Fig. 20.1
Grade 3 hemorrhoids with attenuated RV septum (Courtesy of Richard Billingham, MD)
Table 20.1
Internal hemorrhoidal disease grading (classification)
Grade | Physical/anoscopic findings |
|---|---|
I | No prolapse |
II | Prolapse with spontaneous reduction |
III | Prolapse requiring manual reduction |
IV | Irreducible |
Furthermore, you must always have a high index of suspicion for other competing etiologies of recurrent rectal bleeding such as other anorectal pathology, colorectal cancer, inflammatory bowel disease, COPD, or portal hypertension, mostly based on history, other symptoms, and family history (Fig. 20.2). Just because you see hemorrhoids on examination does not mean they are the underlying cause for your patient’s symptoms.
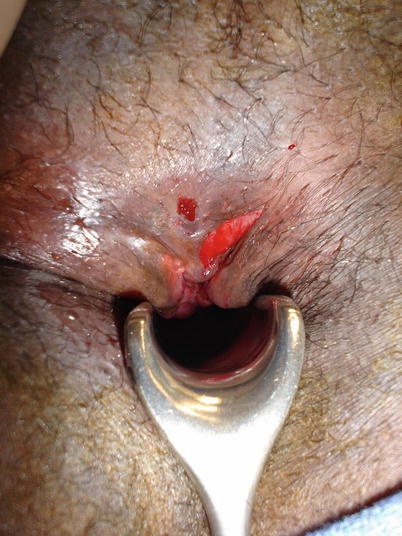

Fig. 20.2
Atypical anal fissure in a patient with concomitant hemorrhoids (Courtesy of Philip Y. Pearson, MD)
Dietary and Bowel Habits
Key Concept: Every patient can benefit from supplemental fiber and education on proper bowel habits.
Focused history should quantify and qualify the patient’s typical dietary and bowel habits. Almost all patients will initially state their diet is high in fiber. Yet, you should specifically determine whether or not a high-fiber diet (12 servings per day) or supplement is used and the frequency of stooling and the quality of stool using a standardize instrument (Bristol stool chart, Table 20.2; see also Fig. 13.1) [4]. This allows assessment of the size and shape (nuggets vs. large) as well as quality (soft vs. hard vs. watery diarrhea). It is also something you can characterize and follow over time to see their response to therapy. Hemorrhoid disease patients will often report habits, which include straining in order to affect a bowel movement, and often they will spend an inordinate amount of time on the commode. Reading on the commode while stooling is to be avoided. Likewise patients with diarrheal stools can have rectal bleeding that may be related to the frequency of wiping or competing etiology. It is important to exclude those causes. Another tool we find useful for assessing patients with constipation is the Rome-III criteria for functional constipation (Table 20.3) [5]. This is a helpful adjunct to classify the constipation, the usual root of the hemorrhoidal disease, as functional (slow transit or related to pelvic floor dysfunction) as opposed to irritable bowel syndrome type C.
Type | Description |
|---|---|
1 | Nutlike nuggets, hard to pass |
2 | Tubular and lumpy, hard to pass |
3 | Tubular with cracks on surface |
4 | Tubular, soft, and smooth |
5 | Soft blobs with clear cut edges |
6 | Mushy, fluffy, ragged edge stool |
7 | Completely watery stool |
Table 20.3
Rome-III criteria for functional constipation*
1 | Must include two or more of the following: |
– Straining during at least 25 % of defecations | |
– Lumpy or hard stools in at least 25 % of defecations | |
– Sensation of incomplete evacuation for at least 25 % of defecations | |
– Sensation of anorectal obstruction/blockage for at least 25 % of defecations | |
– Manual maneuvers to facilitate at least 25 % of defecations (e.g., digital evacuation, support of the pelvic floor) | |
– Fewer than three defecations per week | |
2 | Loose stools are rarely present without the use of laxatives |
3 | Insufficient criteria for irritable bowel syndrome |
Fecal continence (or lack thereof) also has a major impact on the development of and treatment recommendations for patients with symptoms attributable to hemorrhoidal disease. If intervention is required, an elderly female with frequent incontinence to gas, liquid, and occasionally solids may be better served by serial rubber band ligation, or hemorrhoidectomy, as opposed to hemorrhoidopexy, as cases of worsening continence after passage of the transanal stapling device has been observed.
Colonoscopy
Key Concept: Colonoscopy is not for diagnosing hemorrhoids but should be performed in at-risk patients, concerning findings, and those without resolution of their symptoms.
The role of colonoscopy has a definite place in the targeted evaluation and follow-up of rectal bleeding initially ascribed to hemorrhoids [6, 7]. Consider the case of an adopted 30-year-old man with a 2-year history of rectal bleeding. Most physicians would initially attempt a trial of fiber management and anoscopic rubber band ligation if you suspected internal hemorrhoids as the source. However, given the lack of family history, it is still crucially important that he have defined follow-up for the bleeding, as many colorectal surgeons have seen young patients with rectal bleeding, ascribed to as hemorrhoidal by the other providers, who then present much later with a locally advanced colorectal cancer after the bleeding never really resolves.
This is not to say that colonoscopy for rectal bleeding is the first diagnostic test, only that it must nonetheless be reserved for appropriate circumstances. Clearly all colorectal surgeons bear a shared responsibility for assessing adherence to national standard of care guidelines and at a minimum inquiring if their patients are up-to-date with screening colonoscopy [8].
Antiplatelet Agents and Anticoagulants
Key Concept: A number of both OTC and prescription medications can not only increase the risk of bleeding but also need to be addressed prior to intervention.
Hemorrhoidal disease is commonly seen in patients older than 50 years of age, the typical age of onset of symptomatic coronary artery disease and/or peripheral vascular disease. Given the side array of antiplatelet agents and anticoagulants (Table 20.4), colorectal surgeons must review their patient’s medication lists and be familiar with these medications. As newer, more effective agents are added to the market, surgeons must also continuously be aware of the potential of bleeding events when operating on patients actively taking them, as well as the risk of thromboembolic events if they are held. A widely held tenet in medicine is that thromboembolic disease is more difficult to treat and more lethal than bleeding, which can generally be managed nonoperatively with transfusions in all but the most extreme circumstances.
Table 20.4
Side effects of common antiplatelet and anticoagulants
Medication | Selected side effects |
|---|---|
Aspirin | Bronchospasm, allergy, PUD |
Clopidogrel | Cytopenia (rare); TTP, PUD, angina, hypertension, headache |
Prasugrel | Hypertension, TTP, cough, rash, nausea, headache |
Dipyridamole | Cardiac ischemia/angina; nausea, vomiting, headache; least risk of bleeding |
Glycoprotein IIb/IIIa antagonists | Thrombocytopenia; highest risk of bleeding |
Coumadin | Several medication interactions |
One widely used medication is clopidogrel (Plavix TM), a potent antiplatelet agent that currently is without known antidote other than time and platelet transfusion. This medication, in conjunction with aspirin, is routinely given for 1 year after percutaneous vascular stenting in order to reduce thromboembolic events prior to endothelialization. It is recommended that the decision to hold this medication be made by the colorectal surgeon in conjunction with their cardiology colleagues, and studies suggest that for most patients after 5 days of cessation of therapy, surgery can be undertaken without increased risks [9].
“Every pain in the bottom is not a hemorrhoid” – How to deal with patients and referring providers when this is not hemorrhoids and they are convinced it is
Key Concept: You should take this opportunity to educate your referring physicians and patients, not chide them.
This is one of the most frustrating and most commonly encountered scenarios. As stated, as much as 50 % of symptoms such as rectal pain, bleeding, and prolapse are inappropriately attributed to hemorrhoids by the primary care physician, endoscopist, or the patient themselves. Therefore, part of the scope of practice is not to educate just the patients but the referring providers as well. It is also a bit of a balancing act between providing proper education and avoiding accusations or arguments. One thing we have found successful, even prior to an in-office enema administration or anorectal examination, is counseling patients that they should have an open mind as to what we will find. We often tell them about the 50 % statistic and ask them to keep in mind this may be the first time they are seeing a subspecialist. They should be aware that anorectal problems are commonly mistaken for each other, and they may be diagnosed with some competing etiology such as fissures, fistulas, infections, poor hygiene, or in a minority malignancy. Furthermore, we let them know that they may have hemorrhoids, but the symptoms are coming from something else. Most commonly, a simple question even without exam as to the quality of the pain (sharp as opposed to dull) gives a clue that one is dealing with a fissure as opposed to hemorrhoids (or infrequently both). Often patients have suffered for so long with “hemorrhoids” that they are quite relieved to not only finally have the proper diagnosis but also leave with what hopefully is an effective treatment plan. If they truly are convinced it to be a hemorrhoidal problem, you should consider a referral to another colorectal surgeon for a second opinion.
Similar to patient misperceptions, the flexible endoscopic appearance of anorectal pathology can be quite different than on anoscopic exam, and primary care providers (and even gastroenterology) who do not perform a high volume of anoscopy may be obviously trying to help but limited in their depth and breadth of anorectal experience. You must be careful not to offend the referring providers and ideally point out how common misperceptions of anorectal pathology occur in the copy of the note or letter that is sent back to the referring physician. Family Medicine and/or Gastroenterology Grand Rounds along with other educational venues are an ideal way to increase local provider awareness of common anorectal pathology. Certainly arming our colleagues with knowledge of optimal lifestyle modification is a crucial first step.
Lifestyle Modification
Key Concept: Fiber does really work, if your patients take adequate amounts on a regular basis.
In the United States, governmental and medical society recommendations suggest that Americans should ingest at least 25 g of dietary fiber (12 servings of fruits and/or vegetables per day). Many patients find the goal of 25 g of dietary fiber per day a difficult goal to obtain. Yet, it is also the basis for recommendations, based on level 1 data, for the use of supplemental soluble fiber to allow a soft, bulky stool, which minimizes hemorrhoidal tissue trauma. In a meta-analysis of seven randomized trials, Alonso-Coello et al. showed that fiber results in an approximate 50 % decrease in symptoms [10]. Most, if not all, patients should try lifestyle modification before any more invasive intervention. Table 20.5 lists examples of lifestyle modification.
Table 20.5
Lifestyle modifications for patients with hemorrhoidal disease
Lifestyle modification | |
|---|---|
Diet | High-fiber booklet |
Soluble fiber supplement (bulking agent) | One heaping tablespoon in 8 oz of water once or twice daily with the goal of producing soft, bulky stool on a daily basis (ideally). Can reduce amount of water to 4 oz if loose stool |
Fluids | 2 l fluid intake by mouth per day |
Straining | Avoid straining on the commode |
Commode | Avoid reading on the commode or spending excessive time on the commode |
Perianal hygiene | Avoid excessive cleansing; use a peri-bottle, sports bottle, sitz bath, detachable showerhead, or bidet. Apply zinc oxide or other diaper ointment before each bowel movement to protect perianal skin |
Nothing per rectum | Avoid suppositories, digital dis-impaction, or any other transanal instrumentation or intervention |
Kegel exercises | Age appropriate for borderline continence or incontinence |
Pelvic floor retraining | If concomitant pelvic floor dysfunction |
Surgical Decision-Making: How to Decide on What Surgery to Do (Open, Closed, Energy, PPH, THD)
Key Concept: A number of surgical options exist for hemorrhoidectomy. Understand the risks and benefits with each one, and use them as appropriate in indicated patients.
In 1992, Bleday et al. reviewed the University of Minnesota experience with hemorrhoidal disease [11]. Of an initial 21,000 patients, 45 % were offered conservative therapy, 45 % rubber band ligation, and 9.3 % underwent operation. Certainly this experience suggests only 10 % of patients require more than lifestyle modification and/or rubber band ligation. If the surgeon and patient decide that more than conservative measures are warranted, many factors may influence the choice of intervention (Table 20.6). Clearly one size does not fit all, and treatment needs to be tailored and individualized for each patient based on the estimation of benefit and risk of the various surgical options and surgeon comfort and experience with chosen technique being crucial.
Table 20.6
Surgeon- and patient-related factors that influence the choice of operative intervention for hemorrhoidal disease refractory to conservative treatment
Surgeon-related | Patient-related |
|---|---|
Prior education and training | Age, gender, medications |
Operative experience | Bowel and sphincter function |
Local resources | Patient travel resources |
Product availability | Patient work and family preferences |
Confidence of diagnosis of isolated hemorrhoidal disease (i.e., concurrent pelvic floor dysfunction, fecal incontinence, IBD) | Red flag comorbidities: portal hypertension, Crohn, pregnancy, hx pelvic radiotherapy/radiation proctitis, immunosuppression/immunocompromised, bleeding diatheses, poor functional status, limited life expectancy, others |
Magnitude of hemorrhoidal disease burden (i.e., how big are they?) | Magnitude of the hemorrhoidal disease on the patient’s daily quality of life (i.e., how bad is it?) |
In general, grade II hemorrhoidal disease is treated with lifestyle modification and then banding, while the gold standard operation for grade III hemorrhoidal disease is the closed modification of the classic open Milligan-Morgan excisional hemorrhoidectomy (i.e., closed Ferguson excisional hemorrhoidectomy), due to its lowest recurrence rate. However, patients must be willing to sacrifice a significant amount of days off work (average of 2 weeks), and pain and discomfort may take 6 weeks or longer to subside with an excision. A common modification of this operation is the use of a Harmonic Scalpel® (Ethicon, Cincinnati, OH) or LigaSure™ device (Covidien, Mansfield, MA), even for grade IV disease [12, 13]. In general these adjuncts, despite their increased costs, decrease operative time and may result in less pain, fewer complications (less bleeding and urinary retention), and better patient satisfaction [12–16]. Initial concerns that the LigaSure may result in anal stenosis are likely due to lack of experience with the technique [17–19] and in experienced hands lead to equivalent outcomes as conventional hemorrhoidectomy. Although a meta-analysis of nine randomized trials from 2007 suggested that although use of the LigaSure hemorrhoidectomy reduced operative time and blood loss, it may not decrease pain or result in faster time to return to work [20]. Subsequently the Cochrane Collaboration meta-analysis from 2009 of 12 randomized studies on this topic suggested that given apparent equivalent outcomes with decreased pain and earlier return to work (4.8 days earlier), LigaSure hemorrhoidectomy appears superior to conventional excisional hemorrhoidectomy [21].
Compared with excisional hemorrhoidectomy, stapled hemorrhoidopexy is a relatively new, minimally invasive, technologically driven procedure. Despite it being a young procedure (approximately 10 years old), extensive level I data exists with which to guide optimal patient selection and educate expected outcomes [22, 23]. Due to its increased recurrence rate, the procedure for prolapse and hemorrhoids (PPH) should be used selectively as an alternative to conventional or bipolar excisional hemorrhoidectomy in patients with circumferential grade III hemorrhoidal disease without an especially large external component. Well-over a dozen randomized trials exist which usually show, similar to laparoscopic (minimally invasive surgery), that the PPH has a shorter operative time, less postoperative pain, and faster return to work compared to excisional hemorrhoidectomy [22]. In essence the device is a circular end-to-end anastomotic (EEA) stapler up-sized for the anorectal canal and specifically designed and intended for endoluminal supra-hemorrhoidal tissue mucosal resection (not full-thickness resection!). Thus, it results in pexying the prolapsing hemorrhoids higher in the anorectal canal (“face-lift for the anus” similar conceptually to serial rubber band ligation done all at once). The resultant mucosal resection should have very few if any muscle fibers in it and ideally should be symmetric and not be eccentric or “waisted.” Median operative times should be around 30 min for those over the learning curve. Despite short operative times and less postoperative pain, widespread adoption has been limited over surgeon concern regarding (a) the different, potentially more serious complications and (b) lack of long-term data. The most recent meta-analysis on the topic showed that the PPH procedure has a higher recurrence rate, with need for more re-interventions, compared with excisional hemorrhoidectomy [24]. Thus, it would appear patients and surgeons must weigh the short-term gains vs. the long-term potential for recurrence.
A number of randomized trials have compared LigaSure hemorrhoidectomy to stapled hemorrhoidopexy [25, 26]. Arsiani recently randomized 98 patients and found that the stapled procedure had non-statistically significantly higher complication rate (24 % vs. 14 %) and recurrence rate (11 % vs. 2 %). These results are nearly identical to those of Sakr et al. who randomized 68 patients and found complications in 24 % vs. 6 % and residual prolapse in 12 % vs. 3 %.
Transanal Hemorrhoidal Dearterialization (THD)
Key Concept: THD appears to be effective for grade II and III hemorrhoids but has (at present) a niche role in the treatment of hemorrhoids.
The newest minimally invasive, alternative treatment option for hemorrhoidal disease for patients who defer or have contraindication to excisional hemorrhoidectomy is transanal hemorrhoidal dearterialization (THD) also known as Doppler-guided hemorrhoidal artery ligation (HAL). Giordano et al. performed a systematic review of the procedure which reviewed 17 studies and almost 2,000 patients [27]. Although its place in the hemorrhoidal disease treatment algorithm remains uncertain, it appears to be an efficacious, minimally invasive option for grade II and grade III disease. As an outpatient procedure, operative times were typically less than 1 h, with most patients returning to work within a few days and only 18 % of patients experiencing pain. Acute hemorrhage was rare—seen in only three patients. Despite these excellent short-term outcomes, at 1-year symptom recurrence was relatively common—11 % for prolapse, 10 % for bleeding, and 9 % for painful defecation. Subsequently in a review of 170 patients, Ratto et al. reported bleeding in 1.2 %, confirmed residual prolapse in 10 %, and recurrent disease requiring operative intervention in 4 % [28]. In this at 1 year, bleeding and prolapse were controlled in 94 and 90 %, respectively. Clearly results are superior in grade II or II disease compared to grade IV disease, in which this therapy is likely a suboptimal choice [27, 28]. Given the paucity of high-quality data, this procedure will not be discussed in the remainder of this chapter.
Hemorrhoidal Crisis: What Do You Decide to Do at the Time?
Key Concept: When presented with this situation, it is not the time to be overly aggressive surgically. Stick to your basic principles of preserving anoderm, relieve the inflammation and clot, and do not damage the underlying sphincter.
Hemorrhoidal crisis, defined as acutely incarcerated or strangulated internal hemorrhoids with a component of secondary external thrombosis, requires expedient expert care (Figs. 20.3 and 20.4). These patients usually have a past history of constipation and prolapse and present with severe anorectal pain as well as urinary retention. In the past, patients were treated conservatively with analgesics, ice packs, and sitz baths given the major impendent to surgical intervention of distorted anatomy from both the underlying clot burden as well as the marked edema. However, true risk to patients, especially if diabetic, exists with nonoperative approach given necrotic tissue.
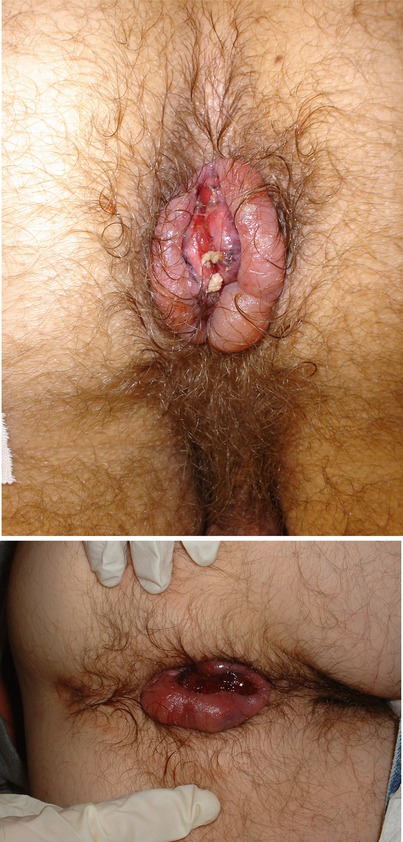

Figs. 20.3 and 20.4
Hemorrhoidal crisis (Courtesy of Richard Billingham, MD and Philip Y. Pearson, MD)
In order to expedite resolution of suffering, colorectal surgeons facile with excisional hemorrhoidectomy can and should intervene selectively in single or multiple quadrants as the distorted anatomy and comfort of the surgeon allows excising necrotic tissue, expressing thrombosis, and reducing prolapse. Optimal intervention includes either closed or, in the presence of significant necrotic tissue, open excisional hemorrhoidectomy (Fig. 20.5). In general, the authors would avoid stapled hemorrhoidopexy in these circumstances for fear of the large 33-mm stapler or large dilator causing inadvertent sphincter damage. In addition, a large part of the symptoms from this situation is from the external component—something that the stapled pexy does not address.
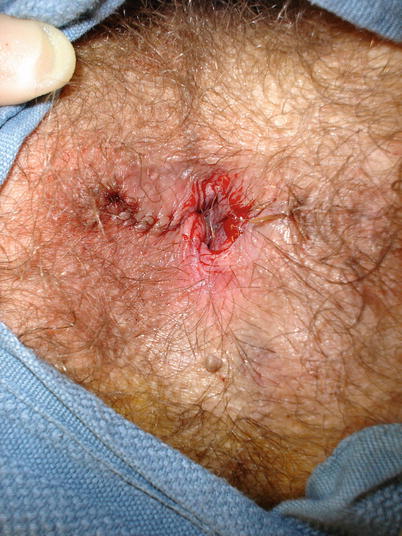

Fig. 20.5
Wounds following excision for hemorrhoidal crisis. This patient is the same as Fig. 20.2 for comparison (Courtesy of Philip Y. Pearson, MD)
In 1982, C. Wang from Taiwan reported on his experience with urgent closed hemorrhoidectomy in 56 patients [29]. The reported technique specifically used packing to push the mucosal flaps against the anorectal wall and to reduce hemorrhage, and he reported excellent outcomes. More recently a randomized trial of a potentially less morbid alternative of incising the mucosa overlying the clots (similar to as for external hemorrhoids) with rubber band ligation was shown to be safe and effective [30].
In our experience, the choice of what to offer the patient depends highly on the surgeon assessment of the degree of anatomic distortion and presence or absence of gangrenous changes—the latter a clear indication for excision. Also, if a less invasive approach is undertaken, without adequate assessment of gangrene or suboptimal results, a contingency plan for expeditious treatment must be in place if the patient decompensates (i.e., rural or unreliable patients may need to be admitted for observation).
Postoperative Regimen
Bowel Management and Avoiding Constipation
Key Concept: Ensure your patient is on a proper bowel regimen postoperatively or obstipation (or extreme pain with hard bowel movements days later) will ensue.
After elective hemorrhoidectomy, in addition to taking fiber and increased fluids, it is important for patients to preemptively treat and avoid narcotic-induced constipation. We recommend fiber twice daily, stool softener three times daily, and if no bowel movement within 48 h, then 60 cc of milk of magnesia every 12 h until a movement is achieved. An alternative regimen would be fiber in the morning and MiraLax (17 g in a tall glass of water) in the evening.
Pain Control with Narcotics, NSAIDS
Key Concept: Non-narcotics aid in reducing not only the pain but also decreasing the need and side effects from narcotics.
Optimal analgesia is achieved using a combination of nonnarcotics and narcotics including, for example, maximum dose Tylenol (recently reduced from 4 to 3 g per 24 h by the FDA due to concerns over hepatic toxicity) 750 mg by mouth every 6 h, alternating every 3 h with 600 mg of ibuprofen with food every 6 h. Opioid-naïve patients are then typically prescribed oxycodone 5–10 mg every hour as needed for breakthrough pain, with titration as needed. The amount of postoperative opioids may be reduced by the intraoperative use of ketorolac, as well as other newer adjuncts as described below [31].
Sitz Baths: Do They Work?
Key Concept: Despite lack of evidence, sitz baths are widely used and have little downside.
Used since ancient times, little level I data exist for the effect of warm sitz (from the German word “sit”) baths on hemorrhoidal pain, but several studies have documented that warm water sitz baths do indeed result in a decrease in anorectal canal pressure for both fissure and hemorrhoid patients [32, 33].
Patients are counseled that soaking the buttocks and anus in warm water for 15 min four times a day is generally recommended and is thought to (1) aid in keeping the area clean, (2) increase perfusion to aid healing (3) reduce anorectal canal resting pressure, and (4) be soothing for most but not all patients. In our experience, sitz baths are effective for the stated reasons, and patients should be counseled that they are an important component of their optimal postoperative outcome and one which they need to take responsibility for.
Preoperative Counseling and Postoperative Instructions
Key Concept: Managing patients’ expectations ahead of time and having preprinted instructions for the postoperative period that addresses many of the commonly encountered scenarios and questions go a long way in making this easier on your patient (and you).
Banding
As part of the informed consent process, patients should be counseled re: the likelihood of needing additional banding every 4–6 weeks until the problem is cured or the patient and the surgeon decide to try a different therapy. In addition, we cover the possibility of vasovagal reaction (relatively common) that they may experience some additional bleeding after the band falls off in 5–7 days, discomfort with the feeling that something is stuck in their rectum for approximately 24 h, feel the urge to defecate, and that rarely the rubber band application of the rubber band may result in perianal sepsis and risk of colostomy or death. Patients are counseled if they have fever or urinary retention to proceed to the emergency room for evaluation. Table 20.7 shows a sample of banding patient instructions.
Table 20.7
Post-hemorrhoidal banding patient instructions
Self-care after banding | |
|---|---|
Discomfort in rectum | Sitz baths, Tylenol, ibuprofen |
Constipation prevention | 1st-line fiber, 2nd-line milk of magnesia |
Bleeding | Minor bleeding expected |
Infection | Rare; if delayed urinary retention or fever >101.3 °F (38.5 °C), then consider proceeding to the emergency department |
Passing the band | Expect to not necessarily see the band(s) pass in the stool |
Recurrent symptoms | Return to clinic no sooner than 6 weeks for consideration of additional banding |
Stapled Hemorrhoidopexy
Patients should be counseled that the first part of the operation is an exam under anesthesia, and sometimes those findings will steer us away from the stapled procedure; you and patient should, ahead of time, discuss the possibility that the EUA may change the operative plan, and the surgeon may recommend just banding at the time of EUA or excisional hemorrhoidectomy. Although stapled hemorrhoidopexy results in less discomfort relative to excisional procedure, patients may still experience significant discomfort that may last as long as 2 weeks (or permanently in the setting of complications) and should be given appropriate analgesics (i.e., narcotics) and bowel regimen. Also, most of the complications of stapled hemorrhoidopexy (see below) should be discussed with the patient, including chronic or permanent alterations in bowel habits and permanent pain and need for additional surgery. In general the recommendations from Table 20.7 apply, with the exception that patients may see staples as opposed to bands.
Excisional Hemorrhoidectomy
This procedure is notoriously painful, and patient should expect pain and discomfort for the better part of 6 weeks. Patients need to be committed to doing sitz baths and preventing constipation that can be anticipated due to the narcotics and also fear of painful defecation (fiber twice daily, Colace 100 mg orally three times daily at a minimum, increased fluid >2 l per day). If the patient does not have a bowel movement within 48 h of surgery despite the above regimen, then we recommend starting 60 cc of milk of magnesia every 12 h until a bowel movement is achieved. Use of ice packs (frozen peas which mold to the area as they soften) may also be used to treat discomfort and swelling. Patients also need to understand that after approximately 24–48 h, the wounds are likely to open up and significant swelling may occur. It is also a good idea to let your patient know they may have open wounds for weeks that will eventually heal in but may be left with small tags that can always be removed in the office.
Complications of Hemorrhoidectomy: What Are They, How Often Do They Occur, and How to Approach and Manage Them?
Key Concept: Hemorrhoidectomy typically goes very well, but it is not a benign operation. You need to be aware of not only how to avoid complications but also how to manage them.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree








