Fig. 7.1
Critical view of safety: gentle grasper traction exposes structures in Calot’s triangle
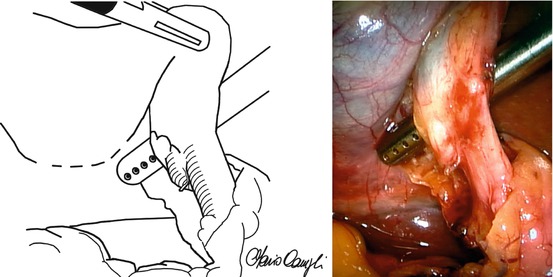
Fig. 7.2
Underpassing cystic duct and artery to obtain the critical view of safety avoids bile duct injuries
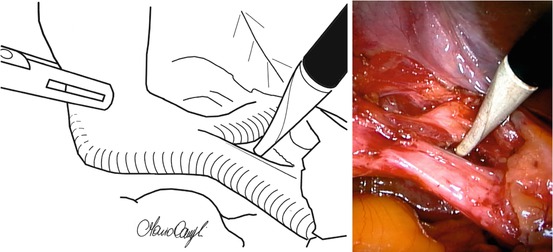
Fig. 7.3
Accurate isolation of each anatomical structure
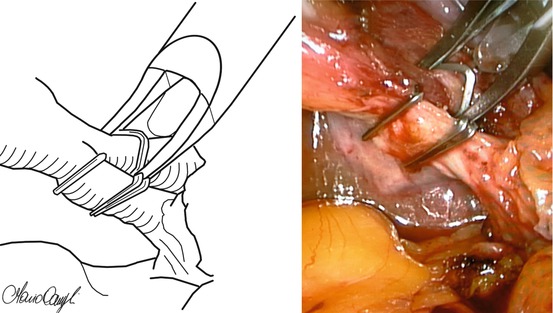
Fig. 7.4
Clipping and dividing structures in Calot’s triangle only after a clear identification
7.1.4 About Conversion
Despite the advances in training and increased clinical experience, conversion rates reaching 10 % are still reported [22] (LoE4). Needful prompt conversions are mandatory to avoid complications, but few studies have investigated the causes of conversion. Lengyel et al. recently claimed that conversion, in many circumstances, is performed “electively” due to an “anticipated” difficulty, with a longer hospital stay and higher costs [23] (LoE4) [24] (LoE3). Furthermore, to identify the timing and the main reasons for conversion, they concluded that the conversion was elective in 91 % of the examined cases. In about half of these cases, conversions were performed without a genuine attempt at laparoscopic dissection and the inserted trocars were fewer than four [22] (LoE4). Despite, several limitations of the study (small sample size, degree of laparoscopic training, experience of the surgeons), the authors believe that all laparoscopic cases should be genuinely attempted, the correct number of ports placed, and some effort made at dissection. With decreasing experience in open cholecystectomy, this procedure does not always seem to be a “safe” alternative.
7.1.5 Partial Cholecystectomy
In the case of a difficult LC (e.g., in acute cholecystitis wherein dissection of Calot’s triangle is challenging due to severe adhesions or inflammation), a change in surgical strategy such as anterograde or partial cholecystectomy or even drainage may be more practical than conversion. Since surgical skill and experience play an important role, a different surgical strategy may be especially valuable for less experienced surgical teams. An alternative approach to conversion aimed at preventing BDI is laparoscopic partial cholecystectomy (Fig. 7.5). The safety and efficacy of this procedure are unclear. Literature concerning LPC is poor. Henneman et al. [25] (LoE3), in 625 patients suffering from acute cholecystitis who received partial (subtotal or incomplete) cholecystectomy, reported a median hospital stay of 4.5 days and one case of BDI. Without firm conclusions, closure of the remnant gallbladder pouch, cystic duct, or both seems favorable, minimizing the need for ERCP, reducing the amount of leaks and the associated hospital stay, and lowering the rate for recurrent symptoms of gallstone disease and for the risk of BDI. Also Davis et al. in a recent retrospective case-control study evaluated this technique in a series of patients with acute cholecystitis. They reported a half postoperative complication with no BDI after this strategy, suggesting partial cholecystectomy as an alternative approach to conversion. Furthermore, this technique with removing necrotic portions of the gallbladder may prevent empyema formation [26] (LoE4).
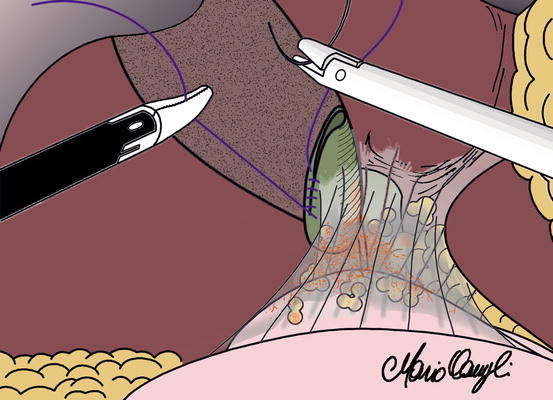

Fig. 7.5
Partial cholecystectomy
7.1.6 Intraoperative Management
A single-institution retrospective analysis of a large series of patients with diagnosis of BDI sustained during LC was recently published where 88 % of the patients receiving on-table repair during surgery had a favorable evolution. The authors concluded that the intraoperative diagnosis of BDI is a very important topic with lower morbidity and mortality rates [27] (LoE4). Even though only case series and expert opinions in management were published in the medical literature, there is a growing body of literature supporting the importance of early referral to a tertiary care hospital to treat BDI with a multidisciplinary approach [28–31] (LoE4) [32] (LoE3) [33] (LoE2). And so the EAES guidelines [21] recommend that “nevertheless no high-quality evidence dealing with this question was identified from clinical studies, the management of BDI should be performed by surgeons who are experienced in this field.”
7.2 Abscesses
The incidence of abscesses in LC is very low. In a large national survey of 77604 LCs [34], the reported abscess incidence was 1/13,000 complications. Bile leakage and gallstone spillage remain the most frequent causes of abscesses after surgery [35–45] (LoE4) [46] (LoE3). Untill now only case reports or case series are published in examined literature, and therefore it was not possible to perform a systematic review according to the criteria of the best evidence-based literature.
7.2.1 Incidence
The incidence rate of unretrieved gallstones in the peritoneal cavity is high (2.4–50 %) [43, 47] (LoE4) [48] (LoE3); nevertheless severe complications are rarely described. The incidence of infection-related complications was reported in 0.1–0.3 %. Abscesses were generally located in the abdominal wall or in the subhepatic space, but less frequently anywhere in the abdomen and more likely in the setting of acute cholecystitis [49] (LoE3).
7.2.2 Management
In a retrospective analysis on 10,174 LCs, only 0.08 % required reoperation for abdominal abscess with no mortality. Since gallbladder perforation and stone spillage occur during the dissection (75 %) or the removal (25 %) of the gallbladder, caution in removing from the hepatic fossa is suggested, avoiding hurried traction to Hartmann’s pouch [46] (LoE3). Less frequent causes include gallstone spillage during gallbladder retrieval across the umbilical port, especially if it is not recovered in an endobag, and so the use of this device is recommended [46] (LoE3). The number and the size of lost stone seem to be a risk factor for abscess growth. More than 15 stones or stones larger than 1.5 cm were found in more than 40 % of these patients [46] (LoE3). The kind of the stones seems to be an important factor: in the pigmented-type stones (black, brown, mixed), bacterial contamination was present in 83 % compared to 33 % in cholesterol calculi [46] (LoE3). It is suggested to send a sample of bile and/or a retrieved stone for microbiological analysis, because pathogens are usually the same as those that cause subsequent infections [46] (LoE3). Extensive peritoneal lavage is widely recommended, but care must be taken to not spread gallstones into more inaccessible sites, making retrieval even more difficult. Placing the irrigating instrument beyond the stones so that they are flushed into view can be helpful [48] (LoE3). Authors emphasize the need for removal of as many calculi as possible during laparoscopy [50] (LoE3). However, they advised conversion to an open procedure only in patients with too many gallstones left in the peritoneal cavity, especially when bacteriobilia is suspected or confirmed by Gram stain of the bile. They also noted that percutaneous drainage of intra-abdominal abscesses in most of the patients was ineffective if the inciting gallstones were not removed [50] (LoE3). There is no indication for converting the laparoscopic procedure to a laparotomy purely on the basis of spilled stones, but documenting spilled stones in the operation note and informing the patient about stones’ spillage and its unlikely consequences should be useful. The surgeon should be alert to the possibility of abscess formation and other complications because early recognition of intraperitoneal gallstones is essential in the diagnosis and further treatment of symptomatic patients [45] (LoE4).
7.2.3 Antibiotic Prophylaxis and Therapy
In a recent Cochrane Systematic Review [51] (LoE1), Sanabria et al. concluded that there is no sufficient evidence to support or refuse the use of antibiotic prophylaxis to reduce surgical infections in low-risk patients undergoing elective LC.
In a recent randomized trial of 166 patients who suffered from accidental perforation of the gallbladder during elective LC, there was no significant association between antibiotic treatment and surgical wound infection [52] (LoE2). No patients developed residual abscess. In a multivariate analysis, diabetes mellitus, age over 60, operation time lasting more than 70 min, and ASA 3 were identified as independent factors significantly associated with the onset of surgical wound infection (p < 0.001) [52] (LoE2). The authors concluded that routine administration of an antibiotic to patients experiencing accidental perforation of the gallbladder during LC is not necessary. They recommend antibiotic prophylaxis, immediately before surgery, for patients with associated risk factors [52] (LoE2).
7.3 Hemorrhages
Vascular injuries during LC may more often occur during dissection of the Calot’s triangle structures [53] (LoE4) [54] (LoE3). Unfortunately the clinical relevance and impact of vascular injuries may be dramatic for the surgeon and above all for the patient. The knowledge of the mechanism by which hemorrhages occur represents a fundamental way to diminish the risk of incontrollable bleeding during LC.
Recent literature still reports incidence data derived from systematic studies of the 1990s: the small number of cases and the wide extent of the confidence interval do not permit to obtain reliable updated incidence rate of bleeding in LC; furthermore, there is no uniform classification about major or minor bleeding. Maybe the real incidence of relevant hemorrhages during LCs is underestimated [54, 55] (LoE3).
Copious bleeding from the liver bed accounts for about 88 % of hemorrhages during LC [54] (LoE3) [56] (LoE4), while the right hepatic artery (RHA) injuries represent less than 12 % of cases [57, 58] (LoE3), with an overall rate of uncontrollable hemorrhages requiring open conversion ranging from 0.1 to 8 % [56, 59] (LoE4) [54, 60] (LoE3) (Fig. 7.6). Coagulation defects may be responsible for uncontrollable hemorrhage, and preoperative blood assessment must be carefully evaluated, and caution must be posed about the use of nonsteroidal anti-inflammatory drugs because of enhanced bleeding diathesis from poor platelet adhesiveness [61] (LoE4). Higher bleeding rate is reported in cirrhotic patients (26 vs 3.1 % in not cirrhotic patients) because of damaged liver function [62] (LoE3).
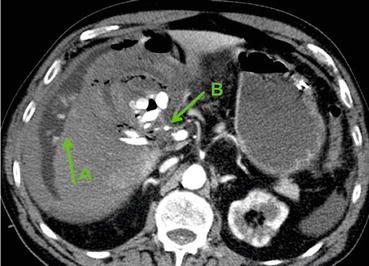

Fig. 7.6
Severe postoperative hypotension after LC: large perihepatic hematoma (A) and active bleeding of the gallbladder bed (B) (Courtesy of G. Gualdi – “Sapienza” University, Rome)
The common hemorrhage of the liver bed is often a borderline condition depending on the different caliber of the involved vessels. It frequently comes from small vascular branches so that direct pressure to the gallbladder bed via a laparoscopic instrument may arrest the hemorrhage [63] (LoE4), but surgeons have to keep in mind that a middle hepatic vein or an aberrant cystic artery (CA) may be also involved [63–65] (LoE4). The portal vein injury, often associated with hepatic artery injury (HAI), is the third highest ranking injury, although it is considerably less common (4 %) [66] (LoE4) [67] (LoE3).
CA bleeding may become a serious complication during LC, with an increasing risk of overlap vascular or biliary structures injuries, that may impose conversion to open surgery. The CA has many possible position, number, and origin with the RHA being the most common, and the knowledge of anatomical variations of the CA may help the surgeon to avoid hemorrhage [68] (LoE4).
The RHA, which is located in 82 % of the cases in the Calot’s triangle ([69] Atlas), is the most common major vascular structure damaged during dissection of this anatomic space (90 %) [58] (LoE3). Stewart et al. [66] (LoE4) described how the RHA may be misidentified as the CA. The source of the error depends upon the common bile duct incorrectly identified as the cystic duct: in this case the transection of the common bile duct exposes the RHA, which is often clipped, based on the wrong assumption that it is a posterior CA. These mistakes emphasize the importance of identifying the CA and dividing it close to the gallbladder. The “fundus-first” technique, suggested for acute cholecystitis [70] (LoE4), may lead to a possible injury to the RHA, which might be retracted downwards, along with the gallbladder [71] (LoE4). For incontrollable hemorrhage, even if only few data are available on the real incidence of bleeding complications, the rate of conversion to open surgery was reported in about 8 % of the cases (meta-analysis from 39 studies for a total of 15,596 patients) [60] (LoE3).
Among patients with bile duct injury (BDI) during LC, the incidence of RHA injury was reported from 12 to 25 % [34] (survey) [71] (LoE4). Higher incidence was reported in the review by Pulitanò and colleagues [58] (LoE3) where 38 % of cases were combined with HAI. In cases of BDI and concomitant HAI, the arterial supply to the bile duct is often completely interrupted, further increasing the risk for potential ischemic stricture of the remaining right biliary tree as well as a high risk for hepatic necrosis. The sensitivity of the bile duct to ischemic injury is well described and might contribute to the increased morbidity after biliary reconstruction [58] (LoE3).
7.3.1 Hemostatic Agents
Many adjunctive local hemostatic agents are frequently proposed to favor bleeding control in liver surgery, but no strong evidence exists about their real efficacy during LC. Because their actual effectiveness is not yet extensively studied in large randomized, controlled prospective studies, the current indications for usage, both in hemorrhage and bile leakage, are not clear and mostly based on the individual surgeon’s preference. Routine use of local hemostatic agents is not recommended.
7.4 Bowel Injuries
The incidence of all bowel injuries (BI) during LC is very low, and it was reported in literature from 0.07 to 0.5 % [54, 72, 73] (LoE3), but excluding lesions for trocar insertion or Veress needle, the specific LC-related causes are seldom referred and ascribe mainly to dissection, adhesiolysis [54] (LoE3), electrocautery burns, and tearing during retraction [74] (LoE4). BI comprise a severe complication when they do occur and may remain undetected during the operation [54] (LoE3). The injuries most frequently involve the small intestine, followed by the colon, duodenum, and stomach [75] (Chapter of book). Careful patient selection, control of the integrity of the isolation of the instruments, and no out-of-sight activities can diminish overall complication rates. Limited injuries to serosa may not require any treatment [76] (LoE4), while full-thickness lesions need immediate repair either laparoscopically [73] (LoE3) or with conversion to laparotomy. Since bowel injuries may remain undetected during the operation, any patient with signs of peritonitis, sepsis, or increased abdominal pain after laparoscopic surgery must promptly be investigated [72] (LoE3).
References
1.
2.
3.
Wherry DC, Marohn MR, Malanoski MP et al (1996) An external audit of laparoscopic cholecystectomy in the steady state performed in medical treatment facilities of the Department of Defense. Ann Surg 224:145–154PubMedCentralPubMedCrossRef
4.
Richardson MC, Bell G, Fullarton GM (1996) Incidence and nature of bile duct injuries following laparoscopic cholecystectomy: an audit of 5913 cases. Br J Surg 83:1356–1360PubMedCrossRef
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree






