CHAPTER 26 Adjustable gastric banding
Step 1. Surgical anatomy
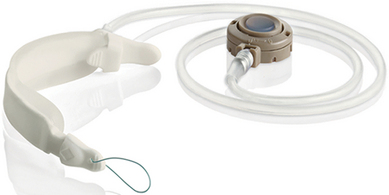
♦ Adjustable gastric banding was first introduced in 1993. Initially the Lap-Band was the only band available, now we have two types: the Lap-Band System by Allergan Health (Figure 26-1) and the Realize Band by Ethicon Endo-Surgery (Figure 26-2).
♦ The first landmarks to establish are the location of the gastroesophageal junction and the angle of His. Often there will be a large gastroesophageal fat pad, which obscures the location of the gastroesophageal junction. The fat pad will need to be dissected away to identify the gastric serosa.
♦ Once the gastroesophageal junction is identified, then the presence of a hiatal hernia can be determined. If present, a hiatal hernia will need to be repaired to avoid future dysphagia and failure of the band.
♦ The hepatogastric ligament, which is part of the lesser omentum, connects the liver with the lesser curve of the stomach. It consists of a caudal flaccid portion known as the “pars flaccida,” which is usually transparent and contains no vessels. The right-sided dissection begins here, and there is usually no need to dissect in the more cranial portion of the hepatogastric ligament known as the “pars densa.” The pars densa should be avoided when possible because it contains the hepatic branch of the vagus nerve and an associated artery. If there is a replaced left hepatic artery, it will be located in this region and must be considered while dissecting in this region because it is often obscured by overlying fat.
♦ Once the pars flaccida is opened, the right diaphragmatic crus can be exposed. Proper identification of the right crus is critical to ensure safe dissection into the retrogastric space. Proper technique and placement of band will help the surgeon to avoid entering the lesser sac.
♦ A perigastric dissection occurs along the lesser curve of the stomach and requires meticulous tissue dissection. This approach may be utilized in cases when there is excess fat along the lesser curve, large accessory or replaced vessels, and poor visibility of the right crus.
Step 2. Preoperative considerations
Patient preparation
♦ The indications and contraindications for an adjustable gastric band are the same for all bariatric surgery patients.
♦ Preoperative assessment by a multidisciplinary team is required. The team should consist of the following: the bariatric surgeon, internists, endocrinologists, pulmonary staff, and cardiology staff, as well as consultation with nutritionists and psychological evaluation. The assessment is based on the patient’s individual needs.
♦ High body mass index (BMI) >50, advanced age, insulin resistance, and poor health are associated negative predictors but are not contraindications to banding procedures.
♦ Patients with a history of esophageal disorders or gastroesophageal reflux should undergo an upper GI contrast study, endoscopy and manometry. Any patient with a documented significant esophageal dysmotility disorder should not have a banding procedure.
♦ Preoperative weight loss is helpful in reducing injury to the liver, reducing operative time, and preparing the patient for postoperative dietary guidelines. Severely obese patients with BMI >50 are recommended to lose >10% of excess weight.
Equipment and instrumentation
♦ Three 5-mm bladeless trocars and one 15-mm bladeless trocar (the 15-mm trocar allows safe and easy passage of the band into the abdomen)
♦ Iron Intern with Nathanson liver retractor
♦ Foot-operated hook cautery for most cases (for patients with excess around the lesser curve and gastroesophageal junction, hand-operated ultrasonic shears are recommended)
Anesthesia
♦ DVT prophylaxis is recommended in all patients undergoing bariatric surgery. Consensus on mechanical versus pharmacologic versus combination has not been reached. No prospective randomized studies are available. I recommend using a combination of sequential compression devices and 5000 units of unfractionated heparin or 30 mg of low-molecular-weight heparin given subcutaneously 1 hour preoperatively and early ambulation postoperatively.
♦ Patients with history of DVT and Pulmonary embolism (PE) should be considered for prophylactic vena cava filter as well as patients with pulmonary hypertension, obesity hypoventilation syndrome, and a BMI >60.
♦ Antiemetics are recommended to reduce vomiting and potential postoperative band prolapse.
♦ Gastric decompression with NGT or calibration tube will allow easy visualization of anatomic landmarks.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree