, the skills required to do a portion of the case. As faculty, we often know how to access the best video or atlas that most accurately depicts the appropriate steps of the procedure. Ideally, a curriculum-based approach will include resources for residents to access to enable them to efficiently acquire this knowledge [27]. The trainer should become familiar with the skill level of the resident and be sure they understand the degree of complexity for each case. It is also important to verify that the trainees are being informed about case coverage in advance. It is critical to be an advocate for your trainee by helping them identify the appropriate resources that may help them prepare. Lastly, and most importantly, preoperative communication must improve. In the SIU B.I.D. model, the briefing is a short interaction at the scrub sink [19]. The purpose of this interaction is to both assess the needs of the learner and to establish learning objectives for both learner and teacher for that particular case. This conversation forces a review of past experiences and helps formulate needs and deficits. Furthermore, learners automatically integrate the experience making it more retrievable at a later date. Unfortunately it seems that this interaction seldom occurs. In a recent survey of nearly 5,000 residents, only 18 % felt that the educational goals of the case or details of the procedure are discussed preoperatively [29]. Adoption of this simple yet effective communication strategy, outlined above, may have a dramatic impact on your current trainees.
Intraoperative Training
Preoperative preparation and postoperative assessment for laparoscopic colectomy may be underutilized, but they are both definable and have been evaluated. General intraoperative teaching methods and procedure specific approaches are nebulous. More specifically, each LC entails numerous variables that can hinder consistent and effective training. Three of these variables routinely inhibit a trainee’s ability to master laparoscopic colorectal resection, and two are specific to laparoscopy. First, several attending surgeons are not comfortable with their own ability to perform LC. Second, the window between the correct and inaccurate dissection plane is similar to open surgery, but the trainer’s ability to control precision and prevent potential problems is slightly compromised with laparoscopy. These two variables are prevalent in academic surgery, but will likely wane in time as the generation of minimally invasive surgeons continues to progress. Lastly, several faculty surgeons frankly have no interest in teaching residents the basics or details of laparoscopic colorectal resection. Unfortunately, the reasons or excuses for this are plentiful and were outlined above (individual, systemic, time constraints, error avoidance, report cards, etc.).
Several conventional and previously studied methods of training residents in the operating room have been described but are less effective for LC. Scaffolding involves conscious or unconscious individualized support during surgery relative to a trainee’s abilities [30–32]. This style was historically effective, yet the reduction of case volume amongst trainees and lack of consistent faculty-trainee interaction have diminished its role. The Halstedian apprenticeship model also relies significantly on experience acquired in the operating room with graduated responsibility for trainees as they progress. The majority of trainers accomplished in LC learned with these methods, but have failed to recognize that the new landscape of residency likely requires more focused educational opportunities to achieve the same result.
A significant amount of the communication during LC is ineffective. As first assistants, trainers have lost the ability to direct with an instrument or their finger and therefore depend on verbal and nonverbal cues. Roberts et al. provided in an in-depth theoretical analysis of communication in the operating room in an effort to highlight teachable moments [33]. They thoughtfully categorize four types of interaction in the operating room (Table 37.1) [33]. Instrumental interactions are the most common form of interaction in the operating room. The goal of the faculty surgeon with these interactions is simply to perform the case as efficiently and safely as possible, with little attention to teaching. All surgeons desire safe and efficient outcomes for their patients; however, to also incorporate teaching surgeons must replace instrumental only interactions with instrumental/teaching communication, when appropriate. This goal is achievable when an appropriate understanding of mutual expectations and familiarity is established before the procedure. This discussion should also include an explanation by the attending regarding their method of instruction on the two-dimensional monitor that both are viewing. This will decrease banter and noneffective interactions.
Table 37.1
Concepts of intraoperative surgeon-resident interaction outlined by Roberts and colleagues
Intraoperative communication category | Description |
|---|---|
Instrumental | Goal of interaction is to move the case forward Termed instrumental because the surgeon often uses the learner like an instrument, as a means to an end |
Pure teaching | Intended primarily to benefit the learner through providing educational value |
Instrumental and teaching | Intended to achieve the pragmatic goal of moving the case forward while also conferring teaching |
Banter | Conversation unrelated to the procedure |
In addition to improving communication both preoperatively and during the case, surgical educators agree that deliberate practice is critical to master a technical skill. Ericcson explains deliberate practice as identifying an area of performance that is to be improved and then providing immediate detailed feedback during performance [34]. This approach is most useful for LC cases when the procedure is deconstructed into steps. Having the trainee master the dissection of the inferior mesenteric artery prior to attempting the pelvic dissection is an example of this. However, the operating room with the inherent variability in disease and patient anatomy, as well as other constraints, may diminish the ability of residents to engage in deliberate practice. Thus, mastery of skills that have ex vivo models available for practice should be transferred to a skills laboratory, reserving operating room learning for fine-tuning of performance.
Guidance and/or supervision in the operating room is critical to learning LC skills; however, it may be suboptimal. A national survey of 125 surgical residency programs addressed resident satisfaction with teaching and showed that 40 % of residents sometimes felt “over-supervised” in the operating room and 21 % always felt “over-supervised,” both contributing to decreased satisfaction [35]. Optimally, the supervising faculty reduces the amount of guidance as trainees ascend along the learning curve and demonstrate improved skills, safety, and confidence. The amount of supervision in the operating room is largely influenced by the complexity of the case, resident experience, attending skill, and desire to teach. This variability will always exist, but the group at Southern Illinois University (SIU) attempted to analyze and investigate operative supervision [36]. To accomplish their goal they used an operative performance rating system and blinded external experts to rate the amount of guidance for videotaped procedures [36]. As expected, the researchers found variability amongst the supervising surgeons and witnessed a reduction in guidance with upper level residents. Furthermore, they discovered that the faculty surgeon typically underestimates the amount of supervision that they provide [36]. This finding requires further exploration and dramatically influences to the ability of faculty to objectively assess a resident’s operative performance and ability to ultimately perform the operation independently. This problem is likely enhanced during performance of LC. An experienced faculty member can practically operate with a trainee’s hands and tactfully expose the correct plane of dissection. These nonverbal clues are further assisted when the trainer holds the camera and subconsciously orients the line of dissection in the center of the monitor. Ideally, as the trainee becomes more accomplished, a second learning curve develops. This second tier of difficulty is readily exposed when the trainer is replaced with a junior resident. The junior resident is capable of holding the camera and another instrument, but all of the nonverbal guidance and direction are absent. Therefore, as we prepare our trainees to operate independently, we must find a balance between maintaining patient safety and fostering independence. This in essence is the art of surgical education.
Assessment
The structured stepwise approach to LC and ability to video record cases make this an ideal procedure for objective assessment. Prior to the development of validated scoring tools, studies evaluating the performance of trainees in the operating room for LC lacked detail about the complexity of the case, the role of the trainee, and appropriate end points. Conversion rates and operative times were used to assess performance, yet they are likely more reflective of the attending surgeon, not the resident.
After the OSATS (objective structured assessment of technical skill) was developed and validated [37], numerous applications and variations of this tool were introduced for almost every subspecialty (Fig. 37.2). We have now been inundated with validated scoring systems containing both generic and procedure specific metrics, with several measures developed specifically for LC. Unfortunately, it has been demonstrated that substantial time often elapses between performance in the operating room and the completion of an evaluation tool [38]. Ideally, the faculty should complete a technical evaluation at the end of every case, or at least within 24 h. As faculty, we must become familiar with the validated specialty-specific tools for LC that are available for the assessment of trainees. Utilization of a validated assessment tool not only stimulates a post-procedure conversation but also ultimately involves procedure-specific feedback as well areas for improvement and practice.