Fig. 10.1
(a) Water-perfusion catheter (Medical Measurement Systems). (b) High-resolution catheter (Medical Measurement Systems). (c) Three-dimensional high-resolution catheter (Sierra Scientific Instruments) (Courtesy of Medical Measurement Systems)
The water-perfusion catheter consists of a flexible thin (diameter between 3.5 and 7.0 mm), plastic tube with four to eight side holes circumferentially or spirally arranged and a central catheter for balloon inflation. The catheter is connected to a perfusion apparatus with a pneumohydraulic pump set to pressures of 10–15 psi with water slowly perfused through the side holes at a rate of 0.1–0.5 mL/min/channel.
In 2007, with advances in technology, a high-resolution, solid-state manometric system was developed that has channels at 0.5–1.0 cm intervals. Each has multiple sensing points which together allow for retrieval of many (usually 36) data points producing a topographical plot of intraluminal pressure. This large amount of data retrieval provides a clearer visualization of the area and prevents loss of potentially important information. The results of the high-resolution catheter correlate well with the water-perfusion studies. Most recently, a 3D high-definition catheter was developed, producing even more accurate and detailed data retrieval. It is 10 cm in length and consists of 256 solid-state microtransducers placed circumferentially 3 mm apart. Due to the placement of these sensors, the results can be interpreted in a multidimensional fashion.
Since the creation of these systems, there has been much interest questioning if the newer modalities of anorectal manometry present added benefit over the older systems. When comparing the various catheter systems, the water-perfusion system has advantages in that it remains a low-cost option with ease of interpretation but can be difficult to calibrate and significant time is needed for maintenance of fluid channels. The newer technology with solid-state catheters has more sensors at closer intervals, thus providing significantly greater anatomic detail than prior systems, including a possible differentiation of the internal and external sphincter, which was not achieved previously [13]. The HRARM and 3DHDM are technically easier to use and, once placed in the appropriate position, do not require significant manipulation with minimal sensor migration, thus improving accuracy. Recently, the 3DARM has allowed for more detailed understanding of the anal canal anatomy. Specifically, it was used to construct a model of the anal canal pressures in pediatric patients noting the longitudinal and radial asymmetry of the anal canal. Thanks to this technology, it is now known that the EAS contributes to distal canal resistance, while PR and IAS contribute to proximal canal [14].
Although these newer probes are exciting, they are much more expensive, require significant time for cleaning, have a shorter life span, and are temperature sensitive. As the HRARM and 3DHDM are relatively new devices, their utility and practicality have not been fully established, particularly in the pediatric population. It is hypothesized that it may be helpful in further understanding the anatomy particularly in those with anatomical anorectal disorders and improved planning for procedures in this area [15]. Several ongoing studies are hoping to investigate if these newer technologies at an increased cost translate into clinical relevance.
Methodological/Practical Aspects
The ARM can be done in children of any age; however only children (usually 5 years and older) are typically able to cooperate with the sensory testing (external and internal) and dynamic components of the test (squeeze and bear-down maneuvers). Thus for younger patients, the ARM is usually limited to the analysis of anal sphincter resting pressure and RAIR. In preparation for an ARM, patients are encouraged to defecate and empty the rectal vault prior to the study. If there is a suspected large stool burden, an enema or suppository is used to prevent stool interference. Typically, as infants have soft stool and enemas may be traumatic at this age, no preparation is necessary [16]. It is suggested that medications that may interfere with function such as opioids or anticholinergics are held during the testing.
To set up for the exam, the patient is placed in the lateral decubitus position, with knees drawn to the chest, thus both hips and knees flexed passed 90°. A digital rectal exam (DRE ) should be completed prior to the exam to evaluate the anatomy for abnormalities and gain a baseline assessment of the function of the area. It also provides a sense of the degree of stool burden and the extent of the patient’s ability to follow commands which is necessary during the study. Adult studies have shown that the digital rectal exam can produce findings that are comparable to the results from the ARM [17]. Prior to the digital insertion, the perianal area should be examined along with assessment of external perineal sensation and anal wink. A finger is then inserted into the rectal canal to evaluate resting tone, squeeze pressure, and defecation dynamics including the presence of a paradoxical puborectalis contraction on bear down.
After completion of the DRE , a lubricated manometry probe is inserted into the rectum. Once placed and in the appropriate location, it is held there for at least 90 s for the anorectal area to acclimate to the insertion prior to obtaining data. It is important to provide clear and detailed explanations during the study as the clinician’s verbal commands and clarifications have been shown to affect accuracy of results [18]. Helping the patient to relax by taking deep breaths or other techniques may be helpful in achieving a better baseline measurement.
Ideally the ARM study is completed in an awake patient without anesthesia or sedation, thus allowing voluntary and sensory testing. However, at times this is not feasible and anesthesia must be given, particularly in the toddler age. As above, one must be aware that this becomes a more limited study as these medications can alter the data. This should be accounted for when interpreting the study. It has been shown that ketamine and midazolam do not affect the sphincter pressure or RAIR response, while propofol decreases the resting sphincter pressure in a dose-dependent manner, although the normal RAIR is maintained [19–21].
Analysis
Baseline, dynamic, and sensory information can be obtained from an anorectal manometry study. Typically a complete study will assess sphincter pressure, bear-down maneuvers, sensation, and reflexes; however in specific situations, the test can be tailored toward particular questions. The following are the common assessments that are completed during the ARM study.
Resting basal pressure : After the patient is relaxed and comfortable with the probe in place, the basal resting sphincter pressure is obtained. This canal pressure measurement is comprised of mostly IAS tone (80 %) with some EAS pressure [22]. A low resting pressure could be indicative of weakness or disruption in the sphincter musculature. With the newer technology, the sphincter pressure can be measured with simple insertion of the catheter and obtaining data from the high-pressure zone. However, with water-perfusion manometry catheters, there are various methods employed. The most common of these is the station pull-through, when sensors are circumferentially arranged on the probe, or continuous withdrawal with spirally arranged sensors.
Squeeze: The squeeze pressure is used to assess sphincter strength/tone. It is produced by the patient voluntarily maximally tightening the anal sphincter and calculated as the highest pressure increase over the baseline resting pressure. This can be calculated as the average of three assessments. It is important to ensure that the intra-abdominal pressure is not increased during this exercise as it would alter the squeeze pressure data. A weak squeeze pressure may indicate myogenic or neurogenic causes (Fig. 10.2b).
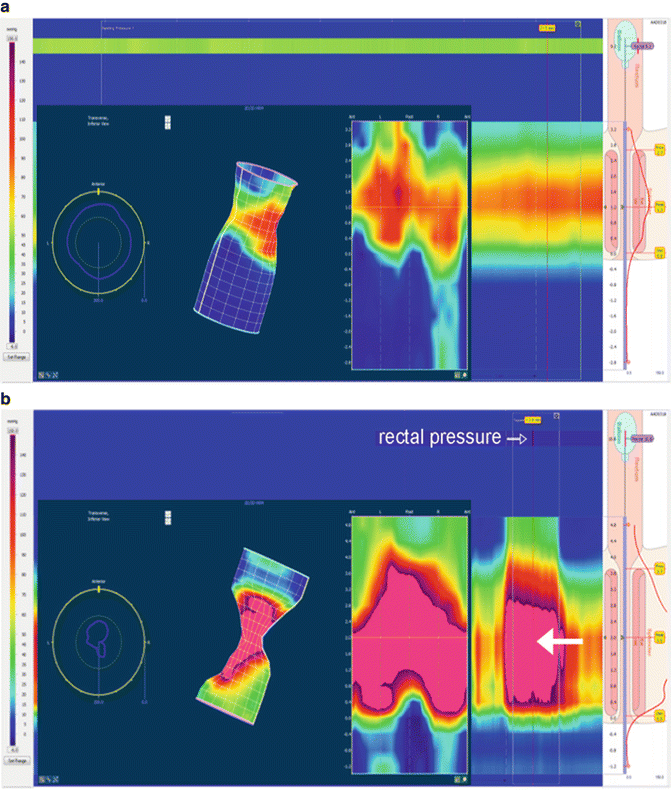





Fig. 10.2
(a) 3D: Resting (Baseline) anal canal during initial recoding. A moderate degree of increased sphincter pressure can be seen. This is often due to patient discomfort/anxiety. It is important to make sure the probe position does not cause discomfort and that the patient is allowed and encouraged to relax as much as possible. (b) 3D squeeze: Significantly increase pressure of sphincter (large white arrow), no pressure increase in abdomen and rectal balloon (rectal pressure, open arrow). (c) 3D bear down: Relaxation of the anal sphincter (black arrow), increase in pressure in the rectum (white arrow). (d) 3D dyssynergic defecation during bear down: Increased sphincter pressure (white arrow) in conjunction with only slightly increased rectal pressure (black arrow). (e) Paradoxical puborectalis: During the bear-down maneuver, a high-pressure area is seen above the sphincter (white arrow) in only the posterior aspect of the anal canal. This is the puborectalis sling which is not relaxing normally. The black arrow points toward the contracted sphincter which is below the puborectalis and is also seen in the anterior aspect of the canal
Anal canal length: The canal length is the measured distance between the anal verge and the location with ≥ 5 mmHg pressure increase over the rectal pressure.
RAIR: The rectoanal inhibitory reflex is obtained to assess the presence of the local enteric reflex. Most importantly, the absence of a RAIR suggests the presence of colonic aganglionosis or Hirschsprung disease. The reflexive relaxation of IAS is naturally caused by stool presence but is simulated during an ARM by rapid balloon inflation and deflation. To date, in pediatrics there is no universally agreed criteria for the presence of a RAIR, which has previously been defined as either a drop in pressure by >5 mmHg or >15 % of the resting pressure. There is typically a dose-related response with greater relaxation and duration of relaxation with larger balloon volumes (Fig. 10.3a). When conducting the test, the clinician must be aware of possible migration of the catheter out of the sphincter, particularly during WPM. Catheter migration may falsely indicate a RAIR response when there is none (Fig. 10.3b). This is the most common cause of a false-positive RAIR (an apparent anal canal relaxation is seen but falsely produced by the catheter migrating in and out of the sphincter region/high-pressure zone with balloon inflation by lack of digitally securing the catheter to the anal margin). The most common cause for a false-negative RAIR test (there is no anal canal relaxation seen, despite balloon insufflation) is a dilated rectum, often due to chronic stool retention. As the rectum is dilated, the balloon does not reach the needed volume to adequately stretch the rectal wall, needed to elicit an anal sphincter relaxation.




Fig. 10.3
(a) Dose-response RAIR 3D ARM. White arrows point to rectal balloon insufflation (which increases rectal sensor pressure). Anal canal relaxation (sphincter relaxation) is seen after each insufflation (black arrows). (b) WP RAIR. The black arrow signals balloon insufflation. The red bar was placed when catheter migration occurred, erroneously making the tracing appear as if anal canal relaxation had resulted from the balloon pressure on the rectum (seen in all four ports). This is a false-negative RAIR
Sensation: Testing the patient’s sensation is an important part of the ARM exam as it provides additional information regarding the patient’s perception of stool which can be indicative of anorectal dysfunction. Sensation is assessed in an awake, active participant (usually aged 5 years and older) by a gradual increase in balloon inflation size. First sensation is defined as the lowest balloon volume that is sensed by the patient. The urge sensation is the lowest balloon volume at which the patient develops the urge to defecate. Finally, the maximum tolerable sensation is the inflation size that is associated with severe urgency and pain. Decreased internal sensation is most often seen with a chronically dilated rectal canal due to persistent constipation.
Bear-down maneuver: The bear-down maneuver , or simulated defecation, is used to assess anorectal and pelvic floor pressure changes during attempted defecation. Similar to above, patients need to have the maturity to understand and cooperate with the testing. This ability is usually acquired around the age of 5 or 6 years. With normal defecation dynamics, there is an expected increase in rectal thrust pressure due to abdominal muscle contraction coordinated with a decrease in anal sphincter pressure. Patients in which these coordinated movements do not occur are thought to have dyssynergic defecation often resulting in outlet obstruction constipation [23]. Additionally, the puborectalis muscle can be visualized with the high-definition manometry, thus allowing for greater understanding of its contribution to defecation dynamics [24] (Fig. 10.2c).
Balloon expulsion: Once these assessments are complete, the probe is removed and a balloon expulsion test is performed. A balloon mounted on a plastic tube is inserted into the rectum and inflated to 50–60 cm3. Some centers use air while others use saline to inflate balloon. The patient is then instructed to sit on a commode and expel the balloon in privacy. The test is considered normal if the patient is able to expel the balloon within a defined time. In adults 1 min is allowed. It is not clear if this time limit is adequate in pediatrics, as well as the right amount of balloon inflation for children, although one series reports that adult volumes and time limit may be applicable [25]. The balloon expulsion test is considered an adjunct evaluation to the ARM to confirm the presence of dyssynergia [25].
Overall, anorectal manometry has been found to be a safe test with rare side effects. With insertion of any foreign object, there is the risk of colonic perforation; therefore care should be taken with placement and removal of probes. Additionally, the study should be delayed or terminated with any abnormal symptom or sign including significant bleeding or acute onset of severe pain.
Reference Values
In general, reliable and reproducible normative values for anorectal manometry are lacking in pediatrics. Although baseline data has been reported in various publications, lack of standardization of the ARM study, a different methodology, and equipment make comparing these values a difficult endeavor [7] (Table 10.1). Therefore, as concrete normative data is lacking in pediatrics, it is always important to correlate the findings with symptom presentation.




Table 10.1
References for normal manometric measurements
Technique | Healthy controls, N= | Ages | Anal resting tone (mmHg) | Rectal pressure (mmHg) | Anal canal length (cm) | Threshold of RAIR (mL) | Sensation threshold (mL) | Critical volume (mL) | Maximal squeeze pressure (mmHg) | |
|---|---|---|---|---|---|---|---|---|---|---|
Benninga [10] | WPM | 13 | 8–16 years | 55 ± 16 | 18 ± 10 | 19 ± 12 | 131 ± 31 | 182 ± 61 | ||
Hyman [26] | Not specified | 20 | 5–16 years | 67 ± 12 | 3.3 ± 0.8 | 140 ± 52 | ||||
16 | >5 years | 11 ± 5 | 14 ± 7 | 101 ± 39 | ||||||
Kumar [7] | WPM | 30 | <1 month (GA 34–39 weeks) | 31 ± 11 | 1.7 ± 0.3 | 10 ± 4 | ||||
30 | 1–16 months | 42 ± 9 | 1.9 ± 0.6 | 14 ± 10 | ||||||
30 | 18 month to 12 years | 43 ± 9 | 3.0 ± 0.5 | 25 ± 12 | ||||||
Li [27] | Not Specified | 10 | 5–15 years | 28 ± 11 | 117 ± 46 | |||||
Sutphen [28] | WPM | 27 | ∼7–12 years | 30 ± 12 | 96 ± 38 | 142 ± 47 | ||||
Benninga [29] | Sleeve, WPM | 22 | Neonates (PMA 30–33 weeks) | 32 ± 4a | 9 ± 2 | 1.6 ± 0.3b | ||||
De Lorijn [30] | Sleeve, WPM | 16 | Neonates (PMA 27–30 weeks) | 25 ± 11a | 7 ± 5 | 3.4 ± 1.6b | ||||
Tang [31] | HRARM | 180 | Newborn (GA 28–42 weeks), 1–85 days old | 29.7 ± 9.9 | 1.9 ± 0.5 cm | |||||
Banasiuk [32] | 3DARM | 61 | 2–17 | 83 (23) | 2.6 (0.68) | 15.7 (10.9) | 24.4 (23.4) | 191 (64) |
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree






