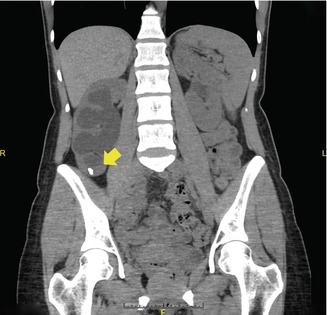
Fig. 21.1
Axial CT scan image demonstrating 2 cm right renal stone (yellow arrow) that was not previously visualized on KUB. Following surgery, the stone analysis revealed a uric acid stone
Ureteral Stones
Ultrasound imaging is helpful in finding renal stones, bladder stones and stones at the ureterovesical junction. In the remainder of the ureter, ultrasound is a poor imaging modality for stone localization. Without contrast, Spiral CT scan is the best imaging choice to visualize stones along the course of the ureter (Fig. 21.2). With contrast, the use of intravenous contrast (IVP) or retrograde pyelogram (RUG) can help to identify ureteral stones, especially if the stones are radiolucent. In addition, lithotriptors using fluoroscopy as a sole imaging device cannot be used to localize radiolucent ureteral stones. IVP and RUG during ESWL can also provide useful information for stone localization.
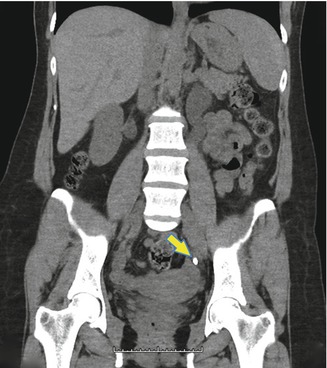

Fig. 21.2
Coronal CT scan image of a left ureteral stone (yellow arrow)
Difficult Stones to Fragment
Some renal calculi are refractory to ESWL therapy. The fragility of stones in descending order is: Cystine, brushite, calcium oxalate monohydrate (COM), hydroxyapatite, struvite, calcium oxalate dihydrate (COD), and uric acid. There is poor fragmentation of Cystine and brushite as these are the most ESWL resistant stones (Fig. 21.3). As a general rule, ESWL resistant stones (i.e., brushite, cystine, COM) should only be treated with ESWL when they are small (<1.5 cm) and larger stones preferentially treated with PCNL or ureteroscopy with Holmium:YAG (Ho:YAG) laser lithotripsy.
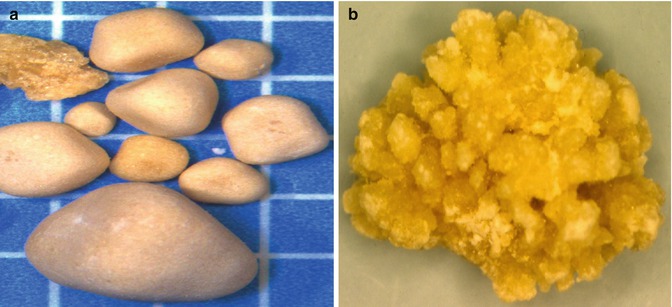

Fig. 21.3
Cystine (a) and brushite (b) stones (Courtesy of Louis C. Herring & Co., Orlando, FL)
In rare circumstances, the very soft matrix calculi are also ESWL resistant. These radiolucent stones, often associated with urea splitting bacteriuria, are composed of as much as 65 % organic matter (compared to 2–3 % organic matrix in most non-infected urinary calculi). ESWL is not effective in treating matrix stones which are ideally treated with PCNL.
Difficult Stones to Access
Ectopic Kidney
An ectopic kidney is a congenital anomaly where the kidney is located above (thoracic), below (pelvis) (Fig. 21.4) or even the opposite side (crossed) of it’s normal position (See Fig. 21.5). The occurrence of ectopic kidney is approximately 1:2,200–3,000 people. Although these kidneys are not in the usual position, an ectopic kidney does not usually present with any symptoms. An ectopic kidney is usually discovered when imaging studies are done for other reasons. The diagnosis of an ectopic kidney is identified on renal ultrasound, CT scan, MRI, renal scan, VGUG or IVP. The location of the kidney and positioning problems of the patient on the operating room table may make ESWL a difficult choice for treatment. Alternative modalities, including ureteroscopy, PCNL and even open surgery may be required.
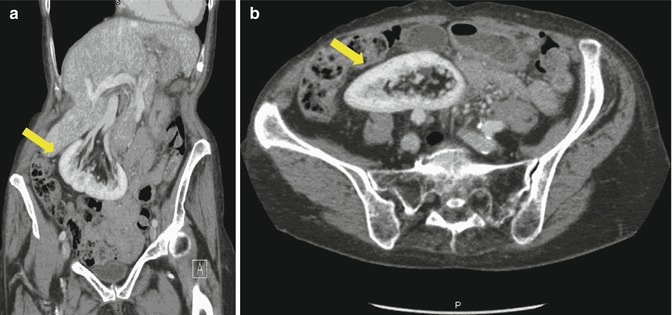
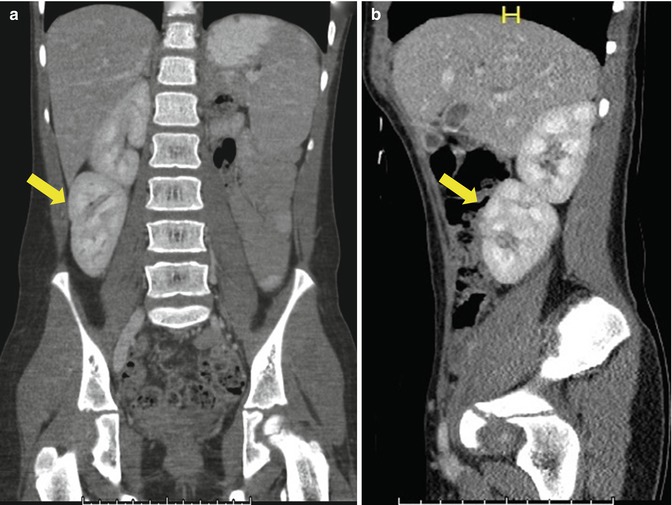

Fig. 21.4
Coronal (a) and (b) axial (b) CT scan images demonstrating a malrotated pelvic kidney (yellow arrow)

Fig. 21.5
CT scan coronal (a) and sagital (b) views of a crossed fused renal ectopia. The crossed kidney (yellow arrow) lies underneath the native right kidney
Ureteropelvic Junction Obstruction
The section of the urinary tract where the pelvis of the kidney meets the ureter is called the ureteropelvic junction. A blockage at this location is called a ureteropelvic junction obstruction (UPJO), where there is an interruption in the urine flow from the renal pelvis to the ureter (Fig. 21.6). The blockage seen in UPJO is thought to be caused by a congenital narrowing of the ureteropelvic junction or less commonly by compression of the ureteropelvic junction by a crossing blood vessel to the kidney. The blockage can be partial or complete with varying degrees of severity. The incidence of UPJO occurs in approximately one in 1,500 children. The male-to-female predominance is greater than 2:1, with the left kidney effected about twice as often as the right. Bilateral UPJO are seen in 10–40 % of cases. Ureteropelvic junction obstruction (UPJO) in adults is commonly associated with urinary stones. The treatment strategies for UPJ obstruction have seen a significant shift in the last several years. The majority of surgical treatments for UPJ obstruction include laparoscopic pyeloplasty, open pyeloplasty, endopyelotomy, endopyeloplasty, and robotic-assisted laparoscopic pyeloplasty. Percutaneous approach is a good alternative to render a patient stone-free and treat ureteropelvic junction obstruction. The nephrostomy tube access for these stones allows simultaneous removal of stones and repair of the UPJ obstruction.
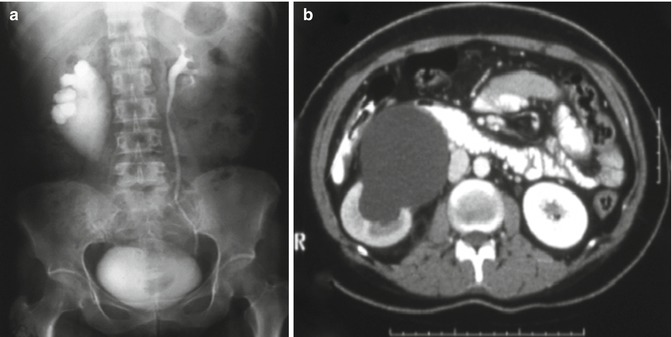

Fig. 21.6
IVP (a) and axial CT scan (b) images demonstrating a right UPJO and normal left kidney
Horseshoe Kidney
A horseshoe kidney is the most common congenital fusion anomaly in the urinary tract (See Fig. 21.7). Typically, the ureter is attached to the kidney at a higher point, called a high insertion, and is anteriorly placed (in front of the kidney) instead of the normal medial location (toward the midline). Approximately up to two-thirds of patients with horseshoe kidney may experience hydronephrosis, infection or kidney stones. The results with ESWL are poor. Alternatively, small stones (<1.5 cm) can be approached with ureteroscopy and laser lithotripsy. Larger stones (>1.5 cm) can be treated by PCNL.
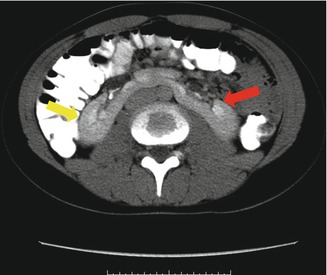

Fig. 21.7
Axial CT scan view of horseshoe kidney demonstrating the right (yellow arrow) and left (red arrow) kidneys connected in the middle
Renal Calyceal Diverticula
Calyceal diverticula are thin-walled cystic cavities located in the peripheral to an otherwise normal calyx, which communicate through a narrow channel. They are lined by transitional epithelium, which is the same tissue that lines the urinary tract. These cysts may originate from embryogenesis, blunt renal trauma or obstruction. They occur in any part of the kidney, but usually originate from an upper pole calyx. Calyceal diverticula are found in both males and females. Renal diverticula may present with a renal stone (Fig. 21.8). The incidence of stone formation in renal calyceal diverticula present in 9.5–39 % and approximately one-third of cases become symptomatic. These stones may include calcium oxalate, calcium phosphate or carbonate apatite. Treatment of these diverticular stone with ESWL is controversial and it can be done when the stones are small and the diverticular neck is patent. Otherwise, ureteroscopy and laser lithotripsy and PCNL are better treatments of choice.